Professional Documents
Culture Documents
Percutaneous Aponeurotomy and Lipofilling A.43
Uploaded by
Yuriko AndreOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Percutaneous Aponeurotomy and Lipofilling A.43
Uploaded by
Yuriko AndreCopyright:
Available Formats
RECONSTRUCTIVE
Percutaneous Aponeurotomy and Lipolling: A Regenerative Alternative to Flap Reconstruction?
Roger K. Khouri, M.D. Jan Maerten Smit, M.D. Eufemiano Cardoso, M.D. Norbert Pallua, M.D., Ph.D. Laurent Lantieri, M.D. Irene M. J. Mathijssen, M.D., Ph.D. Roger K. Khouri, Jr., B.S. Gino Rigotti, M.D.
Boston, Mass.
Background: The application of a new approach is presented, percutaneous aponeurotomy and lipolling, which is a minimally invasive, incisionless alternative to traditional ap reconstructions. Methods: The restrictive subdermal cicatrix and/or endogenous aponeurosis is punctured, producing staggered nicks. Expansion of the restriction reconstructs the defect and creates a vascularized scaffold with micro-openings that are seeded with lipografts. Wide subcutaneous cuts that lead to macrocavities and subsequent graft failure are avoided. Postoperatively, a splint to hold open the neomatrix/graft construct in its expansive state is applied until the grafts mature. Thirty-one patients underwent one to three operations (average, two) for defects that normally require ap tissue transfer: wounds where primary closure was not possible (n = 9), contour defects of the trunk and breast requiring large-volume fat grafts (n = 8), burn contractures (n = 5), radiation scars (n = 6), and congenital constriction bands (n = 3). Results: The regenerated tissue was similar in texture and consistency to the surrounding tissues. Wider meshed areas had greater tissue gain (range, 20 to 30 percent). There were no signicant wound-healing issues, scars, or donorsite morbidities. Advancement tension was relieved without ap undermining or decreased perfusion. Conclusions: Realizing that, whether scar or endogenous fascia, the subdermal aponeurosis limits tissue stretch and/or its three-dimensional expansion, a minimally invasive procedure that expands this cicatrix into a matrix ideally suited for fat micrografts was developed. Grafting this scaffold applies tissueengineering principles to generate the needed tissue and represents a regenerative alternative to reconstructive ap surgery. (Plast. Reconstr. Surg. 132: 1280, 2013.) CLINICAL QUESTION/LEVEL OF EVIDENCE: Therapeutic, V.
n this report, a new concept that harnesses the regenerative potential of fat grafting1 as an alternative to ap transfer is explored. There has been a resurgence of interest in fat grafting for volume replacement.210 However, fat grafting is commonly deemed unreliable because of variable resorption; this may be caused by fat deposition in large pools or spaces in the tissue where it is unable to survive acutely by diffusion until neovascularization provides support.1,2 To overcome this limitation, surgeons have focused mainly on different aspects of the graft itself: harvesting,
From Brigham and Womens Hospital. Received for publication April 2, 2013; accepted April 30, 2013. Copyright 2013 by the American Society of Plastic Surgeons DOI: 10.1097/PRS.0b013e3182a4c3a9
processing, and enrichment.1113 However, successful grafting is also dependent on maximization of the recipient sites capacity to accept and support the graft. Our experience with fat grafting percutaneously released Dupuytren contractures has shown that a tight cord can be transformed into a fat graft recipient scaffold.14 The most severe contractures can also be released without aps. The procedure requires nicking of the cord and the palmar aponeurosis, which can expand in a fashion similar to meshed skin grafts. With the deeper restriction released, the Disclosure: Roger K. Khouri (Sr.), M.D., has an equity interest in the company, Brava, LLC, the manufacturer of the Brava device. None of the other authors has any nancial information to disclose.
1280
www.PRSJournal.com
Volume 132, Number 5 Percutaneous Aponeurotomy and Lipofilling
overlying palmar skin can freely stretch to obviate the need for aps. This led to the realization that other contractures and tissue deciencies might be treated without resorting to aps if the deeper tissues that restrict advancement are mesh-expanded and the tiny gaps generated are fat-grafted. In a two-dimensional defect, the limitation to tissue advancement and primary closure is the underlying scar or the subcutaneous fascia, collectively called the subcutaneous aponeurosis. Mesh expansion of the restrictive bers within the aponeurosis, using percutaneous, staggered nicks in the plane of aponeurosis, increases the surface area, allowing further tissue advancement. This percutaneous aponeurotomy creates small pockets or gaps, interspersed with thin connective bands of the original scar/fascia. The gaps in the resulting matrix are ideally suited for grafting fat. Percutaneous mesh expansion should be contrasted with fasciotomies and relaxing incisions, which generate large gaps where the grafts may collect in large deposits and die (Fig.1).14,15 To correct volume decits, the restriction is three-dimensional, and increases in surface area are not sufcient to effect an optimal space-lling expansion. For proper three-dimensional release, the nicks must be staggered in multiple planes in multiple directions, wherever restrictive bers prevent expansion. This technique is named Rigottomy after its originator.16,17 Its application leads to an expansion of the restrictive block of scar tissue to create a larger three-dimensional recipient scaffold for fat grafting. The loosened grafted scar becomes softer and closer to normal tissue. Repeating the process a few months later leads to substantial tissue volume gain and scar reduction. The Rigottomy is useful when grafting fat into scarred tissue to correct a volume deciency. It transforms a restrictive cicatrix into a regenerative matrix. Our clinical experience with grafting the scarred breast and the Dupuytren hand led us to rene this procedure, the percutaneous aponeurotomy and lipolling reconstruction, which offers a potentially scarless alternative to aps. the g-force is much less than that described by Coleman,3,4 typically approximately 15 to 20 g. The dilute lipoaspirate slurry is injected meticulously into the recipient scaffold, using a ne cannula and a small syringe. The most even distribution of graft is achieved by injecting through multiple needle holes all around the defect, and through each entry site, performing multiple radial passes in multiple planes, never injecting more than a few microliters at a time. The injection continues until the recipient tissue become tight and blanches from the epinephrine still present in the graft solution. This technique is termed lipotumescence. At this stage, the interstitial uid pressure is above physiologic range because the added volume from the graft swells the site beyond what the compliance of the scarred tissue would allow.18 Increased interstitial uid pressure aids the next step by putting the restrictive tissue bers under tension, making them susceptible to nicking by a sharp needle tip. An 18-gauge hypodermic needle is used for the Rigottomies,16,17 or for more practical and effective release, a brush-like device is used to inict a predetermined pattern of staggered nicks that transforms the scar/fascia into the neomatrix scaffold. Tension is the key to the differential cutting ability of the needle tips. For the nicks to be more directional, a skin hook is often used to exert additional tension in the third dimension of expansion (Fig.2). The needles are inserted multiple times in an ordered and staggered series of punctures, typically at a density of four or ve nicks per square centimeter. At each puncture, a 45- to 60-degree oscillatory motion of the needlepoint generates short slits in the fascia, which results in loosening and expansion. Each time a nick is made, it is readily felt by the surgeon retracting as a tiny release advancement, and can often be heard as a soft click, provided that there is sufcient tension on the scar/fascia. These nicks open the tissue, creating a honeycomb pattern into which the graft moves, expanding the space and reducing interstitial uid pressure to physiologic levels. To maximize expansion and volume of graft placement within a given scar/fascia bed, occasionally the best option is to alternate between graft injection and aponeurotomy/nick creation. The deep tissue release is performed through many 2-mm puncture wounds that regenerate individually, rarely resulting in new scar formation. Open scoring of the restrictive fascia or incisions that cause a broader relaxation must be avoided. These create cavities where fat may
PERCUTANEOUS APONEUROTOMY AND LIPOFILLING PRINCIPLE AND TECHNIQUE
The procedure begins with tumescent syringe liposuction, using a 2.7-mm, 12-hole cannula (Marina Medical, Sunrise, Fla.), from wherever the patient has excess fat. The aspirated fat is allowed to sediment for a few minutes, or if centrifuged,
1281
Plastic and Reconstructive Surgery November 2013
Fig. 2. Placement of an 18-gauge needle mounted onto a needle holder is shown (right), with an oscillatory movement to make the many small nicks/cuts (Rigottomies) in the scar/ fascia. The two Gillies hooks place the scar/fascia under tension to allow the needle tip to preferentially release the fibers that restrict expansion.
