Professional Documents
Culture Documents
NSAID Colopathy Case Series
Uploaded by
Sundar RamanathanCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
NSAID Colopathy Case Series
Uploaded by
Sundar RamanathanCopyright:
Available Formats
NSAID-induced Colopathy.
A Case Series
Abdur R Aftab, Fergal Donnellan, Faisal Zeb, David Kevans, Garret Cullen, Garry Courtney
St. Lukes Hospital, Kilkenny, Ireland
Abstract
The adverse effects of non-steroidal anti-inflammatory
drugs (NSAIDs) on the upper gastrointestinal tract and small
intestine are well established. The effect of such therapy on
the large intestine, so called NSAID colopathy, is less well
described. We present four such cases demonstrating the
characteristic endoscopic findings. One case in particular is,
to our knowledge, the first report of the natural history of
this clinical entity, initially presenting with the acute picture
of inflammation and ulceration with subsequent progression
to the more chronic development of diaphragm-like fibrous
strictures. NSAID-induced colonic damage is a clinically
significant condition. Two of our patients presented with
bloody diarrhoea while the other two patients developed
symptomatic anaemia. With the increasing use of enteric
coated and sustained release NSAID preparations this
condition is likely to become more frequent. Increasing
awareness of its clinical presentation and of its spectrum of
endoscopic findings facilitates a more prompt diagnosis and
appropriate treatment to be established.
albeit less well recognized than NSAID-induced gastropathy
and enteropathy. Isolated case reports of NSAID colopathy
range from the more acute complication of inflammation
and ulceration to the more chronic picture of fibrosis and
stricture formation.
Case 1
The first case involves a 65 year old woman who
presented with a year long history of bloody diarrhoea
with intermittent nausea and vomiting and iron deficiency
Key words
NSAID colopathy anemia lower digestive
hemorrhage colon stricture.
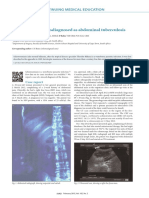
Fig 1. Finding at colonoscopy showing right sided
patchy inflammation.
Introduction
Debenham described the first case of NSAID-induced
colonic damage in 1966, highlighting a case of caecal
ulceration in a patient taking oxyphenbutazone for
rheumatoid arthritis [1]. Since then, the association between
NSAIDs and colonic damage has become well established,
Received:16.02.2009 Accepted: 26.02.2009
J Gastrointestin Liver Dis
March 2010 Vol.19 No 1, 89-91
Address for correspondence:
Dr. AR Aftab
Department of Gastroenterology
St. Lukes Hospital
Kilkenny, Ireland
E-mail: aftabar@hotmail.com
Fig 2. Relatively normal colonic mucosa with
adjacent area of ulceration with acute colitis and
glandular distortion. There are no granulomas,
epithelial dysplasia or malignancy (H-E x 40).
90
Aftab et al
anaemia with a haemoglobin of 9.8g/dL (12 - 15.0g/dL) and
a mean corpuscular volume of 68 (83 -100). Her past medical
history was significant for seronegative arthritis for which
she was taking diclofenac 75mg twice daily for one year prior
to presentation. Upper gastrointestinal endoscopy showed
Helicobacter pylori negative antral gastritis. Small bowel
biopsies were normal. A colonoscopy showed moderate
patchy inflammation from the sigmoid colon to the caecum
(Fig. 1). Subsequent biopsies revealed mild cryptitis in the
ascending and descending colon. There was no evidence of
goblet cell depletion, crypt abscess formation, granulomata
or malignancy (Fig. 2). The terminal ileum was normal at
endoscopy and subsequent biopsies were unremarkable. The
patient was treated for an acute exacerbation of inflammatory
bowel disease and her symptoms settled initially on
intravenous and subsequently oral steroids. Of note, the
patient remained on diclofenac therapy. However, seven
months later, while on 5mg prednisolone, she presented
again with diarrhoea and a haemoglobin of 5.5g/dl. A second
gastroscopy was unremarkable and repeat colonoscopy
subsequently settled. A third colonoscopy performed one
year after the initial presentation showed a number of fibrous
diaphragms situated in the right colon. There was not any
associated inflammation and again the biopsies were normal
Fig. 4). The patient has remained symptom-free with normal
haemoglobin 18 months after her last colonoscopy.
