Professional Documents
Culture Documents
Testing Procedure Ultrasound
Uploaded by
MitecCenememOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Testing Procedure Ultrasound
Uploaded by
MitecCenememCopyright:
Available Formats
TESTS PERFORMED
DEAD ZONE (RING-DOWN RAMP) (Figure 1) Description and Reason For Testing The dead zone is the distance from the front face of the transducer to the rst identiable echo below the transducer/ phantom interface. The dead zone occurs because an imaging system cannot send and receive a signal at the same time. Therefore, no clinical data can be collected in this region. However if artifacts are noted within the dead zone, they may indicate uctuations in the input power to the system. The depth of the dead zone depends upon the frequency (higher frequency decreases the depth of the dead zone) and performance of the transducer and the pulsing/receiving section of the system. Testing Procedure
1. Scan the phantom until the dead zone target group is 2. The rst target is positioned 1 or 2 mm below the scan
surface. Subsequent targets are spaced 1 mm apart. Refer to the individual Model specications for specic details on this target group. Using the electronic calipers, measure the distance between the rst target imaged and the echo produced by the scan surface. The resulting value will be the depth of the dead zone. Document the depth measurement on the quality assurance record. clearly displayed. Freeze this image.
3.
4.
Results The system's dead zone should remain consistent from week to week when using the same instrument settings and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability
Figure 1
Geometric Accuracy - Vertical Measurement Calibration (Figure 2)
Description and Reason For Testing Vertical distance measurements are obtained along the axis of the sound beam. Accurate representation of the size, depth and volume of a structure is a critical factor in a proper diagnosis. Most imaging systems use depth markers and/or electronic calipers to obtain these measurements. The phantom is scanned and a distance measurement obtained using the timing markers and/or electronic calipers. The resulting measurement is then compared to the known distance between the line targets in the phantom. The accuracy of vertical distance measurements depends on the integrity of the timing circuitry of the imaging system. Vertical distance errors are far less likely to occur than horizontal errors. It is important to verify that the phantom has been allowed to reach temperature equilibrium with ambient room temperature, nominally 23C. If room temperature varies excessively from
23C, distance measurement error will be introduced. Thermal gradients within the phantom may also introduce measurement error. Testing Procedure Position the transducer over the vertical group of line targets until a clear image is obtained. Freeze the display. 1. Using the electronic calipers or the timing markers measure the greatest distance that can be clearly imaged between line targets. 2. Document the measurement obtained on the quality assurance record. Results The system's vertical distances measurements should remain consistent from week to week when using the same instrument settings and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability to resolve these targets, corrective action should be considered.
Figure 2 Geometric Accuracy - Horizontal Measurement Calibration (Figure 3)
Linear Horizontal Group, Sector Horizontal Group Description and Reason For Testing Horizontal distance measurements are obtained perpendicular to the axis of the sound beam. Proper diagnosis depends on the accurate representation of the size and volume of a structure being examined. Most imaging systems use distance markers and/or electronic calipers to obtain these measurements. The phantom is scanned and a distance measurement obtained. The resulting measurement is then compared to the known distance in the phantom. The accuracy of the horizontal distance measurements depends on the integrity of the transducer scanning assembly, the output intensity and the resolution of the imaging system. It is important to verify that the phantom has been allowed to reach temperature equilibrium with ambient room temperature, nominally 23C. If room temperature varies excessively from 23C, distance measurement error will be introduced. Thermal gradients within the phantom may also introduce measurement error. Testing Procedure Note: Due to the geometry and variety of sector scan transducers a separate set of horizontal line targets are provided to evaluate the horizontal distance. Please refer to the specication page for the location of these groups Models 539 & 535 phantom provides two scanning surfaces used to evaluate horizontal measurement calibration. Model 570 & 549 have two or four sets of horizontal targets (linear/sector) at different depths..
1. Position the transducer over the horizontal group of line 2. Using the electronic calipers or the timing markers measure 3.
the greatest distance that can be clearly imaged between line targets displayed. Note: Some sector scanners have distance markers on the outside edges of the sector image with no other indicators available. Hand-held calipers must be used for distance measurements within the image on the monitor. Document all of the measurements on the quality assurance record. targets until a clear image is obtained. Freeze the image.
