Professional Documents
Culture Documents
Pinocchio Syndrome
Uploaded by
Takeshi ClairOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pinocchio Syndrome
Uploaded by
Takeshi ClairCopyright:
Available Formats
936 96ournal of Neurology, Neurosurgery, and Psychiatry 1993;56:936-938
to be linked to the limbic lobe, whose excitability was probably enhanced by its compression by the meningioma. When the patient was lying he probably felt a particular emotion and this limbic stimulation may have triggered epileptic discharges in the amygdala. As in Collodi's tale, in which lies made Pinocchio's nose grow, our patient's lies became obvious for his interlocutors. As he was an "eurocrat", using lies to evoke the truth in adversarial EEC negotiations, it is thanks to carbamazepine that he has been able to work again. F SELLAL
LETTERS TO THE EDITOR
'Pinocchio syndrome': a peculiar form of reflex epilepsy?
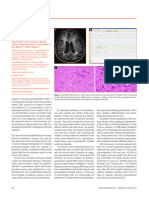
Reflex epilepsies can be defined as epilepsies in which all or a significant part of the seizures can be regularly provoked by a given triggering factor, most often a sensory stimulus. Sometimes it may be unexpected, such as, reading or decision-making.' We report a very unusual epilepsy in which seizures occurred when the patient lied. A 51 year old patient had recently experienced three attacks with loss of consciousness and generalised convulsions. Afterwards he was confused for a few minutes. These attacks started with sensations the patient had regularly felt several times each day, in clusters of one or two weeks for five years. They consisted of epigastric constriction, a sensation of hot flush rising from his stomach to his head, and then auditory and visual illusions, for instance sensation of hearing in echo or metamorphopsia, with intense anxiety. More than a third of the attacks occurred while the patient was lying, for business reasons. The other episodes occurred without any obvious triggering factor. An EEG showed a right anterior and temporal slowing but no epileptogenic activity. Cerebral MRI showed a meningioma, 30 mm in diameter, located on the right cavemous sinus wall and the anterior clinoid process, near the sella turcica (fig). It compressed the medial part of the right temporal lobe with a mass effect. No further attack has been reported since the introduction of carbamazepine therapy and then meningioma ablation. The attacks described fit with the diagnosis of partial vegetative seizures and the type of epilepsy fulfils the criteria of reflex epilepsy. Lying has not previously been described as a triggering factor of seizures but, according to certain authors, in some very rare cases seizures have been regularly provoked by emotion.'2 Emotions are said
Y CHEVALIER M COLIARD Neurology Sermice I, HMpitaux Universitaires de Strasbourg, I place de l'HMpital, 67091 Strasbourg Cedex, France
1 Beaumanoir A, Gastaut H, Naquet R. Reflex seizures and reflex epilepsies. Geneva: Editions Medecine et Hygiene, 1989:555. 2 Gastaut H, Tassinari CA. Triggering mechanisms in epilepsy. The electroclinical point of view. Epilepsia 1966;7:85-138.
Acute non-lymphoblast leukaemia presenting as a Guillain-Barr6 syndrome
Figure Tl weighted MRI scan after gadolinium injection, showing the meningioma and its effect on temporal lobe.
