Professional Documents
Culture Documents
The Epidemiology of Stillbirth
Uploaded by
Nenny Yoanitha DjalaCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The Epidemiology of Stillbirth
Uploaded by
Nenny Yoanitha DjalaCopyright:
Available Formats
The Epidemiology of Stillbirth
Sven Cnattingius and Olof Stephansson
Stillbirths account for an increasing proportion of feto-infant mortality. Yet, causes of stillbirth are
rarely reported, and the causes of most stillbirths remain unknown. Few studies focus specifically on
the epidemiology of stillbirth. Major risk factors include high maternal age, smoking, and overweight.
The prevalence of delayed childbearing and, especially overweight, are increasing in most developed
countries. The proportion o f stillbirth attributable to overweight is likely to increase.
Copyright 9 2002 by W.B. Saunders
tillbirth currently accounts for m o r e than
S one third of all feto-infant mortality and
m o r e than 50% o f all perinatal deaths in develo p e d countries. 1,2 A m o n g n o n m a l f o r m e d fetuses/infants, stillbirth at 28 c o m p l e t e d gestational weeks or later accounts for m o r e than
50% of all feto-infant m o r t a l i t y ) Moreover, the
causes of stillbirth differ f r o m those of early
neonatal mortality, z,4 Despite the clear importance of stillbirth as a public health problem, few
studies have focused specifically on the epidemiotogy and cause of stillbirth.
Causes
In contrast to infant mortality, causes of stillbirth
are generally not registered i n vital statistics or
population-based research registers. T h e r e are
also substantial difficulties in d e t e r m i n i n g the
cause of stillbirth. First, weight a n d gestational
length are, in the case of a stillbirth, estimated at
delivery and not at time of death. This leads not
only to an overestimation of gestational length,
but the fetus may also have lost weight after
death. Thus, the i m p o r t a n c e of low birth weight
in relation to gestational age may therefore be
overestimated in stillbirth. Second, even if diagnostic investigations are p e r f o r m e d , there may
be difficulties in achiex4ng valid results. Pathological investigations must consider possible
changes occurring between the often u n k n o w n
time of death and time of investigation. W h e n
looking for an infectious cause, it may be unknown what infections should be considered lethal, and infections may also occur during or
after delivery.
A n u m b e r of m e t h o d s of g r o u p i n g causes of
death in stillbirth a n d neonatal deaths have
b e e n used. 5,6 T h e cause of stillbirth differs in
m a n y cases f r o m the cause of neonatal deaths,
which necessitates a specific classification system
for stillbirth. More importantly, diagnostic routines generally differ substantially between hospitals, and a successful classification of causes of
stillbirth is highly d e p e n d e n t on a standardized
and systematic clinical procedure. As m o r e than
1 factor may contribute to fetal death, m a n y
classifications have recognized the n e e d for a
hierarchical classification system, in which potentially lethal anomalies take p r e c e d e n c e over
other conditions. 5,6 Two o t h e r i m p o r t a n t causes
of stillbirth are prenatal infections, and above
all, fetal growth retardation. O t h e r causes include isoimmunization, abruptio placenta, maternal chronic diseases, pregnancy-related disorders (such as preeclampsia and gestational
diabetes), and umbilical cord accidents. Yet, despite all these possible causes o f stillbirth, a
substantial p r o p o r t i o n of stillbirths r e m a i n
unexplained. However, within the g r o u p of "unexplained" stillbirths, there is probably a relatively large g r o u p of fetuses with undiagnosed
fetal malnutrition, c h r o m o s o m a l aberrations, or
infections.
Stillbirth and G e s t a t i o n a l A g e
W h e n stillbirth is defined as a fetal death occurring at 20 weeks or later, 82% of all stillbirths are
r e p o r t e d to occur in the p r e t e r m period. 7 Also,
when stillbirth is defined as fetal death at 24
weeks or later or even at 28 weeks or later, the
From the Department of Medical Epidemiology, Karolinska Instituter, Stockholm.
Address ~'eprint requests to Sven Cnattingius, MD, PhD, Department
of Medical Epidemiology, Karolinska Instituter, PO Box 281, SE171 77 StockhoZm; e-mail: Sven. Cnattingius@mep.ki.se.