Case 2
The second case involves a 63 year old woman who
presented with iron deficiency anaemia. Her haemoglobin
measured 4.1g/dL and mean corpuscular volume was 64.
She had noticed increasing dyspnoea and fatigue over the
preceding three months. She did not have any gastrointestinal
symptoms. Her past medical history was significant for
osteoarthritis for which she was taking diclofenac 50mg
daily for two years prior to presentation. Gastroscopy
was unremarkable apart from a mild Helicobacter pylori
negative antral gastritis. Biopsies from the proximal small
bowel were negative for coeliac disease. Subsequent
colonoscopy was performed to the terminal ileum. While
patchy inflammation was evident throughout the colon, the
most predominant feature was six fibrous diaphragms in the
right colon. The terminal ileum was normal. Subsequent
biopsies from the fibrous diaphragms were unremarkable.
Eighteen months later, off diclofenac, she remains well with
normal haemoglobin.
Case 3
Fig 3. Finding at 2 nd colonoscopy of rightsided diaphragm-like stricture with associated
inflammation.
Fig 4. Finding at 3rd colonoscopy of right-sided
diaphragm without any associated inflammation.
revealed multiple diaphragm-like strictures associated with
patchy inflammation from the splenic flexure to caecum (Fig.
3). Interestingly serial colonic biopsies were unremarkable.
It was felt at this stage that the clinical picture was more in
keeping with NSAID-induced colonic damage rather than
inflammatory bowel disease.
The likely offending agent was stopped. She did
not receive any further steroid therapy. The diarrhoea
The third case was a 57 year old woman with iron
deficiency anaemia. Her haemoglobin was 7.4g/dL with a
mean corpuscular volume of 76. She suffered from Stills
disease for which she had been taking diclofenac 75mg twice
daily for two months prior to admission and prednisolone
5mg daily. Her past medical history also included
hypertension. The patient did not have any gastrointestinal
symptoms. Upper endoscopy was performed showing mild
Helicobacter pylori negative antral gastritis. A colonoscopy
was also carried out. This demonstrated two separate areas
of inflamed ulcerated mucosa with early stricture formation
in the right colon. In addition there was mild inflammation
present in the left colon. While both malignancy and Crohns
disease were considered in the differential diagnosis, it was
felt that the overall picture was more consistent with NSAIDinduced colopathy. Subsequent biopsies from the right colon
revealed densely inflamed granulation tissue consistent with
ulceration. There was no evidence of active colitis, dysplasia
or malignancy. The patients diclofenac medication has since
been stopped and twelve months later she remains well with
normal haemoglobin.
Case 4
A 61 year old woman was referred by her G.P. with four
months history of intermittent bloody diarrhoea and anaemia.
Her haemoglobin was 7.2 g/dL with mean corpuscular
volume of 72. She had a background history of rheumatoid
NSAID-induced colopathy
Fig 5. Inflamed diaphragm in ascending colon seen
at colonoscopy (Case 4).
arthritis, hypertension, osteoporosis, fibromyalgia and
depression. She had been taking diclofenac 75 mg
twice daily for five years, prednisolone 5 mg daily and
methotrexate for R.A. and fosmax for osteoporosis. As part
of the investigation for bloody diarrhoea a colonoscopy was
performed which showed several inflammatory diaphragms
from the transverse colon to caecum (Fig. 5). The terminal
ileum appeared normal. Biopsies were taken from ascending
and transverse colon diaphragms which showed ulceration
with a formation of sub acute fibro-vascular granulation
tissue. There was no evidence of granulomata, cryptitis or
dysplasia. Random left colonic biopsies were normal. The
diclofenac has since been stopped and six months later the
patient remains well.