Fig. 1. Flap versus percutaneous aponeurotomy and lipofilling versus relaxing incisions. Z-plasty flap transposition (above) is compared with the percutaneous aponeurotomy and lipofilling procedure (center) and with the fasciotomy/relaxing incisions (below) simulated on a surgical glove, with incisions outlined with a blue marker. In the classic Z-plasty flap transposition, a 5-cm vertical tightness (above, left) is expanded to 7cm at the expense of a horizontal tightness (above, right). Borrowing from Peter to pay Paul resulted in no overall tissue gain. In contrast, scars were left behind and flap necrosis and wound healing issues were risked. The percutaneous aponeurotomy and lipofilling procedure (center, left) uses a series of small percutaneous nicks to mesh the deeper tissues that restrict advancement. Mesh expansion (center, right) of the restrictive subcutaneous tissue enlarges the flap from 8 to 11 cm while leaving behind a network of small gaps where the fat grafts can survive. A net 3-cm tissue gain (30 percent) was generated without new scars.
collect and die from insufcient proximity to a recipient capillary network. For this reason, only small gaps are created. For two-dimensional defects, the process is akin to skin graft mesh expansion. For three-dimensional defects, a solid block of scar tissue is mesh-expanded in the third dimension, creating a honeycomb structure with micro-openings into which grafts can migrate and survive. The most important component of a successful percutaneous aponeurotomy and lipolling is the transformation of a restrictive cicatrix into a regenerative matrix that expands a tight scar or constriction into a loose, threedimensional recipient scaffold that is receptive to fat grafts. Performed solely through needle pricks, the procedure is usually scarless. The key to success is knowing when to stop the release and the grafting. Too many cuts or Rigottomies in the tissue leads to structural loss of the brous network, the merging of adjacent small nicks/cuts into larger slits, and the formation of cavities where fat grafts may pool and fail. Whenever possible, preprocedural Brava (Brava, LLC, Miami, Fla.) expansion is included, which loosens restrictive bers and increases capillary density,19
Fig. 1. (Continued) In the fasciotomies or relaxing incisions (below, left), instead of meshing the tissue with multiple tiny nicks, two large cuts are made. Advancement of the tissue is not as even and the cuts expand into large open spaces (below, right), where the fat grafts will pool with poor interface with the recipient, leading to fat necrosis, fibrosis, and likely loss of the expansion from scar contraction.
1282
Volume 132, Number 5 Percutaneous Aponeurotomy and Lipofilling
allowing more Rigottomies to be performed without signicant vascular compromise.2026 A gain of approximately 20 percent of the total meshed area can be accomplished at each stage. This two-dimensional increase translates to a larger three-dimensional volume expansion. An interval of at least 2 to 3 months is used between sessions to allow inammation to subside and the grafts to mature. After each release and grafting procedure, the construct is splinted in outward extension. Although standard splints function well for two-dimensional defects, for three-dimensional volume correction, our current preferred splinting method is the Brava external negative-pressure device,27 which is capable of exerting a gentle three-dimensional outward expansive force in the early postoperative period. The increased vascularity from Brava enhances graft survival.19,23,24 Keeping the meshed brous construct in an open-expanded shape is akin to having many tiny growth chambers where spontaneous adipogenesis may occur.28,29 Clinical Experience Thirty-one patients were treated for various body area defects: trunk (n = 3), breasts (n=12), extremities (n = 13), face (n = 2), and scalp (n=1). Percutaneous aponeurotomy and
Fig. 3. Palmar scar contracture before (above) and 1 year after (below) a single percutaneous aponeurotomy and lipofilling release. Note the severe blanching before the percutaneous aponeurotomy and lipofilling in the thumb/fifth finger line with the patients effort to open the hand, which was eliminated, with excellent mobility after the procedure.
1283
Plastic and Reconstructive Surgery November 2013
Fig. 4. Preoperative and postoperative abduction. A single-stage percutaneous aponeurotomy and lipofilling procedure was performed on a trunk burn patient (left), after which a 45-degree abduction gain was achieved (right). The restrictive subcutaneous scar was meshed from the abdomen to the antecubital fossa.
Fig. 5. (Left) Preprocedural view of postirradiation axillary contracture and threatened implant erosion; (center) periprocedural view showing mesh release of the contracture and immediate filling of the grafted fat into the expanded scaffold, including fat grafting in the thin space between the skin and the implant capsule; and (right) 1-month postprocedural view with nearly full arm elevation and improved breast contour and implant padding.
1284
Volume 132, Number 5 Percutaneous Aponeurotomy and Lipofilling
no signicant complications or wound healing issues. The tension of the scarred site was always relieved without ap undermining or noticeably decreased perfusion. The regenerated tissue had nearly normal texture and often with considerable preservation of sensation.