4.
Results The system's horizontal distance measurements should remain consistent from week to week when using the same instrument settings and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability to resolve the correct spacing of these targets, corrective action should be considered.
Figure 3
Axial - Lateral Resolution Arrays (Figure 4)
Description and Reason For Testing Axial resolution is the minimum reector separation between two closely spaced objects which can be imaged separately along the axis of the beam, whereas lateral resolution denes the systems ability to image objects separately that lie perpendicular to the axis of the sound beam. If a system has poor resolution capabilities, small structures lying close to each other will appear as one image, causing improper interpretation of the ultrasound ndings. Axial Resolution depends on the transducers center frequency, damping characteristics and pulse length. Generally, the higher the frequency the better the systems axial resolution. Lateral resolution is approximately equal to beam width, and varies with depth, focusing characteristics of the transducer, number of displayed scan lines and the systems sensitivity and gain settings. Testing Procedure The locations in the phantom are referenced from the rst axial target. Refer to the individual Model specications for specic details on this target group.
1. Position the transducer over the axial-lateral resolution
group of line targets on the phantom until a clear image is obtained. Freeze this image. 2. Examine the image to determine if all of the line targets within the group are clearly displayed as separate target points. Record the closest spaced target points which can be imaged (refer to specication drawing). Obtain a hard copy of the display. 3. Document all observations made on the quality assurance record. Results The system's ability to resolve the array targets at given depths should remain consistent from week to week when using the same instrument settings and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability to resolve these targets, corrective action should be considered.
4 mm 3 mm 2 mm 1 mm 5 mm 4 mm 3 mm 2 mm 1 mm
Lateral Resolution Array Sensitivity (Maximum Depth of Penetration) (Figure 5) Description and Reason For Testing
Axial Resolution Array
5 mm
Figure 4 1. Position the transducer over the largest group of anechoic 2. 3. 4. 5.
targets. Refer to the individual Model specications for specic details on this target group. Freeze image and obtain a hard copy. Examine the image to determine the last or deepest target structure displayed. Using the electronic calipers or the timing markers, measure the depth of this target. This test should also be performed with output levels set at the highest and lowest settings. This enables any changes in output to be more easily detected. Document the depth measurement on the quality assurance record.
The ability of an imaging system to detect and display weak echoes from small objects located at specied depths (penetration) is referred to as sensitivity. Clinically, weak reecting echoes are commonly produced from internal structures of organs. Denition of these structures can be extremely important in the interpretation of the ultrasound ndings. Sensitivity can be affected by the pulser/receiver section of the system, the degree of focusing of the transducer, attenuation of the medium, depth and shape (geometry) of the reecting object, and electromagnetic interference from the local surroundings. A systems maximum depth is limited by output power, TGC, gain, transducer frequency, focal depth, number of scan lines and electrical noise. Testing Procedure
Results The system's depth of penetration should remain consistent from week to week when using the same instrument settings and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability to resolve these targets, corrective action should be considered.
Functional Resolution (Figure 5)
Description and Reason For Testing Functional resolution is an imaging system's ability to detect and display the size, shape, and depth of an anechoic structure within the test phantom. In practice, the data obtained will give a direct indication of the minimum size structure the system is capable of resolving at a given depth. Denition and Fill-in describes the imaging system's ability to detect and display the shape and echogenic characteristics of a structure. Clinically, a correct diagnosis is dependent upon the system's ability to differentiate between a cystic or solid structure versus echo patterns originating from the surrounding normal tissue. Testing Procedure
1. Position the transducer over the anechoic target structures until a clear image is obtained. 2. Freeze image and obtain a hard copy. 3. Examine the image to determine the rst and last target in each size group displayed. 4. Record the range of depths visualized for each group. Due to the conguration of the sound beam small targets in the near eld may not be imaged. 5. Document all ndings on the quality assurance record. Results The system's functional resolution should remain consistent from week to week when using the same instrument settings, transducers and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability to resolve these targets are observed, corrective action should be considered.