Discussion
We would like to highlight our case series for a number
of reasons. Firstly, the endoscopic findings were confined
predominantly to the right colon. This is in keeping with
previous reports supporting the theory that this condition
occurs as a result of direct drug toxicity. The increasing use
of both slow release and enteric coated preparations allow
more of the medication to reach the right colon with the
caecum acting as a reservoir [2, 3].
NSAID-induced colonic damage is clinically significant
and not just a benign endoscopic finding. The four patients
presented with symptoms ranging from debilitating
bloody diarrhoea to symptomatic anaemia requiring blood
transfusion. Reports in the literature also indicate that the
NSAID-induced fibrous diaphragms can lead to significant
stenoses necessitating balloon dilatation and often segmental
colectomy [4, 5].
Our series highlights that this effect of NSAIDs is not
likely to be dose related. Our patients were taking doses
between 50 mg to 150mg daily. However the duration of
treatment is highly significant demonstrating a temporal
91
relationship between drug administration and the spectrum
of endoscopic features found in NSAID colopathy.
The patient described in Case 3 was on treatment for two
months and showed evidence only of colonic inflammation
and ulceration that at endoscopy could be mistaken for
Crohns disease or colonic malignancy. The patients described
in Cases 1, 2 and 4 were on treatment with diclofenac for
a number of years and consequently demonstrated the
more pathognomonic feature of diaphragm-like colonic
strictures [6, 7]. To our knowledge the natural history of
NSAID colopathy has not been described. Interestingly, the
patient described in Case 1 had a series of colonoscopies
which demonstrated endoscopic evidence of progression
of this condition. Inflammation was evident at the initial
colonoscopy one year into treatment with diclofenac. This
progressed over the next seven months to early diaphragm
formation associated with the initial inflammatory changes.
The patient had remained on NSAID treatment during this
time. Cessation of the drug resulted in resolution of the
inflammation. However, the diaphragms already formed,
persisted.
Increasing awareness of this clinical phenomenon of
NSAID-induced colopathy allows a prompt endoscopic
diagnosis to be made instead of other differential diagnoses
such as inflammatory bowel disease or colon cancer. This
would lead to the appropriate management and cessation of
the offending agent, thereby avoiding potential toxic effects
of other treatments.
Conflicts of interest
None to declare.
References
1. Debenham GP. Ulcer of the cecum during oxyphenbutazone
(tandearil) therapy. Can Med Assoc J 1966 28; 94:1182-1184
2. Byrne MF, McGuinness J, Smyth CM, et al. Nonsteroidal antiinflammatory drug-induced diaphragms and ulceration in the colon.
Eur J Gastroenterol Hepatol 2002;14: 1265-1269.
3. Aloysius MM, Kaye PV, Lobo DN. Non-steroidal anti-inflammatory
drug (NSAID)-induced colonic strictures and perforation: a case
report. Dig Liver Dis 2006; 38: 276-278.
4. Gopal DV, Katon RM. Endoscopic balloon dilation of multiple
NSAID-induced colonic strictures: case report and review of
literature on NSAID-related colopathy. Gastrointest Endosc 1999;
50: 120-123.
5. Smith JA, Pineau BC. Endoscopic therapy of NSAID-induced colonic
diaphragm disease: two cases and a review of published reports.
Gastrointest Endosc 2000; 52: 120-125.
6. Huber T, Ruchti C, Halter F. Nonsteroidal antiinflammatory
drug-induced colonic strictures: a case report. Gastroenterology
1991;100:1119-1122.
7. Israel LH, Koea JB, Stewart ID, Wright CL, Frankish PD.
Nonsteroidal anti-inflammatory drug-induced strictures of the colon:
report of a case and review of the literature. Dis Colon Rectum 2001;
44:1362-1364.