Copyright 9 2002 by W.B. Saundev's
O146-0005/02/2601-0005535. 00/0
doi:l O.1053/sper.2002.29841
Seminars in Perinatology, Vol 26, No 1 (February), 2002: pp 25-30
25
Cnattingius and Stephansson
26
majority of stillbirth occur preterm. 8,9 Since the
majority of stillbirths occur preterm, it may seem
paradoxical that the risk of stillbirth increases
with gestational age. However, as p o i n t e d out by
Yudkin et al, 1~ fetuses at risk of stillbirth at a
specific gestational age must include all live fetuses at that gestational age. By using this approach, Yudkin et aP ~ showed a consistent increase in risk of stillbirth by gestational age (Fig
1), an observation that has b e e n c o n f i r m e d by
o t h e r investigators, n,12 Thus, the risk of stillbirth
may be highest in the postterm period, which to
a large extent can be explained by increased
rates of small-for-gestational-age fetuses b o r n
postterm. 1~
Risk F a c t o r s
Maternal Age
T h e r e is g o o d evidence that it is b e c o m i n g increasingly c o m m o n a m o n g w o m e n to choose to
delay childbearing. In the United States, the
p r o p o r t i o n of first-time mothers who were age
30 or older increased f r o m 4% in 1969 to 21% in
1994.14 -The t r e n d of delayed childbearing has
occurred primarily a m o n g w o m e n with at least
high school education and is attributed to
w o m e n voluntarily p o s t p o n i n g pregnancies for
personal or professional reasons. Several large
epidemiological studies have r e p o r t e d that high
2,0
1s
1,e
o
Q
1,4
1,2
~, 0,8
0,6
Table 1. Odds Ratio (OR) and 95% Confidence
Intervals (CI) for Stillbirth by Maternal Age
Age (years)
OR
(95 % CI)
(reference group)
<30
1.0
30-34
1.3
(0.9-1.7)
35-39
40+
1.9
2.4
(1.3-2.7)
(1.3-4.5)
Data from reference 16.
m a t e r n a l age increases the risk of stillbirth. 15,16
Fretts et aP 6 r e p o r t e d that, c o m p a r e d to w o m e n
below 30 years, the risk of fetal d e a t h a m o n g
w o m e n aged 35 to 39 years was almost increased
24bld, while c o r r e s p o n d i n g risk for those 40 or
older was m o r e than doubled (Table 1). T h e risk
of stillbirth is especially p r o n o u n c e d a m o n g delayed childbearers, but probably also increased
a m o n g older parous women. Although the risks
of pregnancy-related disorders or complications,
such as preeclampsia, gestational diabetes, a n d
abruptio placenta increase with age, the agerelated increase in stillbirth cannot be explained
by these diseases, a2,a6 T h e age-related stillbirth
risk increases with advancing gestational age,
and older w o m e n have above all an increased
risk of u n e x p l a i n e d s t i l l b i r t h / A l t h o u g h the absolute increase in risk for the individual w o m a n
may be considered modest, the i m p a c t of delayed childbearing becomes m o r e i m p o r t a n t as
the p h e n o m e n o n b e c o m e s m o r e prevalent.
T e e n a g e pregnancies are, in contrast to high
m a t e r n a l age, m o r e associated with neonatal
death than stillbirthJ 7 This is not surprising,
since the risk of p r e t e r m birth, and especially
very p r e t e r m birth, is increased a m o n g teenage
childbearers (and especially very y o u n g teenagers), while the association between restricted
fetal growth and teenage childbearing is m o r e
controversial.IS
Parity
0,4
0,2
0,0
29
31
33
35
37
39
41
Gestationel age (weeks)
Figure l. Rate of stillbirth by gestational age, per
1,000 live fetuses at that gestational age. (Reprinted
with permission. I~)
Studies have r e p o r t e d an increased rate of stillbirth a m o n g nulliparas and g r a n d multiparas. n,m However, in 1 study, the U-shaped pattern between parity and stillbirth risk was,
a m o n g older women, evident in the t960s a n d
early 1970s, but not in the late 1970s and
1980s/6 T h e authors suggest that the reduction
in the parity-related risk of stillbirth over time
Epidemiology of Stillbirth
may be due to i m p r o v e d access to medical care
and changes of obstetrical practice.