Figure 5
Image Uniformity Description and Reason For Testing Image non-uniformity can mask subtle changes in the tissue texture, which may increase the risk of false negative diagnoses. Imagine uniformity can be affected by side lobes in the transducer beam, electrical noise, and problems in the imaging processing hardware. Some artifacts can be the result of transducer malfunction, poor electrical contacts, failure in the image processing and/or systems software, and poor acoustic coupling between the transducer/patient interface causing the introduction of reverberation and banding. Horizontal bands are often caused by reections from interfaces or circuitry and focusing problems while vertical bands may indicate a damaged transducer element. Testing Procedure defect in a particular region of the phantom. If the artifacts are still present, note the gain settings, gray scale level and focal setting and document with a photograph. Repeat the scan using a different gain and focal setting. 4. Document all ndings on the quality assurance record. Results The system's image uniformity should remain consistent from week to week when using the same instrument settings, transducers and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates major areas of image non-uniformity corrective action should be considered.
1. Position the transducer over an area of the phantom which 2. Take particular care to ensure the transducer is properly 3. Scan this region to determine if there are any areas of nonuniformity or artifacts. If demonstrated, repeat the scan at a different location using the same phantom to rule out a coupled to the phantom. is relatively free of target structures.
GRAY SCALE & DISPLAYED DYNAMIC RANGE - (Figure 6) Description and Reason For Testing Gray scale or gray scale processing uses the amplitude of the echoes received to vary the degree of brightness of the displayed image. The adjustment of the echo signal required to go from a just noticeable (lowest gray scale level) echo to the maximum echo brightness is referred to as the displayed dynamic range. Clinically, gray scale processing and displayed dynamic range allow echoes of varying degrees of amplitude to be displayed in the same image. Test Procedure
2. Freeze image and obtain a hard copy. 3. Examine the image. The targets should appear circular in 4.
shape, with clear sharp edges and vary in the degree of brightness ranging from low to high levels of contrast. All ndings should be documented on the quality assurance record.
Results This target group varies in echogenicity and provides a good indication of the performance of the gray scale processing and displayed dynamic range. The system's gray scale processing should remain consistent from week to week when using the same instrument settings and phantom. Compare the test results obtained from the baseline records. If the current image demonstrates changes in the system's ability to resolve these targets, corrective action should be considered.
1. Position the transducer over the gray scale target group
until a clear image is obtained. Refer to the individual Model specications for specic details on this target group.
Figure 6
2D/3D Calibration - (Figure 7)
! Description and Reason For Testing! Ultrasound imaging systems may detect differences in echogenicity of tissue structures and determine the dimensions of those structures based on user or automated boundary detection. Spatial measurement data collected will give an indication of the accuracy the system is capable of. Testing Procedure