You might also like
- A Girl With Ulcerative Colitis in A Tertiary Care Hospital-A Case ReportDocument4 pagesA Girl With Ulcerative Colitis in A Tertiary Care Hospital-A Case ReportAbdullah KhanNo ratings yet
- A Girl With Ulcerative Colitis in A Tertiary Care Hospital-A Case ReportDocument4 pagesA Girl With Ulcerative Colitis in A Tertiary Care Hospital-A Case ReportWyn AgustinNo ratings yet
- en Hematochezia in Young Patient Due To CroDocument3 pagesen Hematochezia in Young Patient Due To Croseptian_tjayaNo ratings yet
- Life-Threatening Lower Gastrointestinal Hemorrhage in Pediatric Crohn's DiseaseDocument8 pagesLife-Threatening Lower Gastrointestinal Hemorrhage in Pediatric Crohn's DiseasePeregrine Albertus Ricco AzaliNo ratings yet
- MedicineDocument5 pagesMedicineRoyd Jesse Kwibisa JrNo ratings yet
- NSAID Colon UlcersDocument5 pagesNSAID Colon UlcersFrederic IkkiNo ratings yet
- Endoscopia: Diagnostic Approach of Intestinal Tuberculosis: Case and Literature ReviewDocument4 pagesEndoscopia: Diagnostic Approach of Intestinal Tuberculosis: Case and Literature ReviewDumitru RadulescuNo ratings yet
- Al12 1 JuvenileDocument24 pagesAl12 1 JuvenileDiego Alberto Hernández CatalánNo ratings yet
- IBD-Rough Road - Case Study in IBD From Presentation To ManagementDocument4 pagesIBD-Rough Road - Case Study in IBD From Presentation To ManagementBejan CorinaNo ratings yet
- Pathologic Quiz Case: Residents' PageDocument4 pagesPathologic Quiz Case: Residents' Pagejeka222No ratings yet
- Crohn's Disease and Recurrent Appendicitis A Case ReportDocument3 pagesCrohn's Disease and Recurrent Appendicitis A Case ReportazizijogjaNo ratings yet
- EMQs For Medical Students Volume 2 2eDocument30 pagesEMQs For Medical Students Volume 2 2ePasTestBooks50% (2)
- Abdominal TB Causing Intestinal ObstructionDocument10 pagesAbdominal TB Causing Intestinal ObstructionCleoanne GallegosNo ratings yet
- USG Splenic AbscessDocument2 pagesUSG Splenic AbscessTaufik ShidkiNo ratings yet
- Awuku 1552016 BJMMR26166Document4 pagesAwuku 1552016 BJMMR26166Kush GuptaNo ratings yet
- Intestinal Tuberculosis: A Diagnostic Challenge: Open Access Case DOI: 10.7759/cureus.13058Document4 pagesIntestinal Tuberculosis: A Diagnostic Challenge: Open Access Case DOI: 10.7759/cureus.13058ATIKA INDAH SARINo ratings yet
- Clinical Practice AssignmentDocument17 pagesClinical Practice Assignmentapi-581678058No ratings yet
- ASN 11 Handout Case Study PDFDocument4 pagesASN 11 Handout Case Study PDFania ojedaNo ratings yet
- Teaching Case of The Month: Abdominal Tuberculosis: An Unusual Cause of Abdominal PainDocument4 pagesTeaching Case of The Month: Abdominal Tuberculosis: An Unusual Cause of Abdominal PainkingkinresmytaNo ratings yet
- Nonsteroidal Anti-Inflammatory Drug-Induced Colopathy An Uncommon Cause of Positive Immunochemical Faecal Occult Blood Test in The Program For Colorectal Cancer ScreeningDocument4 pagesNonsteroidal Anti-Inflammatory Drug-Induced Colopathy An Uncommon Cause of Positive Immunochemical Faecal Occult Blood Test in The Program For Colorectal Cancer ScreeningKito TongHuiNo ratings yet
