Professional Documents
Culture Documents
(OS 213) SGD 01 Malignancy (B) - 1
Uploaded by
Yavuz DanisOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
(OS 213) SGD 01 Malignancy (B) - 1
Uploaded by
Yavuz DanisCopyright:
Available Formats
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
SGD 01: MALIGNANCY
Exam 3 | Med Onco Preceptors | August 23, 2012
OUTLINE
Case 1
Case 2
Case 3
Case 4
General Notes
CASE 1
R.S., 50, M
CC: Right lung nodule
o
o
HPI:
2 mo PTC
o CXR done for employment purposes revealed a
solitary pulmonary nodule measuring approx. 2 cm
o Px denied other symptoms except for an
occasional dry, non-productive cough
o diagnosed with PTB and was given anti-TB meds
regularly taken for 2 months
After 2 months
o repeat chest X-ray was done and revealed an
increase in the size of mass to 3cm
o chest CT scan revealed 3.5 x 2.8 cm enhancing
mass at SUPERIOR SEGMENT OF R UPPER LUNG.
o (-) enlarged peribronchial, hilar, mediastinal nodes
o still no other symptoms except for occasional dry
cough
PMHx: Unremarkable (U/R)
PSSx: (+) Smoking: 1 pack/day for 20 years (20 pack
years)
ROS: (-) anorexia, headache, weight loss, back pain,
hemoptysis
PE: (-) palpable lymph nodes, Clear lung fields, U/R
abdomen
Diagnosis
(Note from the transers: Case 1 contains all general data
applicable to lung malignancies. Italicized and underlined
phrases are applicable to Case 1.)
As with diagnosing any disease condition (in this case,
and in all other cases you will encounter), the most
crucial initial step is a thorough history and physical
examination.
By Hx:
Sx of lung cancer can arise from
1.Local mass effects and systemic effects
Symptoms related to tumor itself: hemoptysis and
chest pain
Constitutional non-specific symptoms such as:
anorexia, weight loss, fevers/night sweats
Tumor mass effects such as cough due to nerve
irritation, hoarseness due to compression of
recurrent laryngeal nerve, and facial/upper
extremity syndrome
2.Effects of metastatic disease
bone, pleura, brain, liver, and adrenal glands
3.Effects of products produced by the tumor
(paraneoplastic syndromes).
*Most lung cancers arise in patients with a long
smoking history; the symptoms of cough and dyspnea
are relatively non-specific.
However, an acute
change in previously stable symptoms can be a clue
to an underlying malignancy.
By PE:
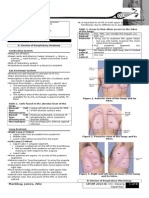
Classic PE findings associated with lung CAs:
Horners syndrome (sympathetic ganglion
dysfunction with ptosis, miosis, enopthalmos and
anhydrosis)
CES, MIKKI, JOLO
A supraclavicular mass due to a Pancoast
tumor (apical tumor involving C8 and T1-2 nerves
causing shoulder pain radiating down to the arm)
SVC syndrome (upper extremity swelling with
or without facial swelling due to vascular obstruction)
Clubbing of fingers and adenopathy suggestive (but not pathognomonic) of an underlying
malignancy.
Table 1. Diagnostic Procedures
Chest X-Ray
tumor in the lungs
enlargement in the mediastinum
due to enlarged lymph node
opacity or white-out lung may
indicate presence of malignancy
or tuberculosis
other thoracic causes
Chest and
localizing tumors, especially
Abdominal CT
central masses not visualized in
Scan
chest X-ray
metastasis (if present)
commonly in the brain and
adrenal glands
determining the presence of fluid
assist in biopsy procedures (CT
GAB)
Positron Emission visualize tumors <1 cm in
Tomography
diameter, malignant lesions and
(PET) Scan
solitary pulmonary nodules
aid in staging mediastinal tumors
R/O active infection (also take up
glucose)
Expensive!
Usually
not
recommended
Bone Scan
detect bone metastasis/es
Magnetic
determine brain metastasis and
Resonance
spinal compression
Imaging (MRI)
rule out (R/O) Potts disease
Chest Ultrasound effusion
locate lung tumors
extent of tumor infiltration
guide needle during thoracentesis
or biopsy.
Histopathology detect cancer cells
special stains (acid fast) to R/O TB
Thoracentesis
drain fluid from pleural effusion
collect samples for histologic
exam,
presence
of
serosanguinous
fluid
is
indicative of malignancy and to
determine if the fluid is a
transudate or exudates
Fine Needle
To collect samples from the
Aspiration Biopsy
lesions that are too large to
(FNAB)
excise for cytologic evaluation
usually CT-guided
Bronchoscopy can also be used if
the lesion is centrally located.