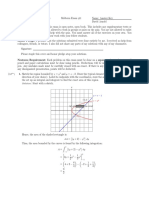
Using the 2D shapes shown in the target diagram in Figure 7, areas and perimeters may be determined by connecting lines between the lament targets. Linear measurements are taken from an image which is on a plane perpendicular to the line targets. For ultrasound systems which have only linear interpolation between points dening a curve, circular or ellipsoid shapes should not be used. Utilize rectangles or triangles instead. In ultrasound systems which utilize a circle or ellipse measurement algorithm, its accuracy may be tested by dening 3 points ! to make a circle or 4 points to make an ellipse as shown. The following formulae are useful:
Rectangle Area Perimeter A = ab P = 2(a+b)
Circle A = r2 P = d
Ellipse A = (ab)/4 P = ((a2 + b2)/2)0.5
For example, the target diagram shows a circle with a radius of 2.0 cm. Its computed area is 12.57cm2. Its perimeter is 12.57cm (the identical value for the perimeter and area is a coincidence). These computed values may be compared with those calculated from the ultrasound systems algorithm. Determination of volume or surface area may be accomplished using the line targets or the 3D egg test object (Model 560 only). If using line targets, the volume or surface area corresponds to a cylindrical rod, rectangular bar, or prism outlined by the 2D geometrical shape normal to the notional rod or bar. ! To calculate a surface area or volume, an image is taken at a particular scan plane. Using the calipers, the dimensions of the 2d shape are taken and area determined based on the systems algorithms. Next, perform a 3D scan of the line targets with the scan planes parallel to each other and the scan direction perpendicular to the axes of the line targets. The distance between the rst scan plane and the last multiplied by the 2D area will give the 3D volume. This system calculated value may then be compared to the actual volumes calculated from the rod lengths and the areas coincident with the 2D shape utilized. A volume measurement of the 3D egg test object may be accomplished by measuring the linear dimensions of the two major axes. Position the transducer so that the scan plane coincides with the maximum cross-sectional area along the length of the object. That is dimension a. Re-position the transducer to measure the maximum circular cross-section, dimension b. Multiple measurements should be made and averaged. The volume of an ellipse with circular cross sections is given by: ! ! V = (4/3) (a/2) (b/2)2
The Model 560 3D egg test object has nominal dimensions of 7.0 cm (major axis = a) and 5.0 cm !(minor axis = b). The calculated volume is 91.6 cm3.
1. Place the phantom on a clean, at surface with
scanning surface #1 positioned for use.
2. Apply an adequate amount of low viscosity gel the
scan surface.
3. Adjust the instrument settings (TGC, output, etc.)
to establish baseline values for "normal" liver scanning. If the bottom of the phantom is seen, adjust the gain settings until image goes entirely black. Record these settings on the quality assurance record. These settings should be used for subsequent testing. Position the transducer over the line target target group or 3D egg test object in the phantom, until a clear image is obtained. Freeze image and obtain a hard copy. Measure the appropriate 2D dimensions Perform a 3D scan. Compare computed and system algorithm spatial measurements All ndings should be documented on the quality assurance record.
4. 5. 6. 7. 8. 9.
Results