CASE REPORTS
The versatility of the technique is illustrated in several clinical cases shown below. Case 1: Palmar Scar
A 21-year-old man sustained a short-range gunshot blast injury to the palm of the hand that was dbrided and allowed to heal by secondary intention. He presented with a stellate contracted midpalmar scar and tendon adhesions that restricted digital extension. He had already failed treatment with splinting alone. The deciency was treated with a percutaneous aponeurotomy and lipolling similar to a Dupuytren contracture release.30 With the contracture under tension, the restrictive scar was mesh-expanded through multiple punctures and the resultant loosened structure was grafted with 30ml of dilute lipoaspirate, diffusely injected into the palm. The hand was splinted in extension for 1 week and then with night splints for 3 months (Fig.3).
Fig. 6. Computed tomographic scan of the patient in case 4, showing severe scoliosis with a fixed contour defect on the right. A thin subcutaneous layer of tissue is evident in the defect, adherent to fascia, which is the target site for treatment.
lipolling was used as an alternative to a ap for the following indications: wound defects that could not be closed primarily (n = 9), contour defects that required megavolume fat grafts (n = 8), burn contractures (n = 5), radiation scars (n = 6), and congenital constriction bands (n = 3). All patients had their defects regenerated with tissues similar in texture and consistency to the surrounding tissues without additional scars or donor-site morbidity. Because the maximal permitted tissue gain is 20 to 30 percent per percutaneous aponeurotomy and lipolling session, most cases required two procedures (range, one to three) performed 2 months apart. There were
Case 2: Burn Scar Contracture
A 42-year-old man with second- and third-degree burns to the trunk, axilla, and left upper extremity presented 1 year after skin grafting and wound healing with a severe axillary contracture. He failed scar management therapy and extension splints. After tumescent lipolling of the burn scar with 150ml of dilute lipoaspirate, and with the contracture under tension, a percutaneous aponeurotomy of the restrictive scar was performed through hundreds of skin nicks over a wide area. To preserve the integrity of the scar and its ability to support fat grafts, the concentration of nicks in the axilla was limited. Tissue length needed for arm elevation was gained by performing the percutaneous aponeurotomy and lipolling over a wide surface area, extending from
Fig. 7. Modification of Brava for three-dimensional splinting in the patient in case 4.
1285
Plastic and Reconstructive Surgery November 2013
Fig. 8. Views of the left flank obtained preoperatively (left) and 5 months postoperatively (right). To improve her contour, more than 300ml of fat survived, and her trunk circumference at the depth of the cleft increased from 65cm to 78cm.
the antecubital fossa to the abdomen. The patient had a shoulder extension splint applied (which he poorly tolerated) and underwent physiotherapy for 2 months after percutaneous aponeurotomy and lipolling. Three months after the rst-stage percutaneous aponeurotomy and lipolling, a 45-degree abduction gain was achieved and the scar was signicantly softened (Fig.4). volume deciency, and scar adhesion bands tethering the skin deep in the cleft (Fig.6). After harvesting fat from the hip, buttock, and abdominal area, and subsequent low-gravity centrifugation, the defect was tightly lipotumesced with 250ml of lipoaspirate through multiple needle puncture entry sites. The graft was delivered in a sprinklerlike fashion from each site through numerous passes of the cannula at multiple angles and multiple levels, delivering less than 2ml per pass. The Rigottomy, consisting of percutaneous needle releases of the constricted area, relieved the lipotumescent tension and opened the defect. Achieving the necessary gain in cutaneous circumference at the level of the cleft required meshing the subcutaneous tissues past the midline both anteriorly and posteriorly. The cycle of lipotumescent grafting and meshing was repeated until 375ml of fat was diffusely grafted in the matrix. Because the correction required the application of a three-dimensional splint postoperatively, the silicone gel rim of Brava was used in combination with a custom-made hard-top and a transparent polyurethane membrane (OpSite; Smith & Nephew, London, United Kingdom) to preserve a low-vacuum seal (Fig.7). Supercial blisters under the gel rim led to short interruptions of the 2-month postgrafting vacuum splint treatment. With conservative treatment, all wounds healed without scars. There were no clinical signs of infection, fat necrosis, or fat resorption, and the resulting ank correction remained stable throughout the rst 5 postoperative months (Fig.8).
Case 3: Irradiated Axillary Scar Contracture
A 65-year-old woman 23 years following mastectomy and irradiation to the axilla presented with progressive inability to raise her left arm and an indurated contracture of the pectoralis and latissimus muscles (along with threatened erosion of the breast implant). There was no available local ap that could be used to perform a classic release of the contracture. The underlying scar-irradiated tissues were tumesced with 100ml of dilute lipoaspirate. Then, with the contracture under tension from lipotumescence and arm elevation, hundreds of Rigottomy nicks/cuts were made into the pectoralis and the latissimus dorsi muscle. This subcutaneous tissue release was performed in multiple staggered planes and on multiple levels, which allowed nearly full arm elevation to be achieved during the procedure (Fig.5). This gain in motion was maintained postprocedurally, and as the fat grafts matured, the tissue gradually improved in consistency and texture. To pad the breast implant, the plane between the capsule and skin was also fat grafted during the same setting.
Case 4: Flank Defect
An 18-year-old female patient presented with a large, xed, three-dimensional contour defect of the left ank 5 years after a thoracolumbotomy and a dorsal thoracolumbar spondylodesis for an extreme progressive congenital idiopathic scoliosis. Percutaneous aponeurotomy and lipolling simultaneously addressed three problems: a cutaneous surface topography deciency of the trunk circumference at the depth of the cleft, a soft-tissue
Case 5: Breast Agenesis
A 15-year-old girl with left breast agenesis from tumor resection during infancy presented with a rudimentary nipple-areola complex tethered to the chest, minimal breast volume restricted to the upper outer quadrant, and a contour defect of the chest wall. The Brava device was applied for 4 weeks before grafting. Her abnormal chest contour precluded her from achieving a normal vacuum seal and regular Brava use. She had to apply the Brava domes while lying down. With a hand pump, she brought the vacuum pressure to 80
1286
Volume 132, Number 5 Percutaneous Aponeurotomy and Lipofilling
Fig. 9. Progression of Brava expansion and serial percutaneous aponeurotomy and lipofilling sessions that generated the lower pole of the right breast. (Above, left) Original defect. (Above, second from left) Prepercutaneous aponeurotomy and lipofilling Brava expansion increased breast volume and separated the nipple-areola complex from the chest. (Above, center) Completion of the first percutaneous aponeurotomy and lipofilling; note the tissue gain and the multiple needle holes necessary for the percutaneous aponeurotomy. (Above, second from right) Extent of additional Brava expansion 8 weeks after the first percutaneous aponeurotomy and lipofilling, at the time of the second percutaneous aponeurotomy and lipofilling. (Above, right) Normal application of Brava. (Below, left) Early outcome after second percutaneous aponeurotomy and lipofilling. (Below, second from left) Further volume and nipple-to-intramammary length gained after 8 additional weeks of Brava expansion at the time of the third percutaneous aponeurotomy and lipofilling. (Below, center) Immediately after the third percutaneous aponeurotomy and lipofilling. Note again the multiple needle punctures required to three-dimensionally expand the restriction into a receptive scaffold for fat grafts. (Below, second from right) Early result. (Below, right) Final outcome at 18 months showing regeneration of the lower pole of the breast and sustained volume and shape.