Excision Biopsy if mass is not too large
Pleural Biopsy
samples from pleural tissue
Bronchoscopy
evaluate lung lesions (esp.
central)
investigate unexplained
hemoptysis or adventitious lung
sounds
obtain materials for microbiologic
studies
UPCM 2016 B: XVI, Walang
Kapantay!
1 of 6
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
SGD 01: MALIGNANCY
Exam 3 | Med Onco Preceptors | August 23, 2012
Mediastinoscopy Suprasternal approach to obtain
specimens from mediastinal
nodes
Thoracoscopy
visualizing and biopsy of pleural
and mediastinal nodes
Pulmonary
establish if dyspnea is cardiac or
Function Test
pulmonary in origin
(PFT)
R/O other differentials
CBC
establish if pallor is due to
anemia
determine the patients blood
type if transfusion is needed
(IMPORTANT Note: A patient who is male, >45 years old,
with history of smoking, presenting with a solitary pulmonary
nodule, should always be considered to have lung CA unless
proven otherwise.)
Staging
(Note: See the Lecture
Malignancies for this part.)
trans
on
Overview
of
Lung
Tumor tissue obtained:
By bronchial/transbronchial biopsy
during FOB
2.
By node biopsy during
mediastinoscopy
3.
From operative specimen at the time of
definitive surgical resection
4.
By percutaneous biopsy of enlarged
lymph node, soft tissue mass, lytic bone lesion, bone
marrow or pleural effusion
5.
By FNAB (CT Guided) Preferred for
this Px because of the peripheral location of the
lesion
6.
From adequate cell block from a
malignant pleural effusion
1.
TNM Classification: used in staging NSCLCs
Cancer Staging: Using the TNM guideline: T1 N0 M0
Stage IA
3.5x2.8 cm superior RUL, no note of enlarged
peribronchial, hilar or mediastinal nodes; But needs
other modalities to rule out possible metastasis
(Note: Patients usually come in late or advanced stages,
seldomly early)
Management
Counseling
together with the patients family
3Cs: Coping, Communicating, Connecting
ADVISE TO QUIT SMOKING!!!
Good balanced diet, exercise
Avoid cancer risks: asbestos, radiation
explaining his condition: natural history of the disease
(stage of his disease), prognosis, treatment options
Intervention Options
Surgery - considered if cancer is only small and
localized to one tumor nodule
o Pneumonectomy
o Lobectomy - preferred operation for SCLC
o Segmentectomy
Radiation Therapy - given in patient with SCLC in the
ff situations:
CES, MIKKI, JOLO
In combination with chemotherapy: treat the tumor
and lymph nodes in the chest; improve 3-year
survival rates, especially in patients less than 65
years old
o After chemotherapy: kill any small deposits of
cancer that may remain
Chemotherapy - main treatment for SCLC.
o
(Note: For more complete lists and details on the drugs
used by Lung Cancer patients, see the Lecture trans on
Overview of Lung Malignancies)
Targeted Therapy
Complementary Methods and Palliative Care
Given after chemotherapy sessions and throughout
treatment as an adjunct to therapy, or to reduce the
side effects.
Help the patient feel better and add to patient's
comfort
o Ex. meditation to reduce stress, acupuncture to
relieve
pain,
peppermint
tea
to
relieve
nausea, aromatherapy, massage therapy, yoga.
Pain medication, palliative care, symptomatic therapy
(for difficulty breathing, etc.) can also be given as
necessary.
Group Counseling/Therapy
Follow-Up
Check-up every 2mo post-treatment
CA patients should be educated about signs and
symptoms of recurrence and potential adverse
effects related to therapy
Monitoring with: CXR, Chest CTSc
Liver UTS every 6 months
Bone scan every year
Cranial CTSc if with frequent headache or signs of inc.
ICP
CASE 2
65, M, Filipino
CC: Cough, mild difficulty of breathing, and progressive
hip pain
HPI:
CXR revealed pulmonary mass at the R upper lung with
2 nodules on the L upper and mid-lung fields.
PMHx: U/R
PSSx: (+) smoking: 40 pack years
ROS: (+) facial swelling upon awakening, weight
loss, anorexia
(-) headache, abdominal pain, or hemoptysis
PE: 2x2 cm hard, fixed right supraclavicular node,
decreased breath sounds at the right upper lung field
with dullness to percussion, and occasional inspiratory
wheezing on all lung fields.
Diagnosis
Table 2. Differentials (Case 2)
Disease
Reason for R/I
SCLC
(+) Pulmonary
mass
(+) Cough
(+) Dyspnea
(+) Facial swelling
(plethora)
(+) Weight loss
Smoking hx: 95%
Reason for R/O
(-) ankle edema
(-) muscle
weakness
(-) polyuria,
polydipsia
Facial swelling
improves (in
small cell CA, it
UPCM 2016 B: XVI, Walang
Kapantay!