Spatial measurements are compared with known areas and volumes and compared with the system manufacturers specifications. Computed values, when compared to baseline measurements should not vary over time.
Figure 7
You might also like
- Phantom Testing InstructionDocument14 pagesPhantom Testing InstructionkarankkNo ratings yet
- AIUM Medical Ultrasound SafetyDocument60 pagesAIUM Medical Ultrasound Safetyscuby660No ratings yet
- WS80A v2.00Document209 pagesWS80A v2.00Biomed UltrasoundNo ratings yet
- Ultrasound ResumeDocument1 pageUltrasound ResumejacquikravitzNo ratings yet
- Siemens Somatom Sensation Cardiac A60 Users Manual 410406 PDFDocument128 pagesSiemens Somatom Sensation Cardiac A60 Users Manual 410406 PDFronny sierraNo ratings yet
- Safety of Radiographic Imaging During Pregnancy - American Family PhysicianDocument7 pagesSafety of Radiographic Imaging During Pregnancy - American Family PhysicianDuddy Ari HardiantoNo ratings yet
- Iacta 2011 Janak Mehta Award Winning PresentationDocument56 pagesIacta 2011 Janak Mehta Award Winning PresentationDr.Sandeep Kumar KarNo ratings yet
- Slide Ultrasound Part 1Document27 pagesSlide Ultrasound Part 1Hanif HussinNo ratings yet
- Women's Imaging: MRI with Multimodality CorrelationFrom EverandWomen's Imaging: MRI with Multimodality CorrelationMichele A. BrownRating: 5 out of 5 stars5/5 (1)
- PVM-2701-2703 Lo BR enDocument4 pagesPVM-2701-2703 Lo BR enkizen_567% (3)
- 103manual QAP Radiologi Pindaan Januari 2019Document115 pages103manual QAP Radiologi Pindaan Januari 2019UMGC Sri RampaiNo ratings yet
- Breast Unit SOP: Checklist While Giving ROIS AppointmentDocument7 pagesBreast Unit SOP: Checklist While Giving ROIS AppointmentAbhinav Ingle100% (1)
- Radio BiologyDocument26 pagesRadio BiologyMAN MedanNo ratings yet
- Viner 2005 Forensic Radiography in South AfricaDocument24 pagesViner 2005 Forensic Radiography in South Africah8517No ratings yet
- Quick Reference Guide (Us) s2000Document26 pagesQuick Reference Guide (Us) s2000Nuno Freitas BastosNo ratings yet
- Ultrasound Equipment Quality Assurance - CHAPTER 14Document3 pagesUltrasound Equipment Quality Assurance - CHAPTER 14Pengcab PARI Kota BekasiNo ratings yet
- Somatom Sessions 20-00079278-00270160 PDFDocument66 pagesSomatom Sessions 20-00079278-00270160 PDF2vjNo ratings yet
- Gel Phantom in Ultrasound DosimetryDocument7 pagesGel Phantom in Ultrasound DosimetrytomgrgicNo ratings yet
- Brochure CT Scan SOMATOM Perspective PDFDocument46 pagesBrochure CT Scan SOMATOM Perspective PDFratna_fanoNo ratings yet
- Doppler Ultrasound of The KidneysDocument23 pagesDoppler Ultrasound of The KidneysivoklarinNo ratings yet
- IU22Document60 pagesIU22oligostarkNo ratings yet
- MEDICAL ELECTRONICS PROJECTS ABSTRACT-Digital Pulmonary Function Test - SpirometryDocument4 pagesMEDICAL ELECTRONICS PROJECTS ABSTRACT-Digital Pulmonary Function Test - SpirometryR.ASHOKKUMAARNo ratings yet
- Iodinated Contrast Media GuidelineDocument41 pagesIodinated Contrast Media GuidelineN Aa100% (1)
- A Basic Ultrasound Machine Has The Following Parts: WavesDocument38 pagesA Basic Ultrasound Machine Has The Following Parts: WavesAhmed Sabry100% (1)
- 3D Ultrasound Hype or HelpfulDocument4 pages3D Ultrasound Hype or Helpfulsubramanyam LAKSHMIPURAMNo ratings yet
- Liver Imaging: MRI with CT CorrelationFrom EverandLiver Imaging: MRI with CT CorrelationErsan AltunNo ratings yet
- Tip-Tv: Program Supplement CT: Cardiac ApplicationsDocument47 pagesTip-Tv: Program Supplement CT: Cardiac ApplicationsvitapabloNo ratings yet
- Radiation Dose and Protection in DentistryDocument11 pagesRadiation Dose and Protection in DentistryPhuong ThaoNo ratings yet