Smokmg
T h e association between smoking and stillbirth
risk is well known and there is probably a causal
association. First, the risk of stillbirth increases
with the a m o u n t smoked. 2,2~ Second, there is a
supportive biological hypothesis. Smoking during pregnancy increases fetal carboxihemoglobin concentration and increases the vascular resistance, because of the vasoconstrictive effect of
nicotine and the r e d u c e d prostacyclin synthesis. 2~-23These toxic effects of tobacco smoke may
partly explain the causal association between
smoking and r e d u c e d fetal growthY 4 These effects may also contribute to the placental
changes a m o n g smokers, such as decidual necrosis, which in turn may lead to abruptio placenta. 25"26 In a study of Meyer a n d Tonascia, 27
the elevated risk of fetal death in smokers was
largely because of higher rates of placental abruption and placenta previa. A n o t h e r study
f o u n d a 40% overall increased risk of stillbirth
a m o n g smokers, but smokers who did not suffer
f r o m placental complications or delivered
growth retarded infants had no increased risk of
stillbirth, t2 Thus, it appears that the association
between smoking and stillbirth is explained by
the smoking-related risks of fetal growth retardation and placental complications. Third, the
hypothesis of a causal association between smoking during pregnancy and stillbirth is further
s t r e n g t h e n e d by a recent Danish study, reporting that smoking cessation in the first trimester
reduces the risk of stillbirth c o r r e s p o n d i n g to
that of nonsmokers. 23 This result also indicates
that smoking exerts its influence on stillbirth
after the first trimester. Smoking has b e e n rep o r t e d to primarily influence risk of p r e t e r m
stillbirth, ~2 and these results are in turn supp o r t e d by a finding that intrauterine growth retardation is a stronger risk factor for p r e t e r m
than for term stillbirth, s
Although the prevalence of smoking during
p r e g n a n c y has declined in m a n y countries, still
between 10% to 30% of the p r e g n a n t population in the western world smoke. 23,29 Thus,
smoking continues to be one of the most important preventable risk factors for stillbirth.
27
Maternal Body-mass Index
An association between maternal body-mass index (BMI) and stillbirth risk, with the highest
risk a m o n g overweight and obese w o m e n was
r e p o r t e d in 1993. 2o A Swedish register-based
study confirmed this and f o u n d that the association between increasing BMI and stillbirth risk
was highest a m o n g nutliparous women. 3~ A recent Swedish study on a n t e p a r t u m stillbirths
f o u n d that the association between early pregnancy BMI and stillbirth risk was strongest for
term stillbirths, suggesting an increasing effect
of a high BMI by gestational length. 31 T h e mechanisms for the BMI-related increases in risk of
stillbirth remain a matter of speculation. Overweight and obese w o m e n are m o r e likely to have
a low socio-economic status a n d are m o r e often
cigarette smokers. Pregnancy complications,
such as gestational diabetes, preeclampsia, and
eclampsia, are m o r e c o m m o n a m o n g overweight
and obese women. After excluding cases and
controls with weight-related pregnancy complications, the risk of stillbirth r e m a i n e d increased
a m o n g overweight women, but was attenuated
a m o n g obese w o m e n (Table 2). 3~ T h e prevalence of overweight and obesity is rising rapidly
in developed countries (Fig 2), 32 and in the
United States a third of the p r e g n a n t population
are overweight (BMI > 25). as If causal, overweight may f r o m a public health perspective be
the most i m p o r t a n t risk factor for stillbirth.
Table 2. Odds Ratio (OR) and 95% Confidence
Intervals (CI) for Antepartum Stillbirth by Bodymass Index (BMI) Among Nulliparous Women
All Cases and
Controls
(n = 613/660)*
BMI
-<19.9++
20.0-24.9
25.0-29.9
-->30.0
Excluding Cases
and Controls With
Gestational
Diabetes and
Preeclampsia
(n = 461/546)*
OR~
(95 % CI)
OR~
(95 % CI)
1.0
1.2
1.9
2.1
(0.8-1.7)
(1.2-2.9)
(1.2-3.6)
1.0
1.2
2.5
1.5
(0.8-1.8)
(1.5-4.0)
(0.7-3.0)
* Number of cases/controls.
t Adjusted for age, height, occupation, and cigarette smoking.
++Reference group.
Data from reference 31.
Cnattingius and Stephansson
28
%
20
15
D MI 25.0-29,9
[] BMI 30.0-34.9
10
[] BMI 35.0+
5
0
1960-62
1971-74
1976-80
1988-94
Figure 2. Prevalence of overweight and obesity
among women aged 20-29 years, United States 19601994. (Data from reference 32.)