2 of 6
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
SGD 01: MALIGNANCY
Exam 3 | Med Onco Preceptors | August 23, 2012
NSCLC
(Squamous
cell)
Adenocarcino
ma
of CA associated
with a chronic
smoking Hx is
SCLC
Presence of
nodules at R and
mid-upper lung
field
Hard, fixed R
supraclavicular
node
(+) Pulmonary
mass
(+) Cough
(+) Dyspnea
(+) Facial swelling
(+) Weight loss
Smoking hx
Presence of
nodules at R and
mid-upper lung
field
Age, Sex
(+) Pulmonary
mass
(+) Cough
(+) Dyspnea
(+) Facial swelling
(plethora)
does not
improve due to
constant
hormone
production of
the tumor)
No reason to rule
out
yet
(histopathologic
examination
needed
for
differentiation)
Ancillary
Tests:
paraneoplasms
CES, MIKKI, JOLO
o
o
o
o
o
Adenocarcinoma,
although more
common than
squamous cell
CA, is more
prevalent in
women,
nonsmokers
Mass is central (vs.
Adenocarcinoma
which is more
peripheral)
mainly
Primary Working Impression: non small cell,
squamous cell lung CA
65 yo, M, Smoker, with Pulmonary Mass probably
malignancy!
Cough, dyspnea Common manifestation of
pulmonary disease; could be due to compression of
airway by a mass in this case
Facial swelling upon awakening Could be due to the
compression of the Superior Vena Cava (SVC
syndrome) by the mass on the right upper lung while
on supine position (sleeping)
Weight loss, anorexia Effect of cancer
Two nodules on L upper & mid lung field Metastasis
to the L lung
Hard, fixed R supraclavicular node Nodal metastasis
from R lung
Progressive hip pain Metastasis to the hip bone
Diagnostic Procedures
CXR and Chest CT Scan
Abdominal and Cranial CT Scan, Bone Scan:
detect metastasis
Biopsy: FNAB of the supraclavicular node,
Bronchoscopy of mediastinal lymph nodes (for
possible metastasis; the more specimens, the
better!)
PET scan: detects widespread metastases; but
again, expensive!
Sputum cytology: if (+), R/O head and neck
primary lesions
for
detection
Serum ACTH Cushingoid syndrome; R/O ACTHproducing small cell CA
Blood chemistry, ABG (to look for hypokalemic
alkalosis)
CBC
BUN-Creatinine Clearance: to check whether or
not the kidneys are competent to filter nephrotoxic
CA drugs (platinum waste)
Staging
T4N3M1 Stage IV Lung CA
T4 2 x 2 cm hard supraclavicular node
N3 involvement of mediastinal and contralateral
lymph nodes
M1 presence of metastasis to supraclavicular
node and hip
Very poor Prognosis
Median survival for untreated patients with Stage
IV bronchogenic CA:
4-6 months
5-year survival rate: 2%
Survival time impkroves with chemotherapy and
other targeted therapies
Management
Counseling
(see Case 1 > Management > Counseling)
Intervention Options
Symptomatic Management
o pain: give non-opioids first before moving on to
stronger drugs like morphine when the pain is
already unbearable
o cough (and hemoptysis): can be treated
pharmacologically
Palliative radiotherapy
o FOR: Bronchial obstruction with pneumonitis,
hemoptysis, upper airway or SVC obstruction brain
or spinal cord compression (important!), or
painful bony metastases.
o
It provides relief of intrathoracic symptoms:
o Hemoptysis (84%), SVC syndrome (80%), Dyspnea
(60%), Cough (60%), Atelectasis (23%), Vocal cord
paralysis (6%)
o Also for: cardiac tamponade, painful bony
metastasis, CNS compression, brachial plexus
involvement
Chemotherapy: Palliates symptoms, improves QOL, and
improves survival in newly-diagnosed patients
o First-line: Cisplatin or Carboplateine, Texane
(paclitaxel, docetaxel), Gemicitabine
o Second-line: Docetaxel or pemetrexed
Growth factor support is rarely needed
EGFR Targeted Therapy: Erlotinib (2nd or 3rd line)
o Prolong ssurvival, Second or Third line therapy
o Very expensive
Management for Bone Metastasis
o Radiotherapy
o Bisphosphonates: reduce secondary close, prevent
Complementary Methods and Palliative Care
(Note: In squamous cell lung CA, you will not give
Bevacizumab (which is an angiogenesis inhibitor) will
cause the patient to bleed out)
of
UPCM 2016 B: XVI, Walang
Kapantay!