- ISUOG - Fetal Nervous System ExaminationDocument8 pagesISUOG - Fetal Nervous System ExaminationAzucenaNo ratings yet
- Endoscopy Department: Graphic Standards Programming and Schematic DesignDocument25 pagesEndoscopy Department: Graphic Standards Programming and Schematic Designmonir61100% (1)
- Contrast Media and Adverse Effects - Vijay KumarDocument41 pagesContrast Media and Adverse Effects - Vijay KumarTapshi SohalNo ratings yet
- MammographyDocument84 pagesMammographyCeles Nilleny UchihaNo ratings yet
- Final MIT Logbook JamilDocument15 pagesFinal MIT Logbook Jamilammar-nasir3314No ratings yet
- MRI Safety TrainingDocument20 pagesMRI Safety TrainingYuda Fhunkshyang100% (1)
- X-Ray Tube Heating and Cooling FactorsDocument22 pagesX-Ray Tube Heating and Cooling FactorsamitNo ratings yet
- Electrocardiogram (ECG or EKG) : Danilyn R. Cenita Paula M. PauloDocument41 pagesElectrocardiogram (ECG or EKG) : Danilyn R. Cenita Paula M. PauloDhanNie CenitaNo ratings yet
- Hernia Repair 3Document38 pagesHernia Repair 3caliptra36No ratings yet
- Siemens Acuson S2000 ABVS 14L5BV Transducer BrochureDocument2 pagesSiemens Acuson S2000 ABVS 14L5BV Transducer BrochureTanya Reynolds50% (2)
- Retrograde Urethrogram - RUGDocument2 pagesRetrograde Urethrogram - RUGJALIL UR REHMANNo ratings yet
- 2017 Truebeam IPADocument166 pages2017 Truebeam IPAzhen yongjieNo ratings yet
- GE 64 Slices CTDocument6 pagesGE 64 Slices CTDhon de CastroNo ratings yet
- ProSim 8 DSDocument12 pagesProSim 8 DSjuliantoroesNo ratings yet
- RF Coils for MRIFrom EverandRF Coils for MRIJ. Thomas VaughanNo ratings yet
- Mindray DP50 Standard SpecDocument3 pagesMindray DP50 Standard SpecRobert HarijantoNo ratings yet
- CT Accreditation Program Clinical Image Quality GuideDocument47 pagesCT Accreditation Program Clinical Image Quality GuideAndreasNo ratings yet
- LINAC by Dr. Musaib MushtaqDocument48 pagesLINAC by Dr. Musaib MushtaqDr. Musaib Mushtaq100% (2)
- Medical Equipment - DefibrillatorDocument25 pagesMedical Equipment - DefibrillatorLem PaneloNo ratings yet
- (Philip T. English DCR, Christine Moore DCR (Auth.Document188 pages(Philip T. English DCR, Christine Moore DCR (Auth.Åri Budianto100% (1)
- Cranial Ultrasound: A Guide to Sonographic Technique and PathologiesDocument43 pagesCranial Ultrasound: A Guide to Sonographic Technique and PathologiesJazib ShahidNo ratings yet
- Evaluation and Routine Testing in Medical Imaging DepartmentsDocument18 pagesEvaluation and Routine Testing in Medical Imaging DepartmentsRankie Choi100% (1)
- OpenMrs Radiology Module User GuideDocument33 pagesOpenMrs Radiology Module User GuideSkaksNo ratings yet
- Audiometers OK PDFDocument81 pagesAudiometers OK PDFErnesto AcostaNo ratings yet
- Chapter 3 - Introduction To Nuclear MedicineDocument4 pagesChapter 3 - Introduction To Nuclear MedicineunknownxemNo ratings yet
- Barium MealDocument3 pagesBarium MealVithiya Chandra SagaranNo ratings yet
- Hospital Practice & Patient CareDocument14 pagesHospital Practice & Patient CareAkinsola AyomidotunNo ratings yet
- Basics of Chest X-Ray Interpretation (39Document23 pagesBasics of Chest X-Ray Interpretation (39Rabi Dhakal100% (1)
- IOSbasic 9 e 1Document20 pagesIOSbasic 9 e 1La Bruja del EsteNo ratings yet
- Policies and Procedures Radiology DepartmentDocument6 pagesPolicies and Procedures Radiology DepartmentRalph Gerard Saldajeno ValdespinaNo ratings yet
- Conventional TomographyDocument8 pagesConventional TomographyMohamad Hilman Al-Kelantani67% (3)
- Modulo TiristorDocument5 pagesModulo TiristorMitecCenememNo ratings yet