- 4 - Clinical Patterns in Crohn's Disease - A Statistical Study of 615 CasesDocument9 pages4 - Clinical Patterns in Crohn's Disease - A Statistical Study of 615 CasesVân NguyễnNo ratings yet
- Pi Is 0016508500545053Document5 pagesPi Is 0016508500545053Abdullah KhanNo ratings yet
- Pi Is 0016508500545053Document5 pagesPi Is 0016508500545053Abdullah KhanNo ratings yet
- Optimal Management of Collagenous Colitis A Review 021016Document9 pagesOptimal Management of Collagenous Colitis A Review 021016Eliza DNNo ratings yet
- Development of Type I Gastric Carcinoid in Patients With Chronic Atrophic GastritisDocument9 pagesDevelopment of Type I Gastric Carcinoid in Patients With Chronic Atrophic GastritisAbristaSeptikasariNo ratings yet
- Hiding in The Water: Clinical Problem-SolvingDocument6 pagesHiding in The Water: Clinical Problem-SolvingtabareeNo ratings yet
- Jejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of LiteratureDocument6 pagesJejunojejunal Intussusception As Initial Presentation of Coeliac Disease: A Case Report and Review of Literatureellya theresiaNo ratings yet
- Iihyuyu6756e54tw5w3553w5et6yfug5757 Jgut75Document6 pagesIihyuyu6756e54tw5w3553w5et6yfug5757 Jgut75RIBNo ratings yet
- Acute Appendicitis in A Patient With Systemic Lupus ErythematosusDocument4 pagesAcute Appendicitis in A Patient With Systemic Lupus ErythematosusJessicaNo ratings yet
- Colonoscopy Induced Ischemic Colitis: An Endoscopic and Histological AssayDocument3 pagesColonoscopy Induced Ischemic Colitis: An Endoscopic and Histological AssayArfania LailyNo ratings yet
- Case Report Peritonitis WordDocument4 pagesCase Report Peritonitis WordMufidatul UmmahNo ratings yet
- JGH 13992Document1 pageJGH 13992Dolly JazmiNo ratings yet
- 18-01 - Going From A To ZDocument7 pages18-01 - Going From A To ZKodoNo ratings yet
- Acute Jejunoileal Obstruction Due To A Pseudopolyp in A Child With Undiagnosed Crohn S DiseaseDocument4 pagesAcute Jejunoileal Obstruction Due To A Pseudopolyp in A Child With Undiagnosed Crohn S Diseasebingl_073No ratings yet
- Penyakit Crohn: Laporan Kasus: Paul V. Siwy, Fandy GosalDocument10 pagesPenyakit Crohn: Laporan Kasus: Paul V. Siwy, Fandy GosalyheyenNo ratings yet
- Granulomatous Appendicitis in A 12-Year-Old Boy: Derya Yayla, Bedriye Nuray Alpman, Yasemin DolekDocument3 pagesGranulomatous Appendicitis in A 12-Year-Old Boy: Derya Yayla, Bedriye Nuray Alpman, Yasemin Dolekansar ahmedNo ratings yet
- Clinical Review: Management of DiverticulitisDocument5 pagesClinical Review: Management of DiverticulitispsychobillNo ratings yet
- J Epsc 2015 05 012Document4 pagesJ Epsc 2015 05 012Hanung PujanggaNo ratings yet
- Case Report: Tuberculosis Liver Abscess in Alcoholism Male PatientDocument4 pagesCase Report: Tuberculosis Liver Abscess in Alcoholism Male PatientWidya Prawirani SiahaanNo ratings yet
- 1471 230X 12 174 PDFDocument5 pages1471 230X 12 174 PDFAila HinlogNo ratings yet
- Empyema Gall Bladder - Forgotten or An Under-ReporDocument4 pagesEmpyema Gall Bladder - Forgotten or An Under-ReporalamgirjalilpramanikNo ratings yet
- EMQsDocument30 pagesEMQsnob2011nob100% (1)