Peripheral nerve complications of acute leukaemia are uncommon. The neuropathy in these cases is frequently related to haemorrhage, into a nerve infarction or leukaemic infiltration.' Symmetrical peripheral neuropathy in acute leukaemia is much less common and other pathogenic factors could be involved.23 We report a very unusual case of acute non-lymphoblastic leukaemia presented initially as GuillainBarre syndrome. This 69 year old man developed symmetric paresthesiae and painful dysesthesiae of acute onset in the distal lower limbs. In the following days these symptoms increased in severity and he developed generalised progressive weakness, with greater involvement in the legs than in the arms. Four weeks after the appearance of the symptoms he went to a local hospital because he was unable to walk. Routine blood tests revealed severe abnormalities and the patient was immediately admitted to the haematological unit of a central hospital. On admission he was alert, well orientated and pale, and febrile. Blood pressure was 130/60, pulse rate 72/minute and respiratory rate 19/minute. Purpura, lymphadenopathy and hepatosplenomegaly were absent. There was generalised flaccid motor weakness of grade III/V (MRC) in the upper limbs and of grade I/V (MRC) in the lower limbs. Deep tendon reflexes were very much diminished in the arms and were absent in the legs. Pinprick sensation was symmetrically impaired in the lower limbs in a stocking distribution and was preserved in the arms. Joint position and vibration sense were impaired in the legs and preserved in the arms. Signs of meningeal irritation, corticospinal tracts, cranial nerves and autonomic involvement were absent. Higher mental function remained normal. The haemoglobin was 6-7 g/dl without reticulocytes. Leukocyte count was 49_000/mm3 with 6% polymorphonuclear neutrophils, 5% lymphocytes, 5% monocytes and 84% blast cells. The platelet count was 81-000/mm3. Bone marrow aspirate specimen showed increased cellularity due to
infiltration (67%) by blasts, Peroxidase + and 5% of promyelocytes. The haematological diagnosis was classified as acute nonlymphoblastic leukaemia, (FAB classification M2).4 Chemotherapy was immediately started and included daunorubicin 40 mg/M2 intravenously for three days and cytosine arabinoside 200 mg/M2 in continuous perfusion for seven days. A remission of the haematological measures was obtained with one therapeutic cycle, after a 22 day period of aplasia complicated with infection and gastrointestinal haemorrhage. Consolidation of the haematological remission was carried out 38 days after the induction, according to a similar protocol. As postremission therapy, cycles of cytosine arabinoside associated alternatively with VP16, 6-thioguanine and daunorubicin have been performed each month to date. Considering the severity of the haematological condition on admission and the emergency chemotherapy, lumbar puncture was delayed until nine weeks after the onset of the symptoms. CSF was clear and colourless, with normal opened pressure, cell count (one lymphocyte/mm3) and glucose concentration. A pure transudate was found with a protein content of 132 mg/dl (normal <50 mg/dl) and an albumin quotient (CSF/serum albumin x 103) of 38-2 (normal <9). Oligoclonal bands of gamma globulins in serum and CSF protein electrophoresis were not observed. There was no evidence of intrathecal immunoglobulin synthesis. Electrophysiological studies were first performed eight weeks after the onset of symptoms. Motor nerve conduction of median nerve was 38-4 ms-' (normal >48 ms-') with a distal motor latency of 4-1 (normal, up to 4-2). Distal sensory action potential was absent. Motor conduction velocity of peroneal nerve was 25 ms-' (normal >40 ms-') with a distal motor latency of 8-7 (normal, up to six). Electromyography of the abductor pollis brevis, tibialis anterior and extensor digitorium brevis muscles revealed a pattern of discrete activity with an increase of mean duration of individual motor unit potentials. Fibrillation potentials and positive waves were observed in these muscles. A sural nerve biopsy showed a mild perivascular mononuclear cell reaction in the endoneurium, and marked demyelination in several