Maternal Weight Gain During Pregnancy
Few studies have investigated the association between weight gain during pregnancy and stillbirth risk. Weight gain is related to prepregnancy BMI, and w o m e n with a high BMI gain
less weight during p r e g n a n c y ? T M Therefore, it
is i m p o r t a n t when analyzing the association between weight gain a n d risk of stillbirth to consider p r e p r e g n a n c y BMI as a c o n f o u n d i n g factor. Taffel et a135 showed an association between
low m a t e r n a l weight gain and stillbirth risk,
whereas-this was not f o u n d by Rydhstr6m et al. ~6
However, n o n e of these studies simultaneously
investigated the possible influences by other covariates. A recent Swedish study was able to take
such confounders into account and f o u n d no
association between pregnancy weight gain a n d
a n t e p a r t u m stillbirth risk. 31
Socio-economic Factors
Although it is generally known that socio-economic status influences stillbirth risk, 2~ the reasons remain essentially unknown. This is not
entirely because most studies have included few
covariates, but results f r o m a recent study suggest that the reasons for the association may be
h a r d to disentangle. 9 T h e group of w o m e n f r o m
low social class was favored by a reduced prevalence of delayed childbearers, but, on the o t h e r
hand, they were m o r e often smokers and overweight. Thus, the risks of stillbirth related to low
socio-economic status, were after adjustment for
maternal age, smoking and body mass index,
essentially the same as the crude risks. Moreover,
further adjustments for time of admittance to
antenatal care, n u m b e r of visits to prenatal care,
and a n u m b e r of o t h e r covariates, did not essentially c h a n g e these risks, n o r were the risks
e x p l a i n e d by i n c r e a s e d rates o f small-for-
gestational-age pregnancies or pregnancy-related disorders a m o n g w o m e n f r o m low social
class9 Residual c o n f o u n d i n g of alcohol a n d illicit drug use is a possible but not p r o b a b l e
explanation. Since the risk related to low social
class was primarily increased for t e r m stillbirth,
one may hypothesize whether these differences
are due to subtle differences in care.
Recurrent Stillbirth
T h e tendency to repeat pregnancy o u t c o m e s in
successive births is well known and also includes
risk of stillbirth. W o m e n with a previous stillbirth may, c o m p a r e d to w o m e n with no previous
stillbirth, have a 6 to 10-fold increased risk of
stillbirth in next pregnancy. 37,3s Although recurrence of stillbirth is m o r e c o m m o n a m o n g
w o m e n with diabetes or pregnancy-induced hypertensive diseases, and may also be associated
with recurrence of fetal growth retardation, such
factors probably only partly explain the risk of
repeating stillbirth, s7-~9
Maternal Hemoglobin Concentration
During normal pregnancy, the h e m o g l o b i n concentration falls until the 20th week of gestation,
remains fairly constant up to 30 weeks and thereafter rises slightly. These changes in h e m o g l o b i n
concentration are mainly due to an increased
plasma volume. In developed countries, b o t h
high a n d low h e m o g l o b i n concentration during
p r e g n a n c y have b e e n associated with small-forgestational-age and p r e t e r m births. Two studies
have r e p o r t e d increased rates of perinatal death
with b o t h low and high h e m o g l o b i n concentration during pregnancy, 4~ and 1 study f o u n d a
similar u-shaped association for stillbirth rates. 42
In a recently published study the risk of stillbirth
was increased for b o t h low (--<115 g / L ) and high
(>--146 g / L ) early pregnancy h e m o g l o b i n concentration, 43 and a relatively large decrease in
h e m o g l o b i n concentration during p r e g n a n c y
t e n d e d to be protective. T h e risk related to high
h e m o g l o b i n values was confined to a n t e p a r t u m
stillbirths without malformations, and especially
p r o n o u n c e d if the fetus also was growth-retarded (Table 3). T h e biological m e c h a n i s m for
the increased risk of stillbirth for high h e m o g l o bin concentration may be that plasma expansion
enhances fetal growth. T h e r e d u c e d b l o o d viscosity may favor b l o o d flow in the m a t e r n a l in-
Epidemiology of Stillbirth
T a b l e 3. O d d s Ratio (OR) a n d 95% C o n f i d e n c e
Intervals (CI) for Stillbirth by H e m o g l o b i n
C o n c e n t r a t i o n in First T r i m e s t e r
Antepmr
Stillbirth Without
Malformations
All
(n = 519/610)*
SGA-stillbirths
(n = 137/390)*
First Hb g/L
ORt
(95% CI)
OR?
(95% CI)
--<115
116-125
126-135 (ref.)
136-145
-->146
1.7
0.9
1.0
1.0
2.0
(1.0-2.8)
(0.6-1.2)
1.5
0.4
1.0
1.1
4.2
(0.6-3.9)
(0.2-0.8)
(0.7-1.4)
(1.1-3.8)
(0.6-2.1)
(1.3-13.9)
* Number of cases and controls.
t Adjusted for age, height, BMI, occupation, smoking, early
pregnancy weekly change in Hb, and week of first Hb measurement.
Source: Stephanssou et al. JAMA 2000;284:2611-7.
tervillous space and prevent thrombosis in the
uteroplacental circulation.
