Professional Documents
Culture Documents
BELL Final
Uploaded by
Emiaj KhalimOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
BELL Final
Uploaded by
Emiaj KhalimCopyright:
Available Formats
BELLS PALSY
Definition: also known as idiopathic facial paralysis is a dysfunction of cranial nerve VII (the facial nerve) that results in inability to control facial muscles on the affected side. Several conditions can cause a facial paralysis, e.g., brain tumor, stroke, and Lyme disease. However, if no specific cause can be identified, the condition is known as Bell's palsy. named after Scottish anatomist Charles Bell, who first described it, Bell's palsy is the most common acutemononeuropathy (disease involving only one nerve) and is the most common cause of acute facial nerve paralysis. it is defined as an idiopathic unilateral facial nerve paralysis, usually self-limiting. The trademark is rapid onset of partial or complete palsy, usually in a single day. It can occur bilaterally resulting in total facial paralysis in around 1% of cases. Causes: cause of the nerve irritation associated with Bells palsy is unknown. Anecdotally, exposure to cold is a frequently cited cause for example, driving with a car window open in frigid weather, or sleeping with the window open on a chilly night. inflammation of cranial nerve VII triggered by a viral infection,- the herpes family. cases have recently been reported after administration of intranasal influenza vaccine. trauma, hemorrhage, meningitis, tumor.
Epidemiology: disorders of the facial nerve can occur to men, women, and children, but they are more prominent among men and women over 40 years of age, people with diabetes, upper respiratory ailments, weak immune systems, or pregnant women. Cases of facial paralysis can be permanent or temporary, but in all circumstances there are treatments designed to improve facial function.
three times more likely to strike pregnant women. it is also considered to be four times more likely to occur in diabetics than the general population. a range of annual incidence rates have been reported in the literature: 15, 24, and 25-53 (all rates per 100,000 population per year).
Signs and Symptoms: The classic presentation of Bell's palsy is weakness on one side of the face. The potential range of weakness is wide it may range from difficulty blinking all the way to a complete paralysis on one side of the face with an inability to close the eye. Onset usually occurs acutely, but the weakness may worsen for 24 to 48 hours before stabilizing. The first awareness of the problem may involve drooling after brushing the teeth or when drinking, an asymmetrical appearance of the mouth noticed in the mirror, an inability to whistle, or excessive tearing in one eye. A man may say that he was unable to blow out his cheeks when shaving. People with Bell's palsy may describe the sensation of unilateral loss of facial movement as deadness, loss of feeling, or numbness, although the affected part of the face is neither asleep nor tingling. Alteration of taste or hearing is occasionally a symptom. Others:
Twitching Weakness or paralysis of face Dryness of the eye or mouth Disturbance or loss of taste Drooping eyelid or corner of the mouth Difficulty in speaking Dribbling when drinking or after cleaning teeth Ear pain
It is important to remember that facial paralysis does not always mean an individual has Bells palsy. Other diagnoses should be considered, especially stroke, Lyme disease, and varicella zoster (Ramsey Hunt syndrome). Less common causes include HIV infection, sarcoidosis, Sjgrens syndrome, amyloidosis, and tumors. Only a physician can distinguish among these possibilities by performing a careful examination.
Anatomy and Physiology:
Facial nerve: the facial nerve's nuclei are in the brainstem (they are represented in the diagram as a ). Orange: nerves coming from the left hemisphere of the brain. Yellow: nerves coming from the right hemisphere of the brain. Note that the forehead muscles receive innervation from both hemispheres of the brain (represented in yellow and orange). The facial nerve resembles a telephone cable and contains 7,000 individual nerve fibers. Each fiber carries electrical impulses to a specific facial muscle. Information passing along the fibers of this nerve allows us to laugh, cry, smile, or frown, hence the name, the nerve of facial expression. When half or more of these individual nerve fibers are interrupted, facial weakness occurs. If these nerve fibers are irritated, then movements of the facial muscles appear as spasms or twitching. The facial nerve not only carries nerve
impulses to the muscles of the face, but also to the tear glands, to the saliva glands, and to the muscle of the stirrup bone in the middle ear (the stapes). It also transmits taste from the front of the tongue. Since the function of the facial nerve is so complex, many symptoms may occur when the fibers of the facial nerve are disrupted. A disorder of the facial nerve may result in twitching, weakness, or paralysis of the face, dryness of the eye or the mouth, or disturbance of taste.
Facial nerve affects facial expression: The facial nerve passes through the base of the skull in transit from the brain to the muscles that control facial expressions. After leaving the brain, the facial nerve enters the temporal bone through the internal auditory canal, a small bony tube, in very close association with the hearing and balance nerves. Along its inch-and-a-half course through a small canal within the temporal bone, the facial nerve winds around the three middle ear bones, in back of the eardrum, and then through the mastoid (the bony area behind the part of the ear that is visible). After the facial nerve leaves the mastoid, it passes through the salivary or parotid gland and divides into many branches. The facial nerve has four components with several distinct functions: facial expression, taste sensation, skin sensation, and saliva and tear production.