foci of nerve fascicles was observed. In addition, there was some axonal degeneration. Leukaemia cell infiltration or areas of necrosis were not present. A progressive improvement of the neurological picture was appearant nine weeks after the onset of symptoms. Thirteen weeks later, he was able to walk without assistance. Two months later, deep tendon reflexes were present though slightly decreased in the legs. Ten months after the onset of the symptoms, the neurological examination was normal and the patient now leads a normal social life and only complains of slight sporadic paresthesie in his feet. This patient had a neurological illness that fulfilled the criteria for the diagnosis of Guillain-Barre syndrome (GBS)5: he developed progressive areflexia and symmetrical weakness of all four limbs, and had characteristic CSF and electrophysiological features. The natural course of his neurological illness, with the phases of progression (four weeks), plateau (six weeks) and remission (40 weeks) was also typical of GBS.5 Cancer patients with GBS differ significantly from non-cancer patients by a more
You might also like
- Seronegative Myasthenia Gravis Presenting With PneumoniaDocument4 pagesSeronegative Myasthenia Gravis Presenting With PneumoniaJ. Ruben HermannNo ratings yet
- Neuro JournalDocument7 pagesNeuro JournalLannydchandraNo ratings yet
- Case ReportDocument5 pagesCase ReportsyahputriNo ratings yet
- Exercise-Associated Numbness and Tingling in The Legs: For Editorial Comment See Page 1509Document4 pagesExercise-Associated Numbness and Tingling in The Legs: For Editorial Comment See Page 1509herpthederpNo ratings yet
- Spinal Cord Injury Case StudyDocument8 pagesSpinal Cord Injury Case StudyMarius Clifford BilledoNo ratings yet
- Nursing Management of Seizures and EpilepsyDocument36 pagesNursing Management of Seizures and EpilepsyMatthew Ryan100% (6)
- 2014 Kabir Et Al. - Chronic Eosinophilic Leukaemia Presenting With A CDocument4 pages2014 Kabir Et Al. - Chronic Eosinophilic Leukaemia Presenting With A CPratyay HasanNo ratings yet
- Guillain Barr Syndrome Occurring Synchronously With Systemic Lupus Erythematosus As Initial Manifestation Treated Successfully With Low DoseDocument5 pagesGuillain Barr Syndrome Occurring Synchronously With Systemic Lupus Erythematosus As Initial Manifestation Treated Successfully With Low DoseTessa CruzNo ratings yet
- Cost of BC CareDocument7 pagesCost of BC CareErwin Chiquete, MD, PhDNo ratings yet
- Acute Pandysautonomia 1983Document9 pagesAcute Pandysautonomia 1983iri_balNo ratings yet
- Megaloblastic Anemia Case Report Focuses on Hypotension and DeliriumDocument5 pagesMegaloblastic Anemia Case Report Focuses on Hypotension and DeliriumNindy PutriNo ratings yet
- ECMO and Foot DropDocument31 pagesECMO and Foot DropAnon0123No ratings yet
- Archneur 23 2 003Document7 pagesArchneur 23 2 003Robert JenkinsNo ratings yet
- Bickerstaff Brainstem Encephalitis Diagnosis and TreatmentDocument7 pagesBickerstaff Brainstem Encephalitis Diagnosis and TreatmentAubrey Unique EvangelistaNo ratings yet
- Jurnal 1Document16 pagesJurnal 1Faisal Fitrah NasutionNo ratings yet
- Hypoglycemia The Great Chameleon A Pseudo NonconDocument3 pagesHypoglycemia The Great Chameleon A Pseudo NonconuchoaNo ratings yet
- Case Report: A Case of Herpes Simplex Virus-1 Encephalitis From A Medicolegal Point of ViewDocument4 pagesCase Report: A Case of Herpes Simplex Virus-1 Encephalitis From A Medicolegal Point of Viewzefri suhendarNo ratings yet
- Lecture 06.8 (Dr. Althekair's Lecture) - Common Peripheral NeuropathiesDocument68 pagesLecture 06.8 (Dr. Althekair's Lecture) - Common Peripheral NeuropathiesmaodNo ratings yet
- Neurology Multiple Choice Questions With Explanations: Volume IFrom EverandNeurology Multiple Choice Questions With Explanations: Volume IRating: 4 out of 5 stars4/5 (7)
- SDH HipotensionDocument4 pagesSDH HipotensiononaNo ratings yet
- Wasp StingDocument3 pagesWasp StingShruthi KyNo ratings yet
- Jurnal 4Document4 pagesJurnal 4Putri Maghfirah BahriNo ratings yet
- Articulo Polineuropatia 1Document3 pagesArticulo Polineuropatia 1Paula JoyaNo ratings yet