mmHg for 30 minutes, followed by 30 to 60 seconds of deation, repeating the cycle four or ve times in a row, twice daily. This loosened the tissues, induced a hyperemia indicative of increased vascularity, and separated the nipple-areola complex from the chest wall by 2 to 3cm (Fig.9, above, left and second from left). The rst percutaneous aponeurotomy and lipolling procedure increased the separation of the nipple-areola complex from the inframammary fold by 1 to 2cm, generated tissue in the lower pole, and partially corrected the volume and contour defect (Fig.9, above, center). Thirtysix hours after the procedure, she resumed Brava wear to maintain the release and support graft survival. Over the next 8 weeks, Brava expansion augmented tissue matrix, breast volume, and cutaneous envelope (Fig.9, above, second from right). The improved chest wall contour allowed her to transition to normal Brava wear at 20-mmHg vacuum (Fig.9, above, right). During the second percutaneous aponeurotomy and lipolling, additional volume and lower pole tissue were gained (Fig.9, below, left and second from left), after which she resumed Brava wear for 8 weeks in preparation for a third and nal grafting session (Fig.9, below, center and second from right). At 18-month followup, she has a breast that is soft and sensate and appears like the normal contralateral breast (Fig.10). This regenerated a breast mound without any scar, incision, ap transfer, or insertion of alloplastic implants.
DISCUSSION
Percutaneous aponeurotomy and lipolling is a new concept that adheres to basic plastic surgery principles: release of the contracture, meticulous grafting of the created defect, and splinting of the graft in extension.3133 However, instead of treating the large wound defect by classic incisionrelease, contracture release is achieved through a series of percutaneous nicks and staggered slits that mesh expand the scar/fascia and transform it
1287
Plastic and Reconstructive Surgery November 2013
Fig. 10. Oblique (above) and anteroposterior (below) views of the original defect (left) and views at 18-month follow-up (right) of the patient in case 5 after three percutaneous aponeurotomy and lipofilling sessions and Brava expansion over a 20-week treatment span. The procedures corrected the chest wall deformity and generated a symmetrical C-cup breast with symmetry of the nipple-areola complex without using an implant, flap, or incision.
into a recipient scaffold with small holes or gaps that are receptive to lling with grafted fat. For the two-dimensional defects, to maintain the gain in surface area, a simple extension splint can be used. However, to maintain the volume gain for the three-dimensional defects, more elaborate splinting is required. Whenever applicable, a negative-pressure device, such as Brava, can achieve this efciently. In addition, preoperative external expansion of three-dimensional defects with Brava increases not only the size of the recipient site but also capillary density,19 thus preserving
perfusion of the meshed construct, allowing for more extensive meshing. When a meshed skin graft is applied, the advancing epithelial ridge that lls the gaps is considered regeneration. The converse is true for the percutaneous aponeurotomy and lipolling, where it is the defect and its surroundings that are meshed instead, and it is the micrografted fat that lls up the gaps to regenerate like tissue. Gillies and Millard, over 50 years ago, recognized that plastic surgery was the art of replacing like with like and borrowing from Peter to
1288
Volume 132, Number 5 Percutaneous Aponeurotomy and Lipofilling
pay Paul (only if Peter can afford it).34 Whereas conventional reconstruction requires the surgical transfer of tissue aps, percutaneous aponeurotomy and lipolling facilitates tissue regeneration in situ, inducing the growth of the like tissue needed to correct the defect, by turning a restrictive cicatrix into a regenerative matrix. This is achieved by loosening the scar/fascia that restricts advancement with multiple nicks/cuts, turning it into a mesh pattern that expands into a honeycomb-like matrix suited for fat graft survival. Thus, the need to borrow from Peter can be bypassed and, instead, Paul can be given the ability to regenerate and correct the defect. The procedure rarely creates skin scars and leaves no donor-site defect. These cases are a selection of many patients that were treated with percutaneous aponeurotomy and lipolling when the conventional alternative required a ap reconstruction. They show that a broad range of reconstructive problems can be addressed adequately with percutaneous aponeurotomy and lipolling, often performed under regional anesthesia on an outpatient basis. Although this approach of mesh expansion with postoperative splinting (including negative-pressure therapy) allows for larger volumes of lipolling, the expansion tissue gained is limited to 20 to 30 percent of the meshed area. One has to be cautious to not overmesh lest the nicks and cuts merge to create large cavities where the injected fat graft will die. Similarly, the amount of lipolling should be moderated, to prevent overinjection and resulting excess interstitial pressure. Optimal correction of extensive defects often requires more than one percutaneous aponeurotomy and lipolling session.