Pathophysiology: Possible causes: tumor, meningitis, stroke, diabetes mellitus, head trauma and inflammatory diseases of the cranial nerves (sarcoidosis, brucellosis), vascular ischemia, viral infections (Herpes Simplex Virus) Inflammation of the seventh cranial nerve(Facial Nerve) Inflamed and edematous nerve becomes compressed to the point of damage. Blood supply is occluded.
Transmission of the neural signals blocked. Ischemic necrosis of the nerve. Weakness or paralysis of the facial muscles as manifested by: o Lacrimation(tearing);
o Painful sensation in the face, behind the ear and the eye; o Speech difficulties; o Eating difficulties.
Diagnostic Tests and Examinations: Since otolaryngologistshead and neck surgeons have special training and experience in managing facial nerve disorders, they are the most qualified physicians to perform an in-depth evaluation of abnormal movement or paralysis of the face. An evaluation will include an examination of the head, neck, and ears, as well as a series of tests. Some of the most commonly used tests are:
Hearing Test - determines if the cause of damage to the nerve has involved the hearing nerve, inner ear, or delicate hearing mechanism.
Balance Test - evaluates balance nerve involvement. Tear Test - measures the eyes ability to produce tears. Eye drops may be necessary to prevent drying of the surface of the eye (cornea).
Imaging CT (computerized tomography) or MRI (magnetic resonance imaging determines if there is an infection, tumor, bone fracture, or other abnormality in the area of the facial nerve.
Electrical Test - stimulates the facial nerve to assess how badly the nerve is damaged. This test may have to be repeated at frequent intervals to see if the disease is progressing.
Treatment: (Medical and Surgucal) The results of diagnostic testing will determine treatment. The goal of the treatment is to eliminate the source of the nerve damage. Patients with less nerve damage have better chances of recovery. Medications are often used as part of the treatment:
If infection is the cause, then an antibiotic to fight bacteria (as in middle ear infections) or antiviral agents (to fight syndromes caused by viruses like Ramsay Hunt) may be used; Acyclovir for viral infections.
If swelling is believed to be responsible for the facial nerve disorder, then steroids are often prescribed; Prednisone as an anti-inflammatory drug.
In certain circumstances, surgical removal of the bone around the nerve (decompression surgery) may be appropriate.
Treatments for permanent facial paralysis Patients with a permanent facial paralysis may be rehabilitated through a variety of procedures including:
Eyelid weights or springs Muscle transfers and nerve substitutions A special form of physical therapy called facial retraining Weakening the paralysis by chemical injection
Nursing Interventions:
i. ii. iii. iv. v. vi.
Exercise the facial muscles in front of a mirror. Massage the face. Apply gentle heat to reduce pain. Using a finger, regularly close the eye to keep it moist. Tape the eye closed for sleeping. Use protective glasses or clear eye patches to keep the eye moist and to keep foreign materials from entering the eye.
vii.
Use doctor-recommended artificial tears or an ointment to keep the eye moist.
viii.
Teaching the eye care Because the blink reflex is diminished, the involved eye may not close completely and the needs to be protected to prevent corneal irritation and ulceration. Inform the patient of potential complications, including corneal irritation and ulceration, overflow of tears, and absence of blink reflex. Key teaching points include: Cover the eye with a protective shield at night. Apply eye ointment to keep eyelids closed during sleep. Close the paralyzed eyelid manually before going to sleep. Wear wrap-around sunglasses or goggles to decrease normal evaporation from the eye.
ix.
Teaching about maintaining muscle tone. Show patient how to perform facial massage which gentle upward motion several times daily when the patient can tolerate the massage. Demonstrate the facial exercises, such as wrinkling the forehead, blowing out the cheeks, and whistling in an effort to prevent muscle atrophy. Instruct patient to avoid exposing the face to cold and drafts. Remind patient and family of the importance of participating in health promotion activities and recommended health screening practices.
Prognosis: Even without any treatment, Bell's palsy tends to carry a good prognosis. There are studies that proved I, these are the following: a. In a 1982 study, when no treatment was available, of 1,011 patients, 85% showed first signs of recovery within 3 weeks after onset. For the other 15%, recovery occurred 36 months later. After a follow-up of at least 1 year or until restoration, complete recovery had occurred in more than two thirds (71%) of all patients. Recovery was judged moderate in 12% and poor in only 4% of patients. b. Another study found that incomplete palsies disappear entirely, nearly always in the course of one month. The patients who regain movement within the first two
weeks nearly always remit entirely. When remission does not occur until the third week or later, a significantly greater part of the patients develop sequelae. c. A third study found a better prognosis for young patients, aged below 10 years old, while the patients over 61 years old presented a worse prognosis. Complications: chronic loss of taste (ageusia) chronic facial spasm corneal infections. incomplete or erroneous regeneration of the damaged facial nerve crocodile tear syndrome, also called gustatolacrimal reflex or Bogorads Syndrome, on recovery, where they will shed tears while eating. This is thought to be due to faulty regeneration of the facial nerve, a branch of which controls the lacrimal and salivary glands. Gustatorial sweating can also occur.