- Estado Epiléptico Parcial No Convulsivo Como Síntoma de Presentación de Encefalitis LímbicaDocument4 pagesEstado Epiléptico Parcial No Convulsivo Como Síntoma de Presentación de Encefalitis LímbicaNathaly CantorNo ratings yet
- Casos Clinicos NEJM 2018Document287 pagesCasos Clinicos NEJM 2018Eduarda RosasNo ratings yet
- Tuberculous Transverse Myelitis: Case Report and Review of The LiteratureDocument7 pagesTuberculous Transverse Myelitis: Case Report and Review of The LiteraturenoraNo ratings yet
- ADEM Case in Heart-Lung TransplantDocument4 pagesADEM Case in Heart-Lung TransplantRodrigo AriasNo ratings yet
- Bmjcred00647 0019Document3 pagesBmjcred00647 0019Vignesh SelvamNo ratings yet
- Cranial Neuropathies in Granulomatosis With PolyangiitisDocument6 pagesCranial Neuropathies in Granulomatosis With PolyangiitisMikeyNo ratings yet
- Síndrome de Lance-Adams: Presentación de Dos CasosDocument5 pagesSíndrome de Lance-Adams: Presentación de Dos Casosbrunotaciano8628No ratings yet
- Hypomagnesemia and Prolonged Hospital Stay: A Case Report and Literature ReviewDocument6 pagesHypomagnesemia and Prolonged Hospital Stay: A Case Report and Literature ReviewIJAR JOURNALNo ratings yet
- Acquired NeuropathiesDocument106 pagesAcquired NeuropathiesDanny J. BrouillardNo ratings yet
- Encefalitis Autoinmune 2011 PDFDocument11 pagesEncefalitis Autoinmune 2011 PDFDiana Vanessa SuarezNo ratings yet
- Two Rare Complications of Glioblastoma Multiforme: Persistent Hiccup and Acquired Haemophilia ADocument3 pagesTwo Rare Complications of Glioblastoma Multiforme: Persistent Hiccup and Acquired Haemophilia APradita Dhriti IndriyaniNo ratings yet
- CLL Case PresentationDocument17 pagesCLL Case PresentationAhmed EshraNo ratings yet
- Renal Failure With Multisystem ProblemsDocument7 pagesRenal Failure With Multisystem Problemscammel ramosNo ratings yet
- Posterior Reversible Encephalopathy Syndrome Secondary To Acute Post-Streptococcal Glomerulonephritis in A 12-Year-Old GirlDocument2 pagesPosterior Reversible Encephalopathy Syndrome Secondary To Acute Post-Streptococcal Glomerulonephritis in A 12-Year-Old GirlwawaningNo ratings yet
- 1 s2.0 S1389945717302496 Main PDFDocument3 pages1 s2.0 S1389945717302496 Main PDFvalentinaNo ratings yet
- Status Epilepticus: Current Understanding: D P, M A M C, D GR M C, G, M PDocument17 pagesStatus Epilepticus: Current Understanding: D P, M A M C, D GR M C, G, M PDMishraNo ratings yet
- Megalencephaly, polymicrogyria, polydactyly syndrome with rare MR findingsDocument3 pagesMegalencephaly, polymicrogyria, polydactyly syndrome with rare MR findingsAnonymous x4Ba2BNo ratings yet
- The Neurology of Eclampsia: Some Observations: Views and ReviewsDocument8 pagesThe Neurology of Eclampsia: Some Observations: Views and ReviewsFajar Rudy QimindraNo ratings yet
- Hashimoto EncephalopathyDocument37 pagesHashimoto EncephalopathyIbrahim IbrahimNo ratings yet
- Clinical CaseDocument6 pagesClinical Casedani_zurita_1No ratings yet
- Anestesia e Esclerose TuberosaDocument5 pagesAnestesia e Esclerose TuberosaMarina MelekNo ratings yet
- Convulsiones y HemianopsiaDocument2 pagesConvulsiones y HemianopsiadianisvillarrealNo ratings yet
- BH 010060 ENGDocument2 pagesBH 010060 ENGCarlosNo ratings yet
- Optic Neuropathy Without Retinopathy in AIDS and Cytomegalovirus InfectionDocument6 pagesOptic Neuropathy Without Retinopathy in AIDS and Cytomegalovirus InfectionJoyeeta DasNo ratings yet
- 2017 32 3 264 267 EngDocument4 pages2017 32 3 264 267 Engemmanuellagrace06No ratings yet
- Guillain-Barré SyndromeDocument21 pagesGuillain-Barré SyndromeZulkarnainBustamamNo ratings yet
- Hypokalemic Periodic ParalysisDocument21 pagesHypokalemic Periodic ParalysisVarun VarnNo ratings yet
- Encefalitis LimbicaDocument11 pagesEncefalitis LimbicaRandy UlloaNo ratings yet
- (1-3) Hypoglycemia Induced Hemichorea (HpogC) (IJGN) - Shashi PrakashDocument3 pages(1-3) Hypoglycemia Induced Hemichorea (HpogC) (IJGN) - Shashi Prakashneeraj2811No ratings yet
- Wallenberg SyndromeDocument6 pagesWallenberg SyndromeThiago SouzaNo ratings yet
- Brain Abscess Case: Drug Abuser with Endocarditis and HemiparesisDocument22 pagesBrain Abscess Case: Drug Abuser with Endocarditis and HemiparesisAariNo ratings yet
- Third Nerve PalsyDocument4 pagesThird Nerve Palsyمجاهد إسماعيل حسن حسينNo ratings yet