REFERENCES
1. Eto H, Kato H, Suga H, et al. The fate of adipocytes after nonvascularized fat grafting: Evidence of early death and replacement of adipocytes. Plast Reconstr Surg. 2012;129:10811092. 2. Nguyen A, Pasyk KA, Bouvier TN, Hassett CA, Argenta LC. Comparative study of survival of autologous adipose tissue taken and transplanted by different techniques. Plast Reconstr Surg. 1990;85:378386; discussion 387. 3. Coleman SR. Structural fat grafting. Aesthet Surg J. 1998;18:386, 388. 4. Coleman SR. Facial recontouring with lipostructure. Clin Plast Surg. 1997;24:347367. 5. Karacaoglu E, Kizilkaya E, Cermik H, Zienowicz R. The role of recipient sites in fat-graft survival: Experimental study. Ann Plast Surg. 2005;55:6368; discussion 68. 6. Kannan RY, Salacinski HJ, Sales K, Butler P, Seifalian AM. The roles of tissue engineering and vascularisation in the development of micro-vascular networks: A review. Biomaterials 2005;26:18571875. 7. Domergue S, Psomas C, Yachouh J, et al. Fat microinltration autografting for facial restructuring in HIV patients. J Craniomaxillofac Surg. 2006;34:484488. 8. Samdal F, Skolleborg KC, Berthelsen B. The effect of preoperative needle abrasion of the recipient site on survival of autologous free fat grafts in rats. Scand J Plast Reconstr Surg Hand Surg. 1992;26:3336. 9. Khouri RK, Schlenz I, Murphy BJ, Baker TJ. Nonsurgical breast enlargement using an external soft-tissue expansion system. Plast Reconstr Surg. 2000;105:25002512; discussion 2513. 10. De Filippo RE, Atala A. Stretch and growth: The molecular and physiologic inuences of tissue expansion. Plast Reconstr Surg. 2002;109:24502462. 11. Kaufman MR, Bradley JP, Dickinson B, et al. Autologous fat transfer national consensus survey: Trends in techniques for harvest, preparation, and application, and perception of short- and long-term results. Plast Reconstr Surg. 2007;119:323331. 12. Smith P, Adams WP Jr, Lipschitz AH, et al. Autologous human fat grafting: Effect of harvesting and preparation techniques on adipocyte graft survival. Plast Reconstr Surg. 2006;117:18361844. 13. Shiffman MA, Mirrafati S. Fat transfer techniques: The effect of harvest and transfer methods on adipocyte viability and review of the literature. Dermatol Surg. 2001;27:819826. 14. Rubin JP, Bennett JM, Doctor JS, Tebbets BM, Marra KG. Collagenous microbeads as a scaffold for tissue engineering with adipose-derived stem cells. Plast Reconstr Surg. 2007;120:414424. 15. Piasecki JH, Moreno K, Gutowski KA. Beyond the cells: Scaffold matrix character affects the in vivo performance of puried adipocyte fat grafts. Aesthet Surg J. 2008;28:306312. 16. Rigotti G, Marchi A, Gali M, et al. Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: A healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg. 2007;119:14091422; discussion 1423. 17. Rigotti G, Marchi A, Khouri RK. Minimally invasive autolo gous mastectomy incisionless reconstruction; external expansion fat grafting and percutaneous scar release: A multicenter experience. Paper presented at: 88th Annual Meeting and Symposium of the American Association of Plastic Surgeons; March 24, 2009; Rancho Mirage, Calif. 18. Guyton AC, Granger HJ, Taylor AE. Interstitial uid pres sure. Physiol Rev. 1971;51:527563. 19. Heit YI, Lancerotto L, Mesteri I, et al. External volume expansion increases subcutaneous thickness, cell proliferation,
CONCLUSIONS
In summary, percutaneous aponeurotomy and lipolling is a novel procedure in which, with little chance of leaving a visible scar, an array of tiny percutaneous needle sticks create a mesh pattern in deeper tissues under tension and expand them to transform the restrictive cicatrix into a regenerative matrix scaffold suitable for fat grafting. Whether or not it is combined with preoperative and postoperative external expansion, the percutaneous aponeurotomy and lipolling procedure is an effective, simple, permanent, natural, autologous, usually nonscarring, and patient-friendly regenerative alternative to ap reconstructions.
Roger K. Khouri, Jr., B.S. 478 Bay Lane Key Biscayne, Fla. 33149 rogerkhour@aol.com
1289
Plastic and Reconstructive Surgery November 2013
and vascular remodeling in a murine model. Plast Reconstr Surg. 2012;130:18. 20. Del Vecchio DA, Bucky LP. Breast augmentation using preexpansion and autologous fat transplantation: A clinical radiographic study. Plast Reconstr Surg. 2011; 127:24412450. 21. Khouri R, Del Vecchio D. Breast reconstruction and aug mentation using pre-expansion and autologous fat transplantation. Clin Plast Surg. 2009;36:269280, viii. 22. Schlenz I, Kaider A. The Brava external tissue expander: Is breast enlargement without surgery a reality? Plast Reconstr Surg. 2007;120:16801689; discussion 1690. 23. Khouri RK, Eisenmann-Klein M, Cardoso E, et al. Brava and autologous fat transfer is a safe and effective breast augmentation alternative: Results of a 6-year, 81-patient, prospective multicenter study. Plast Reconstr Surg. 2012;129:11731187. 24. Lantieri LA, Martin-Garcia N, Wechsler J, Mitrofanoff M, Raulo Y, Baruch JP. Vascular endothelial growth factor expression in expanded tissue: A possible mechanism of angiogenesis in tissue expansion. Plast Reconstr Surg. 1998;101:392398. 25. Yazawa M, Mori T, Tuchiya K, Nakayama Y, Ogata H, Nakajima T. Inuence of vascularized transplant bed on fat grafting. Wound Repair Regen. 2006;14:586592. 26. Del Vecchio D. Breast reconstruction for breast asymmetry using recipient site pre-expansion and autologous fat grafting. Ann Plast Surg. 2009;62:523527. 27. Brava, LLC. Brava breast enhancement and shaping system. Available at: http://www.mybrava.com. Accessed October 9, 2013. 28. Findlay MW, Dolderer JH, Trost N, et al. Tissue-engineered breast reconstruction: Bridging the gap toward largevolume tissue engineering in humans. Plast Reconstr Surg. 2011;128:12061215. 29. Doldere JH, Thompson EW, Slavin J, et al. Long-term stability of adipose tissue generated from a vascularized pedicled fat ap inside a chamber. Plast Reconstr Surg. 2011;127:22832292. 30. Hovius SE, Kan HJ, Smit X, Selles RW, Cardoso E, Khouri RK. Extensive percutaneous aponeurotomy and lipografting: A new treatment for Dupuytren disease. Plast Reconstr Surg. 2011;128:221228. 31. Costagliola M. General principles of burn reconstruction (in French). Ann Chir Plast Esthet. 2011;56:354357. 32. Schwarz RJ. Management of postburn contractures of the upper extremity. J Burn Care Res. 2007;28:212219. 33. Hudson DA, Renshaw A. An algorithm for the release of burn contractures of the extremities. Burns 2006;32:663668. 34. Gillies H, Millard DR. The Principles and Art of Plastic Surgery. Boston: Little, Brown; 1957.