- Acute Cholangitis in A Patient With Kluyvera Cryocrescens Bacteremia: A Case Report and Literature ReviewDocument4 pagesAcute Cholangitis in A Patient With Kluyvera Cryocrescens Bacteremia: A Case Report and Literature ReviewDhen Mas PrimanaNo ratings yet
- Balloon and Bougie Dilation of Benign Esophageal Strictures: Ajay George, Vikas SinhaDocument3 pagesBalloon and Bougie Dilation of Benign Esophageal Strictures: Ajay George, Vikas SinhaAgus KarsetiyonoNo ratings yet
- Ajol File Journals - 76 - Articles - 114038 - Submission - Proof - 114038 901 318286 1 10 20150309Document2 pagesAjol File Journals - 76 - Articles - 114038 - Submission - Proof - 114038 901 318286 1 10 20150309alysNo ratings yet
- Diver TicularDocument5 pagesDiver TicularVi GossNo ratings yet
- Indeterminate ColitisDocument26 pagesIndeterminate ColitisMarlisa YanuartiNo ratings yet
- Case Report: Streptococcus AnginosusDocument4 pagesCase Report: Streptococcus AnginosusIesanu MaraNo ratings yet
- Dor Abdominal e FalcidromeDocument7 pagesDor Abdominal e FalcidromeVinicius SpazzapanNo ratings yet
- Oxigen Oter A PijaDocument6 pagesOxigen Oter A PijazixdiddyNo ratings yet
- Poliadenitis NodosaDocument5 pagesPoliadenitis NodosaRicardo Uzcategui ArreguiNo ratings yet
- Gastrointestinal Pathology Case Studies ParDocument2 pagesGastrointestinal Pathology Case Studies Pardr nirupamaNo ratings yet
- Gill 2011Document4 pagesGill 2011qwerNo ratings yet
- Coeliac Disease: John S. Leeds, Andrew D. Hopper, and David S. SandersDocument14 pagesCoeliac Disease: John S. Leeds, Andrew D. Hopper, and David S. Sandersbdalcin5512No ratings yet
- 2019 Article 1205Document6 pages2019 Article 1205zahra h f aNo ratings yet
- Clinical Predictors of Ileocecal Tuberculosis: A Case SeriesDocument14 pagesClinical Predictors of Ileocecal Tuberculosis: A Case SeriesChristopher AsisNo ratings yet
- Images For Surgeons: Abdominal Tuberculosis: An Easily Forgotten DiagnosisDocument2 pagesImages For Surgeons: Abdominal Tuberculosis: An Easily Forgotten DiagnosisRisti Khafidah100% (1)
- Colitis PDFDocument11 pagesColitis PDFicoanamareNo ratings yet
- GERD: A New Understanding of Pathology, Pathophysiology, and TreatmentFrom EverandGERD: A New Understanding of Pathology, Pathophysiology, and TreatmentNo ratings yet
- Colitis: A Practical Approach to Colon and Ileum Biopsy InterpretationFrom EverandColitis: A Practical Approach to Colon and Ileum Biopsy InterpretationAnne Jouret-MourinNo ratings yet
- Rasi Navamsa: Untitled ChartDocument11 pagesRasi Navamsa: Untitled ChartSundar RamanathanNo ratings yet
- A Hands On Approach To Patch TestingDocument11 pagesA Hands On Approach To Patch TestingSundar RamanathanNo ratings yet
- Adult Combined ScheduleDocument13 pagesAdult Combined ScheduleJustin Ng SincoNo ratings yet
- How To Say No 5 Steps To Stop Being A People Pleaser Life Kit NPRDocument7 pagesHow To Say No 5 Steps To Stop Being A People Pleaser Life Kit NPRSundar Ramanathan100% (1)
- Rasi Navamsa: Untitled ChartDocument11 pagesRasi Navamsa: Untitled ChartSundar RamanathanNo ratings yet
- What You Should Know Before Buying A Home Security SystemDocument13 pagesWhat You Should Know Before Buying A Home Security SystemSundar RamanathanNo ratings yet
- Rasi Navamsa: Untitled ChartDocument11 pagesRasi Navamsa: Untitled ChartSundar RamanathanNo ratings yet