IMAGES:
You might also like
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (587)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (399)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (73)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (119)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- Intrauterine InfectionDocument64 pagesIntrauterine Infectionthapan87100% (1)
- 23 Avian Leukosis Complex 1Document14 pages23 Avian Leukosis Complex 1Aqib HussainNo ratings yet
- Awareness Session: Current Novel Corona Virus (Covid 19)Document8 pagesAwareness Session: Current Novel Corona Virus (Covid 19)danishali03No ratings yet
- Assessment Diagnosis Planning Implementation Rationale Evaluation Subjective Data: Short Term: Independent: Short Term: Goal Partially MetDocument3 pagesAssessment Diagnosis Planning Implementation Rationale Evaluation Subjective Data: Short Term: Independent: Short Term: Goal Partially MetPrincess Mildred AbdonNo ratings yet
- Hiv CounsellingDocument73 pagesHiv Counsellingomotayofaith360No ratings yet
- Clinical Prevention and Population Health Diabetes in African Americans Power PointDocument23 pagesClinical Prevention and Population Health Diabetes in African Americans Power Pointapi-623608782No ratings yet
- Pathology Ple SamplexDocument5 pagesPathology Ple SamplexdawnparkNo ratings yet
- Cohort Study Hansana PDFDocument28 pagesCohort Study Hansana PDFTukai KulkarniNo ratings yet
- Jurnal Triangle SpiderDocument17 pagesJurnal Triangle SpiderZuhdi Mahendra KotoNo ratings yet
- Neonatal Sepsis, Opthalmia Neonatarum & HIV/AIDSDocument15 pagesNeonatal Sepsis, Opthalmia Neonatarum & HIV/AIDSSAKSHI RANANo ratings yet
- Med&upd&vol 31&2021Document1,525 pagesMed&upd&vol 31&2021Rajesh KumarNo ratings yet
- MCCD Training ModuleDocument90 pagesMCCD Training ModuleAashish PatniNo ratings yet
- English Language Dialogue On HIVDocument5 pagesEnglish Language Dialogue On HIVAFRI YUNIKANo ratings yet
- Black Hairy TongueDocument2 pagesBlack Hairy TongueFadhlih MuhammadNo ratings yet
- Carolyn R. Zalameda-Castro, MDDocument9 pagesCarolyn R. Zalameda-Castro, MDeza floresNo ratings yet
- Computer-Based English Proficiency Test AdvisoryDocument7 pagesComputer-Based English Proficiency Test AdvisoryJoyce CarilloNo ratings yet
- Ethical Issues in Mandatory Smallpox VaccinationDocument2 pagesEthical Issues in Mandatory Smallpox VaccinationFaizaNadeemNo ratings yet
- Causal thinking and complex systems approaches in epidemiologyDocument10 pagesCausal thinking and complex systems approaches in epidemiologyPrevencion AtencionNo ratings yet
- Pathophysiology: Tonsillitis Is Inflammation of The Tonsils, Two OvalDocument13 pagesPathophysiology: Tonsillitis Is Inflammation of The Tonsils, Two Ovalyangi doka100% (1)
- Framingham Data Famous Cohort Study of 5209 Subjects From Framingham MADocument2 pagesFramingham Data Famous Cohort Study of 5209 Subjects From Framingham MAEdwin Johny Asnate SalazarNo ratings yet
- Consent FormDocument1 pageConsent FormJulius CagampangNo ratings yet
- Pediatric SmleDocument59 pagesPediatric SmleMoayad Zeyad M100% (1)
- Encefalitis ViralDocument5 pagesEncefalitis ViralRandy UlloaNo ratings yet
- Sample: Extract 1: Questions 31-36Document5 pagesSample: Extract 1: Questions 31-36Jorge VegaNo ratings yet
- Malignant Struma OvariiDocument4 pagesMalignant Struma Ovariixwahyu 108No ratings yet
- GCSE Biology - Health and Disease - WorksheetDocument2 pagesGCSE Biology - Health and Disease - WorksheetVeenaNo ratings yet
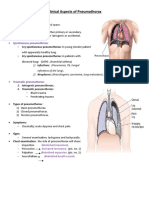
- Clinical Aspects of PneumothoraxDocument3 pagesClinical Aspects of PneumothoraxelisabethNo ratings yet
- IAHS Immunization in TanzaniaDocument5 pagesIAHS Immunization in TanzaniaMasali MacdonaNo ratings yet
- The Lasting Impact of Covid-19 2Document4 pagesThe Lasting Impact of Covid-19 2api-650392913No ratings yet
- M1.U1. TutorialDocument7 pagesM1.U1. TutorialRizki DiniNo ratings yet