FILLER-006
e-TOCs and e-Alerts
Receive the latest developments in plastic and reconstructive surgery. Request the delivery of Plastic and Reconstructive Surgerys e-Alerts directly to your email address. This is a fast, easy, and free service to all subscribers. You will receive: Notice of all new issues of Plastic and Reconstructive Surgery, including the posting of a new issue on the PRS-Online Web site Complete Table of Contents for all new issues Visit www.PRSJournal.com and click on e-Alerts.
1290
You might also like
- Percutaneous Aponeurotomy and Lipofilling: A Regenerative Alternative To Flap Reconstruction?Document11 pagesPercutaneous Aponeurotomy and Lipofilling: A Regenerative Alternative To Flap Reconstruction?Donny Artya KesumaNo ratings yet
- Gox 3 E291Document12 pagesGox 3 E291fer.bpjnNo ratings yet
- From Liposuction To Adipose-Derived Stem Cells IndicationsDocument12 pagesFrom Liposuction To Adipose-Derived Stem Cells IndicationsKikin RizkynnisaNo ratings yet
- Flaps in Maxillofacial ReconstructionDocument29 pagesFlaps in Maxillofacial ReconstructionJaspreet Kaur33% (3)
- Combined Technique of Superficial Liposuction With Ultrasonic Liposculpture PDFDocument8 pagesCombined Technique of Superficial Liposuction With Ultrasonic Liposculpture PDFeiad-mahmoudNo ratings yet
- Full Thickness Skin GraftDocument13 pagesFull Thickness Skin GraftironNo ratings yet
- Nanofat Grafting Basic Research and Clinical.53Document10 pagesNanofat Grafting Basic Research and Clinical.53Luiggi FayadNo ratings yet
- Shoelace Techni e For Delayed Primary Closure of FasciotomiesDocument2 pagesShoelace Techni e For Delayed Primary Closure of FasciotomiesMiguel Angel Lamas RamirezNo ratings yet
- Tensioned Reverse Abdominoplasty: BackgroundDocument8 pagesTensioned Reverse Abdominoplasty: BackgroundlarissaNo ratings yet
- Fingertip and Nail Bed InjuriesDocument27 pagesFingertip and Nail Bed InjuriesiwanbaongNo ratings yet
- Liposuction and Liposculpture: Francesco M. Egro, Nathaniel A. Blecher, J. Peter Rubin, and Sydney R. ColemanDocument9 pagesLiposuction and Liposculpture: Francesco M. Egro, Nathaniel A. Blecher, J. Peter Rubin, and Sydney R. Colemanโสภาพรรณวดี รวีวารNo ratings yet
- Reconstructive Options For The Neck After Resection of Cutaneous MalignanciesDocument10 pagesReconstructive Options For The Neck After Resection of Cutaneous MalignanciesAlvaro Carlos Calvo ValenciaNo ratings yet
- Skin GraftDocument7 pagesSkin GraftrchNo ratings yet
- Adams 2006Document13 pagesAdams 2006AncaVerdesNo ratings yet
- Tom Skin-Sparing Approach To Treatemen of NSTI 2016Document14 pagesTom Skin-Sparing Approach To Treatemen of NSTI 2016Sadaf Raisa KhanNo ratings yet
- Khouri TechniquesDocument12 pagesKhouri Techniquesrandomaeiou7273No ratings yet
- Zingaretti Et Al. 2019Document5 pagesZingaretti Et Al. 2019Walid SasiNo ratings yet
- Hand Rejuvenation With Fat GraftingDocument8 pagesHand Rejuvenation With Fat GraftingMehmet SürmeliNo ratings yet
- Teknik SuturingDocument38 pagesTeknik SuturingrakaNo ratings yet
- TMP 8020Document2 pagesTMP 8020FrontiersNo ratings yet
- Latissimus Dorsi Flap Breast ReconstructionDocument8 pagesLatissimus Dorsi Flap Breast ReconstructionJose Mauricio Suarez BecerraNo ratings yet
- Types of Abdominal IncisionsDocument3 pagesTypes of Abdominal Incisionsjhuzt4_facebook_343onlyNo ratings yet
- BEDAH (Skin Graft)Document7 pagesBEDAH (Skin Graft)Jose FoxNo ratings yet
- Evolution in Tissue Expander Design For Breast Reconstruction: Technological Innovation To Optimize Patient OutcomesDocument10 pagesEvolution in Tissue Expander Design For Breast Reconstruction: Technological Innovation To Optimize Patient OutcomesFauzi Novia Isnaening TyasNo ratings yet
- Nanofat Grafting Basic Research and ClinicalDocument10 pagesNanofat Grafting Basic Research and ClinicalLuiggi FayadNo ratings yet
- Skin GraftDocument38 pagesSkin GraftAndika August100% (1)
- Hammond 2009Document9 pagesHammond 2009edkattaNo ratings yet
- Skin GraftingDocument22 pagesSkin GraftingKumar SuryavanshiNo ratings yet
- Fat Grafting Techniques NotesDocument10 pagesFat Grafting Techniques NotesKonstanța GașperNo ratings yet
- Suturing TechniquesDocument32 pagesSuturing TechniquesRez QNo ratings yet
- Paranoma ExcisionDocument1 pageParanoma ExcisionChrisNo ratings yet
- Transversus Abdominis Release As An AlternativeDocument2 pagesTransversus Abdominis Release As An AlternativeLuiz ViannaNo ratings yet
- Wound HealingDocument40 pagesWound HealingAjay Katiyar100% (1)
- Plastic Surgery: Pablo L. Padilla, Kimberly H. Khoo, Trung Ho, Eric L. Cole, Ramón Zapata Sirvent, Linda G. PhillipsDocument29 pagesPlastic Surgery: Pablo L. Padilla, Kimberly H. Khoo, Trung Ho, Eric L. Cole, Ramón Zapata Sirvent, Linda G. Phillipssportillag1No ratings yet
- Tilleman 2004Document7 pagesTilleman 2004이호원No ratings yet
- Segunda Fase ArticuloDocument7 pagesSegunda Fase ArticuloDanielaNo ratings yet
- Sling LiftDocument6 pagesSling LiftBFF BotoxNo ratings yet
- 2014 Periumbilical Fat Graft A New Resource To Replace Large Volume in The OrbitDocument5 pages2014 Periumbilical Fat Graft A New Resource To Replace Large Volume in The OrbitDimitris RodriguezNo ratings yet
- Skin - Grafts by Madhuri GoreDocument112 pagesSkin - Grafts by Madhuri GoreAnonymous 8hVpaQdCtr100% (1)