- AWS AICamp CertificationDocument39 pagesAWS AICamp CertificationSundar RamanathanNo ratings yet
- Upakarma Devanagari 1Document15 pagesUpakarma Devanagari 1Harish KNNo ratings yet
- 28 AshtakvargaThumbRules PDFDocument11 pages28 AshtakvargaThumbRules PDFAnand AgrawalNo ratings yet
- .. Shri Lalitasahasranama Stotram ..: August 20, 2017Document24 pages.. Shri Lalitasahasranama Stotram ..: August 20, 2017balarrusNo ratings yet
- How To Say No 5 Steps To Stop Being A People Pleaser Life Kit NPRDocument7 pagesHow To Say No 5 Steps To Stop Being A People Pleaser Life Kit NPRSundar Ramanathan100% (1)
- Hemodialysis KineticsDocument26 pagesHemodialysis KineticsSundar RamanathanNo ratings yet
- Best Commuter Towns in NJ To NYC Midtown Direct Homes PDFDocument3 pagesBest Commuter Towns in NJ To NYC Midtown Direct Homes PDFSundar RamanathanNo ratings yet
- Autism Support NJ Excellent Learning CoursesDocument6 pagesAutism Support NJ Excellent Learning CoursesSundar RamanathanNo ratings yet
- Prescription Program: Drug List - To Be Used by Members Who Have A Three (3) Tiered Drug PlanDocument8 pagesPrescription Program: Drug List - To Be Used by Members Who Have A Three (3) Tiered Drug PlanSundar RamanathanNo ratings yet
- Anthem CVS Caremark Value Formulary 072020Document56 pagesAnthem CVS Caremark Value Formulary 072020Sundar RamanathanNo ratings yet
- Game of ThronesDocument34 pagesGame of ThronesSundar RamanathanNo ratings yet
- CRRT Order Set-RenalDocument4 pagesCRRT Order Set-RenalSundar RamanathanNo ratings yet
- VyasapujaiDocument2 pagesVyasapujaiSundar RamanathanNo ratings yet
- Game of ThronesDocument34 pagesGame of ThronesSundar RamanathanNo ratings yet
- Press Release OCI Reissuance 122019Document1 pagePress Release OCI Reissuance 122019Sundar RamanathanNo ratings yet
- Bangalore Property Lawyers FundaDocument15 pagesBangalore Property Lawyers FundaSundar RamanathanNo ratings yet
- Sandhyavandanam ImportanceDocument13 pagesSandhyavandanam ImportanceSundar RamanathanNo ratings yet
- Bringing Parents To Live in The United States As Permanent Residents USCISDocument3 pagesBringing Parents To Live in The United States As Permanent Residents USCISSundar RamanathanNo ratings yet
- 2012 NDT Wetzels Genetic FSGSDocument9 pages2012 NDT Wetzels Genetic FSGSSundar RamanathanNo ratings yet
- Arya ManDocument1 pageArya ManSundar RamanathanNo ratings yet
- AgniDocument6 pagesAgniSundar Ramanathan100% (1)
- VG Equity Income Jan 2018Document54 pagesVG Equity Income Jan 2018Sundar RamanathanNo ratings yet
- 2012 NDT Wetzels Genetic FSGSDocument9 pages2012 NDT Wetzels Genetic FSGSSundar RamanathanNo ratings yet
- Teacher School ME Report S.Y. 2019 2020Document6 pagesTeacher School ME Report S.Y. 2019 2020Rufus TanhuecoNo ratings yet
- Service Manual Anestesia Machine GE9100cDocument241 pagesService Manual Anestesia Machine GE9100cYesid Dayan De Leon Escorcia100% (1)
- Anaphy Instuctural DesignDocument6 pagesAnaphy Instuctural DesignDanielleSarahCacheroNo ratings yet
- Courses - Downloads - 2019 Batch - Dual Degree CurriculumDocument86 pagesCourses - Downloads - 2019 Batch - Dual Degree CurriculumSreejith N ch19b090No ratings yet