- Can Analyzer Mn67216 EngDocument24 pagesCan Analyzer Mn67216 EngFerdinand VelokurckiNo ratings yet
- Can 20Document72 pagesCan 20hemanthbbcNo ratings yet
- As3000 Service Manual PDFDocument180 pagesAs3000 Service Manual PDFsambadeeNo ratings yet
- Servicemanual Welch Allyn300Document106 pagesServicemanual Welch Allyn300MitecCenememNo ratings yet
- Class X Mathematics: Page No. Dropped Topics/ChapterDocument6 pagesClass X Mathematics: Page No. Dropped Topics/ChapterПараг ТамбеNo ratings yet
- NIMCET 2020 Question PaperDocument10 pagesNIMCET 2020 Question PaperAnirban Adhikari AniiNo ratings yet
- Model Paper Sainik School Class 6Document2 pagesModel Paper Sainik School Class 6AbcNo ratings yet
- MATH 4 Q4 WEEK 1 DLLDocument6 pagesMATH 4 Q4 WEEK 1 DLLJulie LescanoNo ratings yet
- Contemporary Math FundamentalsDocument31 pagesContemporary Math FundamentalsAngelene Mae MolinaNo ratings yet
- MAA EXTRA SPECIMEN QUESTIONS SOLVEDDocument15 pagesMAA EXTRA SPECIMEN QUESTIONS SOLVEDnkvfdvdfNo ratings yet
- STD 10 Math QPandMSKV Hyd 5Document22 pagesSTD 10 Math QPandMSKV Hyd 5RAJESH P KNo ratings yet
- SRCE 2.0 User Manual R2Document117 pagesSRCE 2.0 User Manual R2Shalaho D DevyNo ratings yet
- Big Bay Bei Qualifier Round 2021 (P4)Document13 pagesBig Bay Bei Qualifier Round 2021 (P4)S1ice man100% (2)
- Math CHP Worksheet PDFDocument20 pagesMath CHP Worksheet PDFzainabNo ratings yet
- Volume and Surface Area of 3D ShapesDocument6 pagesVolume and Surface Area of 3D Shapesfatima malhiNo ratings yet
- Lecture Planner - Maths - PDF Only - (Udaan 2024)Document2 pagesLecture Planner - Maths - PDF Only - (Udaan 2024)P SrinivasNo ratings yet
- Soil Mechanics and Construction TechnologyDocument18 pagesSoil Mechanics and Construction TechnologyGebshet WoldetsadikNo ratings yet
- Antiderivative and Indefinite IntegralDocument5 pagesAntiderivative and Indefinite IntegralDimas HernadyNo ratings yet
- Midterm 1Document11 pagesMidterm 1JUNIOR RAID YEBARA GUTIERREZNo ratings yet
- June 2017 QPDocument24 pagesJune 2017 QPGordon CheungNo ratings yet
- Kto12 Curriculum GuideDocument59 pagesKto12 Curriculum GuideDiane RodriguezNo ratings yet
- Drop Forging Die DesignDocument6 pagesDrop Forging Die DesignChinmay Das88% (8)
- Module in Mathematics 8: Your Lesson For TodayDocument20 pagesModule in Mathematics 8: Your Lesson For TodayDhenver DimaculanganNo ratings yet
- LITTLE FLOWER SYLLABUS 2022-23Document7 pagesLITTLE FLOWER SYLLABUS 2022-23Big boiiigNo ratings yet
- Physics Lab Measures UncertaintyDocument20 pagesPhysics Lab Measures UncertaintyakhitoNo ratings yet
- Math g6 m5 Teacher Materials PDFDocument329 pagesMath g6 m5 Teacher Materials PDFMariaNo ratings yet
- 2003 AIME solutions title under 40 charactersDocument10 pages2003 AIME solutions title under 40 charactersARNAV AMBRENo ratings yet
- DualDocument35 pagesDualdangreglongNo ratings yet
- SP Maths Basic 10Document7 pagesSP Maths Basic 10G AshithNo ratings yet
- Grade 4 - 4Q MATH Answer KeyDocument9 pagesGrade 4 - 4Q MATH Answer Keyflower.power11233986100% (2)
- Polynomial Word Problems WorksheetDocument2 pagesPolynomial Word Problems WorksheetChelsea Henderson100% (1)
- 3D Mensuration Last 5 Year Best Questions by Gagan Pratap SirDocument14 pages3D Mensuration Last 5 Year Best Questions by Gagan Pratap SirAnupam Gautam0% (1)
- Teacher's Resource Book 4 PDFDocument268 pagesTeacher's Resource Book 4 PDFPaulo Mkali88% (8)
- GCSE-Mathematics - 504-November2021-Foundation Tier, M6 Paper 2 (With Calculator) - PaperDocument20 pagesGCSE-Mathematics - 504-November2021-Foundation Tier, M6 Paper 2 (With Calculator) - PaperRanil SilvaNo ratings yet