3 of 6
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
SGD 01: MALIGNANCY
Exam 3 | Med Onco Preceptors | August 23, 2012
CASE 3
52, M
CC: non-productive, associated with back pain.
Pulmonary 10 pack-year
embolism
smoking
(+) unproductive
cough for 1 mo
(+) occasional
pleuritic chest
pain
(+) Hemoptysis
Pneumonia (+) unproductive
cough for 1 mo
(+) occasional
pleuritic chest
pain
HPI:
1 mo PTC
o Non-productive progressing cough, assoc. pleural
chest pain
10 days PTC
o (+) Hemoptysis, Fatigue, Anorexia
PMHx: U/R
PSSx: (+) smoking: 10 pack year
ROS: (+) 30 % weight loss; (-) headache, abdominal
pain, back pain
PE: Slightly cachexic, no palpable nodes, occasional
wheezing at all lung fields
CXR: Large bulky mass with hilar adenopathy
CT Scan:
3x5 cm tumor invading the R main bronchus, 3 cm
distal to carina
Atelectasis at hilar region
Enlarged ipsilateral hilar and mediastinal lymph nodes
Diagnosis
Table 3. Differentials (Case 3)
Disease
Reason for R/I
Reason for R/O
Bronchoge 10 pack-year
nic CA
smoking
(SCLC)
(+) unproductive
cough for 1 mo
(+) occasional
pleuritic chest
pain
(+) Hemoptysis
(+) Anorexia,
weight loss
(+) wheezing in all
lung areas on PE
Large bulky mass
with hilar
adenopathy on
CXR
3x5 tumor invading
R main bronchus
Enlarged ipsilateral
hilar and
mediastinal
lymph nodes
Atelectasis at hilar
region on CT
Pulmonary 10 pack-year
(-) night sweats,
Tuberculosi
smoking
fever
s
(+) unproductive
no tests done for
cough for 1 mo
AFB
smear/culture
(+) occasional
pleuritic chest
pain
(+) Hemoptysis
(+) Anorexia,
weight loss
Large bulky mass
with hilar
adenopathy on
CXR
CES, MIKKI, JOLO
(-) evidence of
effusion
(transudative or
exudative)
no reported
dyspnea
(-) no PE findings
of consolidation,
abnormal breath
sounds
Primary Working Impression: Small cell lung CA
Arises in peribronchial locations and infiltrate the
bronchial submucosa
Usually occurs in the big airways (hilar & central)
Very rapid progression and highly malignant
Smoking is a risk factor (as well as being male)
Common spread is to the mediastinal lymph nodes,
liver, bones, adrenal glands and brain
Diagnostic Procedures
CXR, CT Scan
Biopsy: Bronchoscopy with biopsy, CT scandirected needle biopsy, Endoscopic esophageal
ultrasound w/ biopsy, Mediastinoscopy w/ biopsy,
Open lung biopsy, Pleural biopsy
Ancillary Tests: CBC with platelet count,
Serum electrolytes, glucose, calcium, Liver Function
Tests (ALT, AST), Renal Function Test, ECG, Bone
Scan, PET Scan
Staging
TNM Classification is not used in staging SCLC. Instead,
we describe the malignancy as Limited or Extensive
Limited
o Limited to one side of the chest
o Can be treated with sufficient radiation therapy
o Prognosis: 20 months, 2-year survival rate of 25%,
5-year survival rate of 20%
Extensive
o Spread to other side and/or other distant organs
(including pleural/pericardial effusion or
hematogenous metastases)
o Prognosis: 12 months, 2-year survival rate of 4.6%
Confinement to one Hemithorax Limited-Stage
Disease
Management
Counseling
(see Case 1 > Management > Counseling)
Intervention Options
Chemotherapy:
o Etopside +cisplatin / carboplatin
o CRx doses may be adjusted on the basis of nadir
granulocyte counts
o Blood work +CBC is needed prior to each cycle of
chemotherapy to ensure marrow recovery before
the next dose of chemotherapy is administered.
o Serum LDH is a good marker for response and
should be monitored.
o Renal function should be monitored because of
nephrotoxicity from cisplatin.
o CT scans should be obtained after 2 cycles of
therapy to assess response (if afforded)
UPCM 2016 B: XVI, Walang
Kapantay!