- Nava 2006Document8 pagesNava 2006Pasquale ProvaNo ratings yet
- Graft Selection: Full-Thickness Skin GraftDocument8 pagesGraft Selection: Full-Thickness Skin GraftIkhsanNo ratings yet
- Traditional AbdominoplastyDocument23 pagesTraditional AbdominoplastyNguyen DuongNo ratings yet
- Ijomi 15 415Document4 pagesIjomi 15 415Bagis Emre GulNo ratings yet
- Louarn Pascal2010 Article TheHigh Superior TensionTechniDocument9 pagesLouarn Pascal2010 Article TheHigh Superior TensionTechnijuan carlos pradaNo ratings yet
- Mattress SuturesDocument2 pagesMattress SuturesIo DobriNo ratings yet
- Jurnal Scar RevisionDocument8 pagesJurnal Scar Revisionnurul rezki fitrianiazisNo ratings yet
- Fascial Closure-Dumanian2020Document15 pagesFascial Closure-Dumanian2020Kevin QuinterosNo ratings yet
- Utilizing Free Skin Grafts in The Repair of Surgical Wounds: Madalene C. Y. HengDocument11 pagesUtilizing Free Skin Grafts in The Repair of Surgical Wounds: Madalene C. Y. HengDefri ChanNo ratings yet
- Plastic SurgeryDocument6 pagesPlastic SurgeryChaitanya PathakNo ratings yet
- A Simple Technique To Create Spur in Loop Colostomy: Surgeon at WorkDocument3 pagesA Simple Technique To Create Spur in Loop Colostomy: Surgeon at WorkTika Renwarin Tua ElNo ratings yet
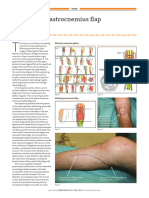
- Pmfaam17 Gastrocnemius BurdDocument4 pagesPmfaam17 Gastrocnemius Burdleidy-riverosNo ratings yet
- The Limited Scar Mastopexy Current Concepts and Approaches To Correct Breast PtosisDocument9 pagesThe Limited Scar Mastopexy Current Concepts and Approaches To Correct Breast PtosisreyllcNo ratings yet
- Episiotomy: By: Charisse Ann G. GasatayaDocument23 pagesEpisiotomy: By: Charisse Ann G. GasatayaCharisse Ann GasatayaNo ratings yet
- Soft Tissue ManagementDocument1 pageSoft Tissue ManagementGautham NaiduNo ratings yet
- Jurnal Oral Maksilo SurgeryDocument41 pagesJurnal Oral Maksilo SurgeryPrima MaulanaNo ratings yet
- Bekas Luka Bakar PDFDocument6 pagesBekas Luka Bakar PDFRiandini PandansariNo ratings yet
- 20SPIGCDocument3 pages20SPIGCscribullNo ratings yet
- MastopexyDocument15 pagesMastopexyLuiggi FayadNo ratings yet
- The Five-Step Lower Blepharoplasty Technique Refined: CosmeticDocument2 pagesThe Five-Step Lower Blepharoplasty Technique Refined: CosmeticNgân Pham KhánhNo ratings yet
- Tissue Engineering and Wound Healing: A Short Case StudyFrom EverandTissue Engineering and Wound Healing: A Short Case StudyRating: 5 out of 5 stars5/5 (2)
- Surat LaborDocument2 pagesSurat LaborYuriko AndreNo ratings yet
- EnchantmentanaDocument50 pagesEnchantmentanamealecsandraNo ratings yet
- TB Statistics and Key Facts Feb 2014Document3 pagesTB Statistics and Key Facts Feb 2014Yuriko AndreNo ratings yet
- How Are We: PresentingDocument44 pagesHow Are We: PresentingMuhammad Zufar Bin MarwahNo ratings yet
- Midgut VolvulusDocument2 pagesMidgut VolvulusYuriko AndreNo ratings yet
- Lampiran A (IKA) PDFDocument1 pageLampiran A (IKA) PDFYuriko AndreNo ratings yet
- Reseach Poster Handout PrintDocument1 pageReseach Poster Handout PrintYuriko AndreNo ratings yet
- Midgut VolvulusDocument2 pagesMidgut VolvulusYuriko AndreNo ratings yet
- Review Of: Equivocal Child AbuseDocument1 pageReview Of: Equivocal Child AbuseYuriko AndreNo ratings yet
- Apa (Ton) Broeders, Ma PHD University of Leiden NL Netherlands Forensic Institute, Rijswijk NLDocument10 pagesApa (Ton) Broeders, Ma PHD University of Leiden NL Netherlands Forensic Institute, Rijswijk NLYuriko AndreNo ratings yet
- Encoded Evidence: Dna in Forensic Analysis: PerspectivesDocument1 pageEncoded Evidence: Dna in Forensic Analysis: PerspectivesYuriko AndreNo ratings yet
- Jfo 12273Document2 pagesJfo 12273Yuriko AndreNo ratings yet
- Jfo 12275Document4 pagesJfo 12275Yuriko AndreNo ratings yet
- Apa (Ton) Broeders, Ma PHD University of Leiden NL Netherlands Forensic Institute, Rijswijk NLDocument10 pagesApa (Ton) Broeders, Ma PHD University of Leiden NL Netherlands Forensic Institute, Rijswijk NLYuriko AndreNo ratings yet
- Uillain Arré Yndrome: L A. M, MDDocument4 pagesUillain Arré Yndrome: L A. M, MDYuriko AndreNo ratings yet
- Forensic Art Guidelines SGFAFI1 ST EdDocument24 pagesForensic Art Guidelines SGFAFI1 ST EdYuriko AndreNo ratings yet
- P ('t':'3', 'I':'669120784') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Document14 pagesP ('t':'3', 'I':'669120784') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Yuriko AndreNo ratings yet
- Withholding or Withdrawing LifeDocument5 pagesWithholding or Withdrawing LifeYuriko AndreNo ratings yet
- KP 1.1.15 Teknik Presentasi IlmiahDocument21 pagesKP 1.1.15 Teknik Presentasi IlmiahfitriahendricoNo ratings yet
- Book Review Forensic Testimony: Science, Law and Expert EvidenceDocument4 pagesBook Review Forensic Testimony: Science, Law and Expert EvidenceYuriko AndreNo ratings yet
- Matriks KegiatanDocument1 pageMatriks KegiatanErni Yessyca SimamoraNo ratings yet
- 772980Document14 pages772980Yuriko AndreNo ratings yet
- P ('t':'3', 'I':'669097626') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Document5 pagesP ('t':'3', 'I':'669097626') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Yuriko AndreNo ratings yet