Multiple Birth
Since twins are m o r e likely to be growth-retarded and to be delivered preterm, they have an
increased risk of stillbirth and (above all) neonatal death. A particular concern is monozygotic
twins, who have p o o r e r survival than dizygotic
twins. 44,45 If 1 twin dies in utero, the cotwin is n o t
only at increased risk of fetal death, but also runs
an increased risk of cerebral palsy and o t h e r
cerebral impairments. 44 The relative i m p o r t a n c e
of twin pregnancy as a risk factor for stillbirth is
likely to increase, as the rate of twin pregnancies
are increasing. 46
Conclusions
In contrast to infant mortality, the decline in
stillbirth rates have, in most countries, b e e n less
obvious. The majority of stillbirths dies unexpectedly preterm, when possibilities to detect
warning signs, such as fetal growth restriction,
are limited. Major maternal risk factors include
m a t e r n a l smoking, high maternal age, and overweight, but why high maternal a g e and overweight influence stillbirth risk remains to be
determined. In contrast to smoking, the prevalence of delayed childbearing and overweight
are increasing in most developed countries.
29
Thus, the relative i m p o r t a n c e of these factors is
likely to increase.
References
1. Kalter H: Five-decade international trends in the relation of perinatal mortality and congenital malformations: Stillbirth and neonatal death compared. IntJ Epidemiol 20:173-179, 1991
2. KleinmanJC, Pierre MBJr., MadansJH, et al: The effects
of maternal smoking on fetal and infant mortality. AmJ
Epidemiol 127:274-282, 1988
3. Cnattingias S, Haglund B, Kramer MS: Differences in
late fetal death rates in association with determinants of
small for gestational age fetuses: Population based cohort study. BMJ 316:1483-1487, 1998
4. Naeye RL: Maternal age, obstetric complications, and
the outcome of pregnancy. Obstet Gynecol 61:210-216,
1983
5. Fretts RC, Usher RH: Causes of fetal death in women of
advanced maternal age. Obstet Gynecol 89:40-45, 1997
6. Lammer EJ, Brown LE, Anderka MT, et al: Classification
and analysis of fetal deaths in Massachusetts. JAMA 261:
1757-1762, 1989
7. Copper RL, Goldenberg RL, DuBard MB, et al: Risk
factors for fetal death in white, black, and Hispanic
women. Collaborative Group on Preterm Birth Prevention. Obstet Gynecol 84:490-495, 1994
8. Gardosi J, Mul T, Mongelli M, et al: Analysis of birthweight and gestational age in antepartum stillbirths. BrJ
Obstet Gynaecol 105:524-530, 1998
9. Stephansson O, Dickman PW, Johansson ALV, et al: The
influence of socioeconomic status on risk of stillbirth in
Sweden. I n t J Epidemiol 2001
10. Yudkin PL, Wood L, Redman CW: Risk of unexplained
stillbirth at different gestational ages. Lancet 1:11921194, 1987
11. Huang DY, Usher RH, Kramer MS, et al: Determinants
of unexplained antepartum fetal deaths. Obstet Gynecol
95:215-221, 2000
12. Raymond EG, Cnattingius S, KielyJL: Effects of maternal
age, parity, and smoking on the risk of stillbirth. Br J
Obstet Gynaecol 101:301-306, 1994
13. Clausson B, Cnattingius S, Axelsson O: Outcomes of
post-term births: the role of fetal growth restriction and
malformations. Obstet Gynecol 94:758-762, 1999
14. Heck KE, Schoendorf KC, Ventura SJ, et al: Delayed
childbearing by education level in the United States,
1969-1994. Matern Child HealthJ 1:81-88, 1997
15. Cnattingius S, Forman MR, Berendes HW, et al: Delayed
childbearing and risk of adverse perinatal outcome. A
population-based study. JAMA 268:886-890, 1992
16. Fretts RC, Schmittdiel J, McLean FH, et al: Increased
maternal age and the risk of fetal death. N Engl J Med
333:953-957, 1995
17. Olausson PO, Cnattingius S, Haglund B: Teenage pregnancies and risk of late fetal death and infant mortality.
BrJ Obstet Gynaecol 106:116-121, 1999
18. Fraser AM, BrockertJE, Ward RH: Association of young
maternal age with adverse reproductive outcomes.