4 of 6
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
SGD 01: MALIGNANCY
Exam 3 | Med Onco Preceptors | August 23, 2012
Radiotherapy
o In combination with Chemotherapy
o Main treatment for our case will consist of
combination Chemotherapy and chest irradiation
(etoposide plus cisplatin plus 45 Gy chest radiation
therapy).
o PROPHYLACTIC BRAIN RADIATION THERAPY
(PBRT)
Lung CA can metastasize to the brain around
60% of controlled lung CA
PBRT reduces the chance of metastasis to the
brain
Px should be advised of the possible cognitive
deficits as a result of PBRT
Supportive and Other Considerations: Antiemetics,
Fluid support with Cisplatin, Monitoring for blood
counts and blood chemistry, signs of bleeding and
infection, Possible Blood Transfusions for the
hemoptysis (if massive), Nutrition therapy for signs
of cachexia, Analgesics (for the pleuritic chest pain),
Cough
suppressants,
if
cough
becomes
uncomfortable, If required, use of hemopoietins
(treatment for anemia)
Complementary Methods and Palliative care
CASE 4
55, M
CC: Chronic cough and weight loss
HPI:
5 mo PTC: chronic cough and weight loss
PMHx:
Ischemic Heart Disease
diagnosed 2 years ago
Tx: isosorbide mononitrate and aspirin
No recent attacks of chest pain
PSSx: (+) smoking, alcohol (occasional)
ROS: (+) occasional hemoptysis, exertional dyspnea,
30% weight loss, anorexia, occasional right
sided pleuritic chest pain
(-) headache, back pain, facial swelling,
abdominal pain, orthopnea, and PND.
PE: pale palpebral conjunctivae, no palpable cervical
or supraclavicular nodes, decreased breath sounds at
the right upper lung fields with dullness to percussion
over said area, and an unremarkable abdomen.
CXR: (+) density at the right apex
Chest CT Scan: 5.5x6.8 cm mass with right perihilar
and subcarinal lymph node enlargement.
Diagnosis
Table 4. Differentials (Case 4)
Disease
Reasons for R/I
Reasons for R/O
NSCLC (+) chronic cough
No reason to rule
(squamous (+) worsening or
out yet
cell CA)
(histopathologic
new dyspnea
al examination
(+) weight loss
of biopsy
(+) hemoptysis
sample needed)
(+) pleuritic pain
(+) decreased
breath sounds;
dull on percussion
CES, MIKKI, JOLO
Cachexia and
weight loss
suggest systemic
spread
Subcarinal and
perihilar
lymphadenopathy
(bronchogenic
CA)
Small cell (+) chronic cough
Usually presents
lung
with central
(+) worsening or
carcinoma
endobronchial
new dyspnea
(SCLC) (+) weight loss
tumor
(-) headache upon
(+) hemoptysis
consult
(+) pleuritic pain
(+) decreased
breath sounds;
dull on percussion
Cachexia and
weight loss
suggest systemic
spread
Pulmonary Smoking hx
(-) night sweating
Tuberculosi (+) cough,
(-) orthopnea,
s
hemoptysis
PND
(+) chest pain
(+) weight loss,
anorexia
(+) perihilar and
subcarinal
lymphadenopathy
(remember
Rankes complex)
Primary Working Impression: Squamous Cell
Carcinoma
Presence of respiratory symptoms due to a possible
lung tumor (cough, dyspnea, hemoptysis - possible
rich blood supply of tumor)
decreased breath sounds at the right upper lung fields
with dullness to percussion
Signs suggesting the presence of a malignancy: weight
loss, anorexia, lymphadenopathy
Imaging studies reveal a mass at the right apex
History of smoking
To rule in: PTB (difficult to rule out unless patient is
asked to have sputum AFB and/or culture)
Diagnostic Procedures
CXR, CT Scan
PET Scan, Cranial and Abdominal CT or MRI,
Bone Scan, CT Scan for Adrenals
CBC with platelet count: check for hemodynamic
stability
o patient presented with pale conjunctive and
hemoptysis, which is not yet quantified.
o Px may present with a bleeding mass due to the
high vascularity of a carcinoma.
Biopsy
Sputum Cytology/Examination if its squamous
cell CA, it is likely that it will be detected using this
procedure
Ancillary tests
Staging
T2bN2M0 Stage IIA
o T2B: Tumor is >5 cm, does not directly involve
carina; invades visceral pleura
UPCM 2016 B: XVI, Walang
Kapantay!