- Human Embalming TechniquesDocument5 pagesHuman Embalming TechniquesOlufemi KolawoleNo ratings yet
- Translation and Validation of The Amsterdam Preoperative Anxiety and Information Scale (Apais) Into Hausa LanguageDocument23 pagesTranslation and Validation of The Amsterdam Preoperative Anxiety and Information Scale (Apais) Into Hausa LanguageGlobal Research and Development ServicesNo ratings yet
- Grand Strategy MatrixDocument1 pageGrand Strategy MatrixDominic SociaNo ratings yet
- Daftar Pustaka - 2pusssDocument6 pagesDaftar Pustaka - 2pusssMuhammad ShodiqinNo ratings yet
- NCPDocument11 pagesNCPJohnhineNo ratings yet
- Bartleby and Infantile AutismDocument4 pagesBartleby and Infantile AutismAlyna Marya IoaneiNo ratings yet
- EntomologistDocument4 pagesEntomologistapi-79028662No ratings yet
- Robots in Shipbuilding Industry (1160) PDFDocument9 pagesRobots in Shipbuilding Industry (1160) PDFWahyu WahyurachmatdhaniNo ratings yet
- Topic: Magnesium Sulphate (Mgso4: Group 5Document11 pagesTopic: Magnesium Sulphate (Mgso4: Group 5Wan Ahmad FaizFaizalNo ratings yet
- June 2022 Set 1 Test Paper - Do Not Let Parents DecideDocument11 pagesJune 2022 Set 1 Test Paper - Do Not Let Parents DecideAISYAH ABDULLAHNo ratings yet
- DHCDocument2 pagesDHCLiaqat Ali KhanNo ratings yet
- Food Defense Planning For Wholesale Food Establishments A Self-Inspection ChecklistDocument2 pagesFood Defense Planning For Wholesale Food Establishments A Self-Inspection ChecklistFrancisco0% (1)
- Operant ConditioningDocument18 pagesOperant ConditioningIna GanuNo ratings yet
- Rational-Emotive Behaviour Therapy (Rebt)Document11 pagesRational-Emotive Behaviour Therapy (Rebt)Sheralena Mohd RasidNo ratings yet
- Dast20 PDFDocument3 pagesDast20 PDFMarchnuelNo ratings yet
- Introduction To Water and Sanitation For Health Facility Improvement Tool "Wash Fit"Document73 pagesIntroduction To Water and Sanitation For Health Facility Improvement Tool "Wash Fit"dalford100% (1)
- Fluoride The Aging Factor PDFDocument151 pagesFluoride The Aging Factor PDFkate bastidasNo ratings yet
- Jurnal Hubungsn Stres Dengan Kesehatan Gigi Dan MulutDocument8 pagesJurnal Hubungsn Stres Dengan Kesehatan Gigi Dan MulutTyasNurFauzianaNo ratings yet
- Report - SUMATHI (230380015090)Document5 pagesReport - SUMATHI (230380015090)anumolusumathiNo ratings yet
- Ge Lightspeed 16 Brochure PDFDocument8 pagesGe Lightspeed 16 Brochure PDFJairo ManzanedaNo ratings yet
- Emergency Response Manual (Riot)Document7 pagesEmergency Response Manual (Riot)Kua Ming TeckNo ratings yet
- Gender Differences in AKI To CKD TransitionDocument13 pagesGender Differences in AKI To CKD TransitionNatasha AlbaShakiraNo ratings yet
- Capstone Assignment Critical Analysis EssayDocument5 pagesCapstone Assignment Critical Analysis EssaymarcoNo ratings yet
- The 28-Day Crossfit Program For BeginnersDocument2 pagesThe 28-Day Crossfit Program For BeginnersAditya Pratap SinghNo ratings yet
- Personal Philosophy Statement Assignment 2017Document2 pagesPersonal Philosophy Statement Assignment 2017api-538727441No ratings yet
- Parenting. Vol 1Document458 pagesParenting. Vol 1pbsood100% (2)