N EnglJ Med 332:1113-1117, 1995
30
Cnattingius and Stephansson
19. Kiely JL, Paneth N, Susser M: An assessment of the
effects of maternal age and parity in different components of perinatal mortality. Am J Epidemiol 123:444454, 1986
20. Little RE, Weinberg CR: Risk factors for antepartum and
intrapartum stillbirth. Am J Epidemiol 137:1177-1189,
1993
21. Ahlsten G, Ewald U, Tuvemo T: Maternal smoking reduces prostacyclin formation in human umbilical arteries. A study on strictly selected pregnancies. Acta Obstet
Gynecol Seand 65:645-649, 1986
22. Longo LD: Carbon monoxide: Effects on oxygenation of
the fetus in utero. Science 194:523-525, 1976
23. Morrow RJ, Ritchie JW, Bull SB: Maternal cigarette
smoking: The effects on umbilical and uterine blood
flow velocity. A m J Obstet Gynecol 159:1069-1071, 1988
24. Kramer MS: Intrauterine growth and gestational duration determinants. Pediatrics 80:502-511, 1987
25. Kramer MS, Usher RH, Pollack R, et al: Etiologic determinants of abruptio placentae. Obstet Gynecol 89:221226, 1997
26. Naeye RL: Abruptio placentae and placenta previa: Frequency, perinatal mortality, and cigarette smoking. Ob,stet G}naecol 55:701-704, 1980
27. Meyer MB, Tonascia JA: Maternal smoking, pregnancy
complications, and perinatal mortality. Am J Obstet Gynecol 128:494-502, 1977
28. Wisborg K, Kesmodel U, Henriksen TB, et al: Exposure
to tobacco smoke in utero and the risk of stillbirth and
death in the first year of life. Am J Epidemiol 154:322327, 2001
29. Cigarette smoking among pregnant women and gMs. In:
Women and smoking--a report from the Surgeon General Rockville, MD, Department of Health and Human
Services, 2001, pp 71-73
30. Cnattingius S, Bergstrom R, Lipworth L, et ah Prepregnancy weight and the risk of adverse pregnancy outcomes. N EnglJ Med 338:147-152, 1998
31. Stephansson O, Dickman PW, Johansson A, et al: Maternal weight, pregnancy weight gain, and the risk of antepartum stillbirth. Am J Obstet Gynecol 184:463-469,
2001
32. Flegal KM, Carroll MD, Kuczmarski RJ, et al: Overweight
33.
34.
35.
36.
37.
38.
39.
40.
41.
42.
43.
44.
45.
46.
and obesity in the United States: prevalence and trends,
1960-1994. IntJ Obes Relat Metab Disord 22:39-47, 1998
Galtier-Dereure F, Boegner C, Bringer J: Obesity and
pregnancy: Complications and cost. Am J Clin Nutr
71:1242S-1248S, 2000
Abrams B, Carmichael S, Selvin S: Factors associated
with the pattern of maternal weight gain during pregnancy. Obstet Gynecol 86:170-176, 1995
Taffel SM: Maternal weight gain and the outcome of
pregnancy. Vital Health Star 21:1-25, 1986
Rydhstrom H, Tyden T, Herbst A, et al: No relation
between maternal weight gain and stillbirth. Acta Obstet
Gynecol Scand 73:779-781, 1994
Cnattingius S, Berendes HW, Forman MR: Do delayed
childbearers face increased risks of adverse pregnancy
outcomes after the first birth? Obstet Gynecol 81:512516, 1993
Samueloff A, Xenakis EM, Berkus MD, et al: Recurrent
stillbirth. Significance and characteristics. J Reprod Med
38:883-886, 1993
Freeman RK, Dorchester W, Anderson G, et al: The
significance of a previous stillbirth. AmJ Obstet Gynecol
151:7-13, 1985
MurphyJF, O'Riordan J, Newcombe RG, et al: Relation
of haemoglobin levels in first and second trimesters to
outcome of pregnancy. Lancet 1:992-995, 1986
Naeye RL: Placental infarction leading to fetal or neonatal death. A prospective study. Obstet Gynecol 50:583588, 1977
Garn SM, Ridella SA, Petzold AS, et ah Maternal hematologic levels and pregnancy outcomes. Semin Perinatol
5:155-162, 1981
Stephansson O, Dickman PW, Johansson A, et al: Maternal hemoglobin concentration during pregnancy and
risk of stillbirth. JAMA 284:2611-2617, 2000
Pharoah PO, Adi Y: Consequences of in-utero death in a
twin pregnancy. Lancet 355:1597-1602, 2000
West CR, Adi Y, Pharoah PO: Fetal and infant death in
mono- and dizygotic twins in England and Wales 198291. Arch Dis Child Fetal Neonatal Ed 80:F217-F220, 1999
Ventura SJ, MartinJA, Curtin SC, et ah Births: final data