5 of 6
OS 213: Human Disease Treatment 3 (Circulation
and Respiration)
SGD 01: MALIGNANCY
Exam 3 | Med Onco Preceptors | August 23, 2012
o
o
N2: metastasis to ipsilateral mediastinal and/or
subcarinal lymph nodes
M0: no distant metastasis (based on PE findings;
ideal = radiographic image of lymph nodes)
Management
Counseling
(see Case 1 > Management > Counseling)
Intervention Options
Surgical resection with lymph node dissection
o may have poor results because of node
involvement
o Some oncologist conclude that surgery should only
be conducted in patients who have clearing of the
mediastinal nodes after adjuvant therapy
Chemotherapy followed by Radiation Therapy (Tx
of choice)
o Cisplatin-based combination (with etoposide)
o Improved survival compared with sequential
therapy but more side effects such as fatigue,
esophagitis and neutropenia
Supportive Therapy: Pain relief, Emesis therapy,
Ondansetron, Prochloroperazine, Dexamethasone,
Nutritional intervention
Complementary Methods and Palliative Care
GENERAL NOTES
On History and PE:
Getting a good history and PE is important since
most CAs metastasize to the lungs. For women, usually
comes from breast cancer, and for men, rectal cancer.
Before doing treatment for Lung CA, always check for
CA in other locations.
On Doing a Biopsy
Do a biopsy to check for possible malignant cells
then classify what type of cancer; always opt for the
most accessible biopsy (e.g. lymph node)
FNAB
CT-guided biopsy (CT GAB): for peripheral masses
Bronchoscopy-guided biopsy: for central (hilar or
mediastinal) masses
VATS as a last resort if you're absolutely positive that
there's a malignancy but other the methods have
failed to give a positive result
On Staging and Treatment:
Stage dictates treatment
Stage 1: Surgery then chemo (Don't do radio)
Stage 2: Surgery
Stage 3A: Chemotherapy then surgery
Stage 4: Chemotherapy and Radiotherapy;
palliative
On Other diagnostics:
Do a brain CT scan for small cell carcinoma because it
is very malignant
CES, MIKKI, JOLO
Sputum cell cytology is seldom used as a diagnostic
measure; do biopsy instead
On Patient Workups:
Before doing biopsies, do PT, PTT test to see if there
are any bleeding disorders
Must have cardiopulmonary clearance (ECG, etc.)
before having a bronchoscopy
Platinum-containing anti-cancer drugs are nephrotoxic
(also hepatotoxic) - check kidney function via
BUN/Creatinine
CBC is done to see if the patient has recovered from
chemotherapy
On Other Treatment:
Chemotherapy and Radiotherapy requires good
performance status (i.e. children) otherwise the
patient might die from the treatment
Erythropoietin transfusion can increase the risk of
stroke and ischemia if given at the wrong dose.
Proper regimen is high dose erythropoietin once a
week.
Combine chemotherapy with other forms of therapy
like anti-angiogenesis drugs and radiotherapy, etc.
Leads to a better outcome
Others:
Sarcoidosis is rarely a viable differential in the
Philippines
Always get a good history; the lung malignancy might
only be secondary
END
Ces: Here it is, from 9 pages of pure redundancy,
tenen! Haay. Antoxic tuloy magreorganize. Tinoxic ko
rin yata ang sarili ko sa pag-aayos ng isang trans na
hindi naman babasahin ng mga tao. T___T Sana ganito
pa rin ung cases sa future, para purposeful naman ang
pagpapaka-OC ko sa trans na to. Haha. Kung hindi,
ohwell.
At dahil smileys na lang ang greetings nina Mikki at
Jolo, uubusin ko na lang ang space na to. Not. Kalahati
na lang siguro.
Hello Block B! Kumusta naman ang weekly transing
natin?
Hello 2016! 2nd place ang EPIMERS sa FATE! XVI:
Walang Kapantay!
Hello Medchoir 2016! Fun fun fun (and eat eat
EAAAAT!) in San Juan! Sana next time makapunta na
tayong lahat for more chikahan. Hahaha! Mag-ipon na
lang muna tayo ng mga ala-The Buzz na mga tanong
sa ngayon. ;)
Mikki, Jolo:
UPCM 2016 B: XVI, Walang
Kapantay!