- Movement DisorderDocument37 pagesMovement DisorderFalcon DarkNo ratings yet
- 3 (Problem-Based Learning)Document36 pages3 (Problem-Based Learning)Ayu AzlinaNo ratings yet
- Uninvestigated Dyspepsia Versus Investigated DyspepsiaDocument3 pagesUninvestigated Dyspepsia Versus Investigated DyspepsiaYuriko AndreNo ratings yet
- Leadership and Teamwork: Rahmatina B. Herman Bagian Pendidikan Kedokteran Fk-UnandDocument22 pagesLeadership and Teamwork: Rahmatina B. Herman Bagian Pendidikan Kedokteran Fk-Unandsandurezu100% (1)
- Eviden BAsed Medicine For PBLDocument33 pagesEviden BAsed Medicine For PBLamiruddin_smartNo ratings yet
- Functional Dyspepsia - Past, Present, and Future (2008)Document6 pagesFunctional Dyspepsia - Past, Present, and Future (2008)Yuriko AndreNo ratings yet
- Evaluation and Management of Dyspepia (1999)Document14 pagesEvaluation and Management of Dyspepia (1999)Yuriko AndreNo ratings yet
- ElectroForce3200 BiomaterialsDocument2 pagesElectroForce3200 BiomaterialsRaja JayakumarNo ratings yet
- Tissue Engineering and Regenerative Medicine 2019: The Role of Biofabrication - A Year in ReviewDocument44 pagesTissue Engineering and Regenerative Medicine 2019: The Role of Biofabrication - A Year in ReviewAlexandra CernencuNo ratings yet
- Bài Báo 3Document10 pagesBài Báo 3HoangNgocAnhNhanNo ratings yet
- Davies JE. Mechanisms of Endosseous Integration. Int J Prosthodont.Document12 pagesDavies JE. Mechanisms of Endosseous Integration. Int J Prosthodont.Santiago Durango HurtadoNo ratings yet
- Different Degradation Rates of Nanofiber Vascular Grafts in Small and Large AnimalDocument35 pagesDifferent Degradation Rates of Nanofiber Vascular Grafts in Small and Large AnimalMadalina CalcanNo ratings yet
- Nucleus Arthroplasty Volume IIDocument55 pagesNucleus Arthroplasty Volume IIHelifunoNo ratings yet
- Biomimetic (Latest)Document127 pagesBiomimetic (Latest)Pawee PiyasowanNo ratings yet
- Endodontics and Pulp Biology: The Impact Clinically: Rci Icw IclcDocument4 pagesEndodontics and Pulp Biology: The Impact Clinically: Rci Icw IclcdrashotiNo ratings yet
- Basics and Applications of Rapid Prototyping Medical ModelsDocument13 pagesBasics and Applications of Rapid Prototyping Medical ModelsSuhas ReddyNo ratings yet
- Seminar Nasional - VII Rekayasa Dan Aplikasi Teknik Mesin Di IndustriDocument4 pagesSeminar Nasional - VII Rekayasa Dan Aplikasi Teknik Mesin Di IndustrizaenalNo ratings yet
- ContohDocument3 pagesContohRueban AntonyNo ratings yet
- Biomedical Applications of Zeolite-Based Materials - A ReviewDocument13 pagesBiomedical Applications of Zeolite-Based Materials - A ReviewNoberto Fontenele FrotaNo ratings yet
- The Global 50 2024 EngDocument333 pagesThe Global 50 2024 EngrebecamorantesNo ratings yet
- 3D Printed PCL-SrHA Scaffold For Enhanced Bone RegenerationDocument12 pages3D Printed PCL-SrHA Scaffold For Enhanced Bone RegenerationDicky Pratama PutraNo ratings yet
- Cultured Meat - WikipediaDocument153 pagesCultured Meat - WikipediaDivya DiyaNo ratings yet
- Bio-Hybrid Implant, Next Generation of Bio-Engineered Implant - A ReviewDocument9 pagesBio-Hybrid Implant, Next Generation of Bio-Engineered Implant - A ReviewPartha Sarathi AdhyaNo ratings yet
- JCR 2021 Q 2 JournalsDocument126 pagesJCR 2021 Q 2 JournalsRhouen RazeNo ratings yet
- Biopolymers and Nanocomposites For Biomedical and Pharmaceutical Applications by Sharmin, Eram Zafar, FahminaDocument180 pagesBiopolymers and Nanocomposites For Biomedical and Pharmaceutical Applications by Sharmin, Eram Zafar, FahminaRizvana HreditaNo ratings yet
- Research Paper 1Document15 pagesResearch Paper 1Puru GaurNo ratings yet
- FabriationDocument8 pagesFabriationBendaud bataborNo ratings yet
- Radiesse For Aesthetic Soft Tissue Augmentation PDFDocument7 pagesRadiesse For Aesthetic Soft Tissue Augmentation PDFfishvalNo ratings yet
- Author's Accepted Manuscript: Ceramics InternationalDocument53 pagesAuthor's Accepted Manuscript: Ceramics InternationalZainab SattarNo ratings yet
- Biology ProjectDocument8 pagesBiology Projectabcd0% (1)
- A Hydrogel - Fiber Scaffold Based On Silk Fibroin - Oxidized Pectin With Sustainable Release of Vancomycin HydrochlorideDocument10 pagesA Hydrogel - Fiber Scaffold Based On Silk Fibroin - Oxidized Pectin With Sustainable Release of Vancomycin Hydrochlorideyeison ocampo rodriguezNo ratings yet
- A Comparison of Micro CT With Other Techniques Used in The Characterization of ScaffoldsDocument15 pagesA Comparison of Micro CT With Other Techniques Used in The Characterization of ScaffoldsMANOJ MNo ratings yet
- Tissue EngineeringDocument32 pagesTissue Engineeringbrian3442No ratings yet
- Names: Maddie Mosscrop, Trevor Nong, Alex Obatake CM: 2537 Assignment: BE570 Lab Protocol Due Date: 5/23/2018Document4 pagesNames: Maddie Mosscrop, Trevor Nong, Alex Obatake CM: 2537 Assignment: BE570 Lab Protocol Due Date: 5/23/2018api-375199340No ratings yet
- PCE ReportDocument27 pagesPCE ReportNikhil ThosarNo ratings yet
- Silk-Its Mysteries, How It Is Made, and How It Is UsedDocument30 pagesSilk-Its Mysteries, How It Is Made, and How It Is UsedassassinoscoreNo ratings yet
- Tissue Engineering For Tissue and Organ RegenerationDocument466 pagesTissue Engineering For Tissue and Organ RegenerationheyguysilikepieNo ratings yet