for 1998. Natl Vital Stat Rep 48:1-100, 2000
You might also like
- Association Between MRNA Expression of Aromatase 1Document8 pagesAssociation Between MRNA Expression of Aromatase 1Nenny Yoanitha DjalaNo ratings yet
- Palliative Care - Modul NennyDocument31 pagesPalliative Care - Modul NennyNenny Yoanitha DjalaNo ratings yet
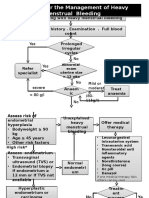
- Algorithm For The Management of Heavy Menstrual BleedingDocument2 pagesAlgorithm For The Management of Heavy Menstrual BleedingNenny Yoanitha DjalaNo ratings yet
- En Endometrial Cancer Guide For PatientsDocument30 pagesEn Endometrial Cancer Guide For PatientsNenny Yoanitha DjalaNo ratings yet
- Hypertensionin PregnancyDocument100 pagesHypertensionin Pregnancyricky hutagalungNo ratings yet
- Estimated Fetal Weight Formula GuideDocument5 pagesEstimated Fetal Weight Formula GuideNenny Yoanitha Djala100% (1)
- Night Shift Duty 11 FEBRUARIDocument2 pagesNight Shift Duty 11 FEBRUARINenny Yoanitha DjalaNo ratings yet
- AJOG 2008 - Amoxicillin Pharmacokinetics in Pregnant WomenDocument6 pagesAJOG 2008 - Amoxicillin Pharmacokinetics in Pregnant WomenNenny Yoanitha DjalaNo ratings yet
- Program Kerja Gugus Kendali Mutu SMF Obstetri dan Ginekologi 2017-2018Document1 pageProgram Kerja Gugus Kendali Mutu SMF Obstetri dan Ginekologi 2017-2018Nenny Yoanitha DjalaNo ratings yet
- Reichman 2014Document5 pagesReichman 2014Nenny Yoanitha DjalaNo ratings yet
- Algorithm For The Management of Heavy Menstrual BleedingDocument2 pagesAlgorithm For The Management of Heavy Menstrual BleedingNenny Yoanitha DjalaNo ratings yet
- American Journal of Obstetrics and Gynecology Volume 207 Issue 3 2012 (Doi 10.1016/j.ajog.2012.07.031) McPherson, Jessica A. Odibo, Anthony O. Shanks, Anthony L. Ro - Impact of Chorionicity On R PDFDocument6 pagesAmerican Journal of Obstetrics and Gynecology Volume 207 Issue 3 2012 (Doi 10.1016/j.ajog.2012.07.031) McPherson, Jessica A. Odibo, Anthony O. Shanks, Anthony L. Ro - Impact of Chorionicity On R PDFNenny Yoanitha DjalaNo ratings yet
- Forceps Review in Modern Obstetric PracticeDocument5 pagesForceps Review in Modern Obstetric PracticeNenny Yoanitha DjalaNo ratings yet
- Strategi Bisnis KorporasiDocument41 pagesStrategi Bisnis KorporasiAliMu'minHarahapNo ratings yet
- Termination Pregnancy Report 18 May 2010Document45 pagesTermination Pregnancy Report 18 May 2010Nenny Yoanitha DjalaNo ratings yet
- Obstetrical Forceps - History Mystery and MoralityDocument16 pagesObstetrical Forceps - History Mystery and MoralityNenny Yoanitha DjalaNo ratings yet
- Medical Eligibility Criteria For Contraceptive Use Fifth Edition 2015Document14 pagesMedical Eligibility Criteria For Contraceptive Use Fifth Edition 2015agustinasntNo ratings yet
- How To Explore After Forceps ExtractionDocument7 pagesHow To Explore After Forceps ExtractionNenny Yoanitha DjalaNo ratings yet
- Anatomical Causes Bad Obstetric HistoryDocument3 pagesAnatomical Causes Bad Obstetric Historykyle31No ratings yet
- Fetal and Maternal Effects of Forceps and VacuumDocument4 pagesFetal and Maternal Effects of Forceps and VacuumNenny Yoanitha DjalaNo ratings yet
- Final Data 2011 PDFDocument90 pagesFinal Data 2011 PDFNenny Yoanitha DjalaNo ratings yet
- Reichman 2014Document5 pagesReichman 2014Nenny Yoanitha DjalaNo ratings yet
- Trali Dari Ats JournalDocument2 pagesTrali Dari Ats JournalNenny Yoanitha DjalaNo ratings yet
- Algorithm For The Management of Heavy Menstrual BleedingDocument2 pagesAlgorithm For The Management of Heavy Menstrual BleedingNenny Yoanitha DjalaNo ratings yet
- Cytomegalovirus Infection in Patients With Active InflammatoryDocument7 pagesCytomegalovirus Infection in Patients With Active InflammatoryNenny Yoanitha DjalaNo ratings yet
- Forceps ExtractionDocument49 pagesForceps ExtractionNenny Yoanitha DjalaNo ratings yet
- Genetic Study of TORCH Infections in Women With BOH PDFDocument6 pagesGenetic Study of TORCH Infections in Women With BOH PDFNenny Yoanitha DjalaNo ratings yet