6 of 6
You might also like
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- (OS 213) LEC 03 Review of Normal Lung Structure and FunctionDocument8 pages(OS 213) LEC 03 Review of Normal Lung Structure and FunctionYavuz DanisNo ratings yet
- LogmakDocument2 pagesLogmakYavuz DanisNo ratings yet
- A Durable Ultrasound Phantom For Trainees Using Common MaterialsDocument7 pagesA Durable Ultrasound Phantom For Trainees Using Common MaterialsYavuz DanisNo ratings yet
- TI Analog HandbookDocument101 pagesTI Analog HandbookJenory DenemyNo ratings yet
- 2016 May - NCDocument36 pages2016 May - NCYavuz DanisNo ratings yet
- Diagnostic Procedures in Ophthalmology Full ColourDocument488 pagesDiagnostic Procedures in Ophthalmology Full ColourAnquito100% (4)
- (Os 213) Lec 05.2 Drugs For RtiDocument1 page(Os 213) Lec 05.2 Drugs For RtiYavuz DanisNo ratings yet
- Radio 25 E1 Lec 10 MSK RadiologyDocument3 pagesRadio 25 E1 Lec 10 MSK RadiologyYavuz DanisNo ratings yet
- (OS 213) LEC 03 Review of Normal Lung Structure and FunctionDocument8 pages(OS 213) LEC 03 Review of Normal Lung Structure and FunctionYavuz DanisNo ratings yet
- (OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Document16 pages(OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Yavuz DanisNo ratings yet
- 5 Medicine OSCE Collection: By: Fatimah Al-IbrahimDocument69 pages5 Medicine OSCE Collection: By: Fatimah Al-IbrahimJim JordenNo ratings yet
- (Os 213) Pictotrans Ws 02 - Ecg Skills Enhancement (A)Document16 pages(Os 213) Pictotrans Ws 02 - Ecg Skills Enhancement (A)Yavuz DanisNo ratings yet
- (OS 213) LEC 15 Surgery For Peripheral Vascular Diseases I (B)Document8 pages(OS 213) LEC 15 Surgery For Peripheral Vascular Diseases I (B)Yavuz DanisNo ratings yet
- (OS 213) LEC 15 Pneumonia (B) - 1Document7 pages(OS 213) LEC 15 Pneumonia (B) - 1Yavuz DanisNo ratings yet
- (OS 213) LEC 10 Rheumatic Fever and RHD (B)Document6 pages(OS 213) LEC 10 Rheumatic Fever and RHD (B)Yavuz DanisNo ratings yet
- (OS 213) LEC 13 Paragonimus Westermani (A)Document4 pages(OS 213) LEC 13 Paragonimus Westermani (A)Yavuz DanisNo ratings yet
- (Os 213) Lec 09 TB Dots (A)Document2 pages(Os 213) Lec 09 TB Dots (A)Yavuz DanisNo ratings yet
- RADIO 250 (8) LEC 11 Introduction To Interventional RadiologyDocument6 pagesRADIO 250 (8) LEC 11 Introduction To Interventional RadiologyYavuz DanisNo ratings yet
- (OS 213) LEC 02 Cardinal Symptoms of Heart Disease (A)Document14 pages(OS 213) LEC 02 Cardinal Symptoms of Heart Disease (A)Yavuz DanisNo ratings yet
- (OS 213) CASE 01 Case PresentationsDocument3 pages(OS 213) CASE 01 Case PresentationsYavuz DanisNo ratings yet
- (OS 213) LAB 03 Paragonimus Westermani (A)Document3 pages(OS 213) LAB 03 Paragonimus Westermani (A)Yavuz DanisNo ratings yet
- (OS 213) LAB 03 Paragonimus Westermani (B) - 2Document3 pages(OS 213) LAB 03 Paragonimus Westermani (B) - 2Yavuz DanisNo ratings yet
- RADIO 250 (8) LEC 08 Genitourinary Pelvis RadiologyDocument14 pagesRADIO 250 (8) LEC 08 Genitourinary Pelvis RadiologyYavuz DanisNo ratings yet
- CVS Course Summary: Anatomy, Diseases, TreatmentsDocument12 pagesCVS Course Summary: Anatomy, Diseases, TreatmentsYavuz DanisNo ratings yet
- RADIO 250 (8) LEC 09 Musculoskeletal RadiologyDocument4 pagesRADIO 250 (8) LEC 09 Musculoskeletal RadiologyYavuz DanisNo ratings yet
- Radio 250 E1 Lec 01 Intro To Radiology and RadioprotectionDocument6 pagesRadio 250 E1 Lec 01 Intro To Radiology and RadioprotectionYavuz DanisNo ratings yet
- Radio 250 (8) Lec 05 Gi RadiologyDocument11 pagesRadio 250 (8) Lec 05 Gi RadiologyYavuz Danis100% (1)
- (OS 213) LEC 09 Physical Diagnosis of The Respiratory System (B) - 2Document8 pages(OS 213) LEC 09 Physical Diagnosis of The Respiratory System (B) - 2Yavuz DanisNo ratings yet
- (OS 213) LEC 11 Viral and Fungal Diseases of The Lung (A)Document7 pages(OS 213) LEC 11 Viral and Fungal Diseases of The Lung (A)Yavuz DanisNo ratings yet