- Meyer 1995Document7 pagesMeyer 1995Rogério XavierNo ratings yet
- International Journal of Pharmaceutical Science Invention (IJPSI)Document3 pagesInternational Journal of Pharmaceutical Science Invention (IJPSI)inventionjournalsNo ratings yet
- Als LymeDocument2 pagesAls LymeChristine Anne HellmundNo ratings yet
- Subacute Transverse Myelitis Developed Depending On Lyme Disease: A Case ReportDocument3 pagesSubacute Transverse Myelitis Developed Depending On Lyme Disease: A Case ReportmuthmainnahNo ratings yet
- World03 30 16Document40 pagesWorld03 30 16The WorldNo ratings yet
- Ha Ema To PoiesisDocument38 pagesHa Ema To PoiesisEmma Joel OtaiNo ratings yet
- UrinalysisDocument16 pagesUrinalysisJestha Parayno De Vera100% (6)
- 2) Megaloblastic AnemiaDocument17 pages2) Megaloblastic AnemiaAndrea Aprilia100% (1)
- Plasmid-Mediated Resistance - WikipediaDocument16 pagesPlasmid-Mediated Resistance - WikipediaUbaid AliNo ratings yet
- 01 - Chance - Fletcher, Clinical Epidemiology The Essentials, 5th EditionDocument19 pages01 - Chance - Fletcher, Clinical Epidemiology The Essentials, 5th EditionDaniel PalmaNo ratings yet
- CBD Sirosis, Hematemesis MelenaDocument29 pagesCBD Sirosis, Hematemesis Melenadyah farahNo ratings yet
- Blessing IwezueDocument3 pagesBlessing Iwezueanon-792990100% (2)
- Alconfactsheet CenturionDocument3 pagesAlconfactsheet Centurionsudhakar.mrNo ratings yet
- Unit 5 Drugs Acting On The Immune SystemDocument30 pagesUnit 5 Drugs Acting On The Immune SystemBea Bianca Cruz100% (1)
- Failures in Periodontal Therapy: Review ArticleDocument6 pagesFailures in Periodontal Therapy: Review ArticlezinniaNo ratings yet
- Estevan Jimenez Patient Clinical Report ForDocument7 pagesEstevan Jimenez Patient Clinical Report ForIsrael MelloNo ratings yet
- Refacere Dinti Frontali Cu Cape de CeluloidDocument5 pagesRefacere Dinti Frontali Cu Cape de CeluloidSorina NeamțuNo ratings yet
- Breast Assessment Learning ObjectivesDocument6 pagesBreast Assessment Learning Objectivesalphabennydelta4468No ratings yet
- Tuberculosis and Typhoid: Deadly Diseases in the PhilippinesDocument37 pagesTuberculosis and Typhoid: Deadly Diseases in the PhilippinesAriel FuentespinaNo ratings yet
- Positioning: The Battle For Your MindDocument30 pagesPositioning: The Battle For Your Mindjayson RebeiroNo ratings yet
- Errata: Shadow of The Demon LordDocument3 pagesErrata: Shadow of The Demon LordKaio CorsatoNo ratings yet
- UN AIDS Miles-To-Go - enDocument268 pagesUN AIDS Miles-To-Go - ensofiabloem100% (1)
- Rejected Application FinalDocument28 pagesRejected Application FinalJithin JayanNo ratings yet
- Fluconazole Final Dossier - Enrollemt Number 2Document139 pagesFluconazole Final Dossier - Enrollemt Number 2lathasunil1976No ratings yet
- Cirugia BariatricaDocument9 pagesCirugia BariatricaedwardmenesesNo ratings yet
- Latihan Un Bahasa Inggris 2018: The Following Text Is For Questions 1 and 2Document9 pagesLatihan Un Bahasa Inggris 2018: The Following Text Is For Questions 1 and 2AWDNo ratings yet
- Spectrophotometric determination of total phenolic content in Gul-e-ZoofaDocument4 pagesSpectrophotometric determination of total phenolic content in Gul-e-Zoofayulyansyah susantoNo ratings yet
- Clinical Guidelines For Treating Caries in Adults Following A Minimal Intervention Policy-Evidence and Consensus Based Report PDFDocument11 pagesClinical Guidelines For Treating Caries in Adults Following A Minimal Intervention Policy-Evidence and Consensus Based Report PDFFabian ArangoNo ratings yet
- Gordon Functional Health AssessmentDocument18 pagesGordon Functional Health Assessmentjokazel100% (1)
- And Technical Description: User ManualDocument100 pagesAnd Technical Description: User ManualYouness Ben TibariNo ratings yet
- Siddha Therapeutic Index - 18-Article Text-133-1-10-20210308Document7 pagesSiddha Therapeutic Index - 18-Article Text-133-1-10-20210308Dr.kali.vijay kumkarNo ratings yet
- Drugs & Cosmetics ActDocument70 pagesDrugs & Cosmetics ActAnonymous ibmeej9No ratings yet
- Acute Myocardial InfarctionDocument35 pagesAcute Myocardial Infarctionvirnzrobz80% (10)
- DOH Forms Streamlined for Easier Health Facility LicensingDocument5 pagesDOH Forms Streamlined for Easier Health Facility LicensingMenGuitar100% (3)