- Reichman 2014Document5 pagesReichman 2014Nenny Yoanitha DjalaNo ratings yet
- Successful Pregnancy OutcomeDocument6 pagesSuccessful Pregnancy OutcomeNenny Yoanitha DjalaNo ratings yet
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5784)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (890)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (72)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- 3rd Annual Radiology For Non-Radiologists (5-6 Oct 2019)Document2 pages3rd Annual Radiology For Non-Radiologists (5-6 Oct 2019)itnnetworkNo ratings yet
- General Pathology MCQDocument3 pagesGeneral Pathology MCQSooPl33% (3)
- Cephalometric Evaluation of GrowthDocument79 pagesCephalometric Evaluation of GrowthAhmedsy Ahmedsy AhmedsyNo ratings yet
- Surgical Specimen Management: A Descriptive Study of 648 Adverse Events and Near MissesDocument7 pagesSurgical Specimen Management: A Descriptive Study of 648 Adverse Events and Near MissesRubia Sari Mamanya HaristNo ratings yet
- Velammal VistDocument30 pagesVelammal VistpriyaNo ratings yet
- Notification Babu Jagjivan Ram Memorial Hospital SR Resident PostsDocument5 pagesNotification Babu Jagjivan Ram Memorial Hospital SR Resident PostsJeshiNo ratings yet
- 04.03-02 Endocrine IV - Uterine Pharmacology PDFDocument4 pages04.03-02 Endocrine IV - Uterine Pharmacology PDFMaikka IlaganNo ratings yet
- Gestational AgeDocument4 pagesGestational AgeNadya Nur AqilahNo ratings yet
- Placenta Previa MarginalDocument50 pagesPlacenta Previa MarginalMedy WedhanggaNo ratings yet
- Vandykediann ResumeDocument3 pagesVandykediann ResumeHARSHANo ratings yet
- BibliographyDocument21 pagesBibliographyapi-204960846No ratings yet
- Kangaroo Joey ManualDocument16 pagesKangaroo Joey ManualCarmen Leiva AsencioNo ratings yet
- Factors Affecting Utilization of Maternal Health CDocument8 pagesFactors Affecting Utilization of Maternal Health CYussufNo ratings yet
- Case presentation on short stature and pubertal delay in a 14-year-old maleDocument27 pagesCase presentation on short stature and pubertal delay in a 14-year-old maledidu91No ratings yet
- Live Before You DieDocument6 pagesLive Before You DieCharms CabauatanNo ratings yet
- Third Stage of Labour Lastt Last LastDocument30 pagesThird Stage of Labour Lastt Last LastAyanayuNo ratings yet
- CV Elective Program For International StudentsDocument5 pagesCV Elective Program For International StudentsYosafatPrasetyadiNo ratings yet
- ISICAM TimetableDocument8 pagesISICAM TimetableMichael SusantoNo ratings yet
- 2018 UNICEF Eswatini Neonatal GuidelinesDocument180 pages2018 UNICEF Eswatini Neonatal GuidelinesTrishenth FonsekaNo ratings yet
- Smart Solutions For OB/GYN: ACUSON X Family and ACUSON P Family Ultrasound SystemsDocument8 pagesSmart Solutions For OB/GYN: ACUSON X Family and ACUSON P Family Ultrasound SystemsPopescu ValiNo ratings yet
- Maquet LyraDocument12 pagesMaquet LyraMiguel YepesNo ratings yet
- Botiss Maxgraft Bonebuilder SurgicalGuideDocument11 pagesBotiss Maxgraft Bonebuilder SurgicalGuideDemmy WijayaNo ratings yet
- Periodontal FlapsDocument65 pagesPeriodontal FlapsSaleh AlsadiNo ratings yet
- KAREEN PRC FILE Corrected FinalDocument10 pagesKAREEN PRC FILE Corrected Finaljedkath2008No ratings yet
- Traumatic Diaphragmatic Hernia Anaesthetic ConsideDocument3 pagesTraumatic Diaphragmatic Hernia Anaesthetic ConsideHalim SudonoNo ratings yet
- Mccee QuestionsDocument69 pagesMccee QuestionsAndre R. Reynolds Anglin100% (3)
- Transcutaneous Electrical Nerve Stimulation (Tens) and Pain ManagementDocument54 pagesTranscutaneous Electrical Nerve Stimulation (Tens) and Pain ManagementhashfiluthfihNo ratings yet
- 2017.104 - The - Leopold - Maneuver - PosterDocument1 page2017.104 - The - Leopold - Maneuver - PosterRey CelNo ratings yet
- Facial ContoursDocument20 pagesFacial Contourscmkflorida7011100% (1)
- Plan of The Course Anatomy and Clinical Anatomy: Academic Year 2013/2014Document7 pagesPlan of The Course Anatomy and Clinical Anatomy: Academic Year 2013/2014Rinor MujajNo ratings yet