- (OS 213) LEC 10 Rheumatic Fever and RHD (B)Document6 pages(OS 213) LEC 10 Rheumatic Fever and RHD (B)Yavuz DanisNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Principles of SamplingDocument15 pagesPrinciples of SamplingziggerzagNo ratings yet
- Accidental PoisoningDocument3 pagesAccidental PoisoningBRUELIN MELSHIA MNo ratings yet
- Design and Analysis of Algorithms Prof. Madhavan Mukund Chennai Mathematical Institute Week - 01 Module - 01 Lecture - 01Document8 pagesDesign and Analysis of Algorithms Prof. Madhavan Mukund Chennai Mathematical Institute Week - 01 Module - 01 Lecture - 01SwatiNo ratings yet
- Electrophoresis and Fractionation of Wheat GlutenDocument14 pagesElectrophoresis and Fractionation of Wheat GlutensecucaNo ratings yet
- Riedijk - Architecture As A CraftDocument223 pagesRiedijk - Architecture As A CraftHannah WesselsNo ratings yet
- Using Snapchat For OSINT - Save Videos Without OverlaysDocument12 pagesUsing Snapchat For OSINT - Save Videos Without OverlaysVo TinhNo ratings yet
- Delhi Public School: Class: XI Subject: Assignment No. 3Document1 pageDelhi Public School: Class: XI Subject: Assignment No. 3Aman Kumar BhagatNo ratings yet
- Rubric - Argumentative EssayDocument2 pagesRubric - Argumentative EssayBobNo ratings yet
- Bethany Getz ResumeDocument2 pagesBethany Getz Resumeapi-256325830No ratings yet
- OLA CAB MARKET ANALYSIS AND TRENDSDocument55 pagesOLA CAB MARKET ANALYSIS AND TRENDSnitin gadkariNo ratings yet
- Useful Coaching Questions: Questions To Create A State Change Questions To Ask When Something Goes WrongDocument2 pagesUseful Coaching Questions: Questions To Create A State Change Questions To Ask When Something Goes WrongAntonioNo ratings yet
- PGP TutorialDocument21 pagesPGP TutorialSabri AllaniNo ratings yet
- Linguistics: Chapter 1 - 10Document41 pagesLinguistics: Chapter 1 - 10Ahmad A. JawadNo ratings yet
- Where On Earth Can Go Next?: AppleDocument100 pagesWhere On Earth Can Go Next?: Applepetrushevski_designeNo ratings yet
- 256267a1Document5,083 pages256267a1Елизавета ШепелеваNo ratings yet
- DANZIG, Richard, A Comment On The Jurisprudence of The Uniform Commercial Code, 1975 PDFDocument17 pagesDANZIG, Richard, A Comment On The Jurisprudence of The Uniform Commercial Code, 1975 PDFandresabelrNo ratings yet
- Manual Bombas CHWDocument16 pagesManual Bombas CHWFred GarciaNo ratings yet
- R4 User GuideDocument48 pagesR4 User GuideAaron SmithNo ratings yet
- Mole Concept - DPP 09 (Of Lec 13) - Yakeen 2.0 2024 (Legend)Document3 pagesMole Concept - DPP 09 (Of Lec 13) - Yakeen 2.0 2024 (Legend)Romeshchandra Class X-CNo ratings yet
- Manju Philip CVDocument2 pagesManju Philip CVManju PhilipNo ratings yet
- AIATS 2021 (OYMCF) Test 01 Offline - Code A - SolutionsDocument34 pagesAIATS 2021 (OYMCF) Test 01 Offline - Code A - Solutionsbhavyakavya mehta100% (1)
- Castel - From Dangerousness To RiskDocument10 pagesCastel - From Dangerousness To Riskregmatar100% (2)
- Conserve O Gram: Understanding Histograms For Digital PhotographyDocument4 pagesConserve O Gram: Understanding Histograms For Digital PhotographyErden SizgekNo ratings yet
- The Polynesians: Task1: ReadingDocument10 pagesThe Polynesians: Task1: ReadingHəşim MəmmədovNo ratings yet
- CV Abdalla Ali Hashish-Nursing Specialist.Document3 pagesCV Abdalla Ali Hashish-Nursing Specialist.Abdalla Ali HashishNo ratings yet
- Digital Citizenship Initiative To Better Support The 21 Century Needs of StudentsDocument3 pagesDigital Citizenship Initiative To Better Support The 21 Century Needs of StudentsElewanya UnoguNo ratings yet
- Korba - BAH Online Temp MonitoringDocument7 pagesKorba - BAH Online Temp Monitoringrama jenaNo ratings yet
- Research Paper On Organ DonationDocument8 pagesResearch Paper On Organ Donationsheeliya whiteNo ratings yet
- Philippine College of Northwestern Luzon Bachelor of Science in Business AdministrationDocument7 pagesPhilippine College of Northwestern Luzon Bachelor of Science in Business Administrationzackwayne100% (1)
- English Skills BookDocument49 pagesEnglish Skills BookAngela SpadeNo ratings yet